DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Common skin lesions Non-surgical physical treatments CME
Common skin lesions
Non-surgical physical treatments
Created 2008.
Learning objectives
- Describe the use of physical therapies in the treatment of skin lesions including cryotherapy, radiotherapy, photodynamic therapy, laser and pulsed light therapy.
Introduction
Physical therapy of skin diseases refers to treatment that employs heat, cold, ionising and non-ionising radiation.
Cryotherapy
Cryotherapy is used to reduce or remove superficial skin lesions, including:
- Actinic keratoses
- Seborrhoeic keratoses
- Benign lentigines
- Viral warts
- Skin tags
- Molluscum contagiosum
Using a special technique, it may also be used to treat superficial non-melanoma skin cancers. Cryotherapy should not be used if there is any doubt about the pathology of the lesion, especially if melanoma is within the differential diagnosis.
Although well tolerated by adults, treatment stings and is inappropriate in young children unless unavoidable.
Liquid nitrogen (boiling point –196C) is the most useful cryogen. It can be delivered to medical practices at low cost (e.g. $2/litre) as required. It should be stored in an purpose-designed Dewar. The most popular are 20-litre vacuum tanks that can hold unused liquid nitrogen for up to several months. The tanks may last 10 or 20 years but do eventually suddenly or slowly lose their vacuum. The nitrogen may be carefully poured into a smaller container or a special withdrawal tube may be used.
It is dangerous to store nitrogen in a glass thermos as this may explode destructively if inadvertently sealed. A steel flask is necessary and there must always be a release valve.
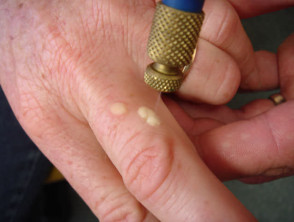
Cryotherapy
Nitrogen can be applied to the lesion using a loose hand-made cotton-tip swab, but it may be difficult to be accurate. The swab should not be re-dipped into the nitrogen flask as viral particles may be transmitted. Instead, use a new swab or pour nitrogen into an insulated small container that is single-use or sterilised between patients.
A hand-held spray unit is much more convenient and accurate, providing a constant fine jet of liquid nitrogen. Different size spray nozzles, adapters and probes are available for different sized lesions in different sites. The tip of a spray nozzle should be held about 1 cm away from the skin surface and perpendicular to it. The lever is gently and repetitively squeezed to maintain a constant area of freeze up to 1 cm in diameter.
The diameter of the freeze may be confined to the lesion (seborrhoeic keratoses, actinic keratoses, molluscum contagiosum) or include 1 mm of surrounding normal skin (viral warts). Benign superficial skin lesions may resolve with freeze/thaw times of 5 to 30 seconds depending on the depth of the lesion.
Effective cryotherapy of malignant lesions requires training and experience, and a wider margin (most recurrences after cryotherapy arise on the periphery of a lesion because the freeze failed to reach sufficiently low temperature). Longer freezes cause deeper damage and greater morbidity. Tissue injury depends on the rate of cooling, minimal temperature reached and freeze/thaw time. A temperature of –30 to -50C ensures destruction of malignant cells, particularly if the freeze/thaw cycle is repeated.
Adverse reactions include:
- Short term blistering, exudation, haemorrhage, ulceration
- Long term adnexal damage, anaesthesia, hypopigmentation and (rarely) scarring
Cryotherapy
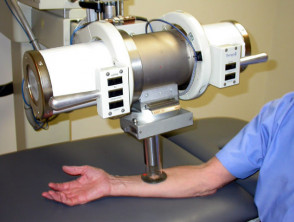
Radiotherapy
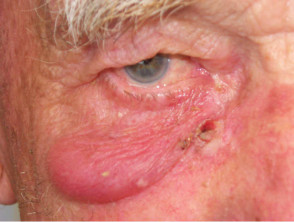
Radiotherapy is the use of ionising radiation to treat skin diseases. Although frequently used in the 1960's and 70's to treat benign and malignant skin conditions, radiotherapy is rarely recommended nowadays because of the risk of the development of further malignancies and poor long term cosmetic results.
Current indications for radiotherapy of skin disease include:
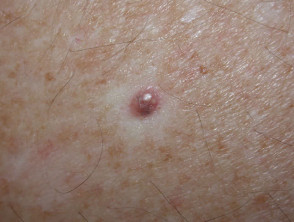
- Some basal cell and squamous cell cancers in the elderly
- Some lymphomas
- Rarely, intractable localised inflammatory skin disease.
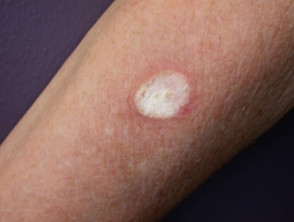
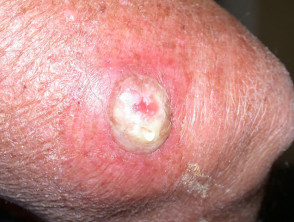
Malignant skin lesions are treated with multiple fractions of superficial X-rays delivered over two or three weeks. Treated areas become inflamed and may ulcerate before healing. Eventual scars tend to have a waxy atrophic appearance with telangiectasia and a tendency to break down with minor injury.
