DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Scaly skin diseases Disorders of keratinisation CME
Scaly skin diseases
Disorders of keratinisation
Created 2009.
Learning objectives
- Describe common features of lichen planus, lichen sclerosus, ichthyosis, pityriasis rubra pilaris, Darier disease and keratosis pilaris
Lichenoid diseases
Many skin diseases include the term ‘lichen’, which is thought to originate from a resemblance to the lichen that is found on trees.
- Idiopathic lichen planus
- Erosive lichen planus
- Lichenoid drug eruption
- Lichen sclerosus
Lichen simplex is a type of eczema and was discussed in the dermatitis section of this course. There are several other uncommon “lichen” conditions that will not be considered in this course.
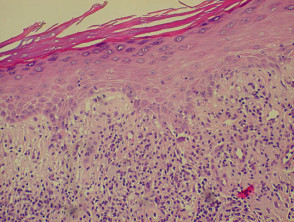