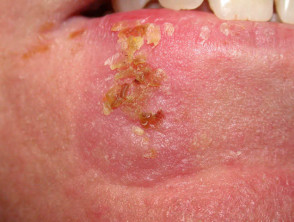
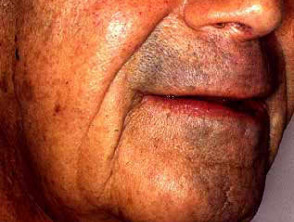
Cutaneous reactions to radiotherapy
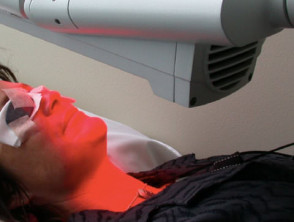
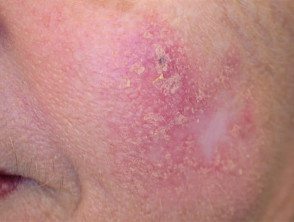
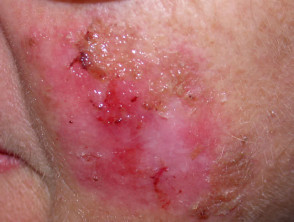
Photodynamic therapy
Photodynamic therapy (PDT) involves an oxygen-dependent phototoxic reaction and is used to treat superficial forms of non-melanoma skin cancer and other skin conditions. The photosensitiser (usually a porphyrin) can be given intravenously or can be applied to the target lesion topically (most often methyl aminolevulinate). It is selectively localised in the target tissue and is later illuminated with visible light (often 611 nm with a diode source), resulting in photodamage and subsequent cell death.
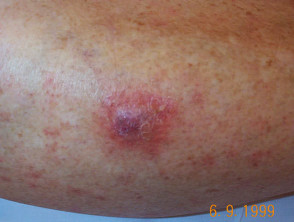
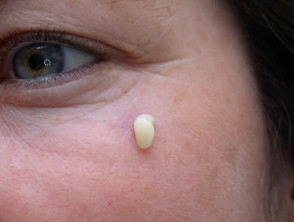
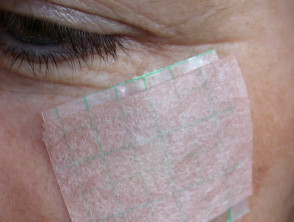
Photodynamic therapy
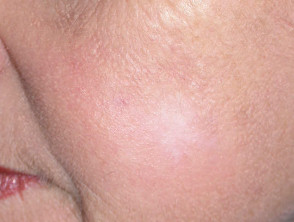
There is minimal damage to surrounding normal tissue hence side effects are limited to the target area. As a rule, cosmetic results are good or excellent.
Photodynamic therapy
Lasers
Lasers were first used in New Zealand in the 1980's to treat vascular birthmarks (port wine stains). The word 'laser' is an acronym for Light Amplification by Stimulated Emission of Radiation. Current therapeutic lasers remain expensive and hence are restricted to a small number of dermatology and cosmetic medicine practices in major centres.
The important properties of laser light are:
- Monochromatic (single wavelength)
- Collimated (parallel beam)
- Coherent (in phase)
- Continuous wave or pulsed (to reduce transmission of heat to surrounding tissues)
Different models are now commonly used to treat the following type of skin lesion:
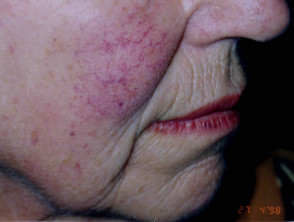
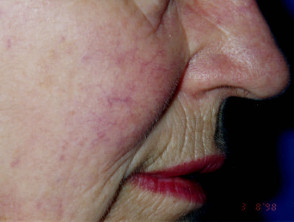
- Red lesions: yellow light to remove facial telangiectasia and vascular birthmarks;
- Brown lesions: green or red light to remove freckles and pigmentation;
- Tattoos: various wavelengths are required to remove different colours;
- Epidermal lesions (skin tags, viral warts, seborrhoeic keratoses): a bloodless knife;
- Facial resurfacing; vaporisation by carbon dioxide or erbium lasers;
- Scar revision;
- Epilation: hair removal and permanent reduction of dark hairs using various wavelengths.
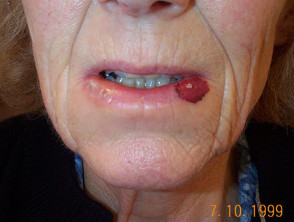
Vascular laser treatment
Advantages of laser treatment include:
- More precise hence less risk of damage to other tissues or scarring;
- For some indications, it is more effective than other known treatments;
- It may be quicker or more convenient than other treatments.
Microwaves and non-coherent broadband flash lamps are also available for hair removal. A flash lamp may also be useful to treat vascular lesions and for non-ablative rejuvenation of the skin (dermal remodelling). Radiofrequency devices may also tighten lax tissues to a modest degree.
Interested practitioners should undertake a laser safety course and carefully evaluate the range of devices available. A viable business depends on the local market, capital and running costs of equipment and staff and efficacy.
Activity
Undertake practical training in cryotherapy (ask your local dermatologist) or purchase a training video / CD-ROM.
Related information
References:
On DermNet NZ:
Liquid nitrogen/cryotherapy guidelines
Information for patients
Other websites:
- Brymill: Cryogenic systems
- Medscape: Topical Photodynamic Therapy in Clinical Dermatology
- Medscape Reference: Physical modalities including laser
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.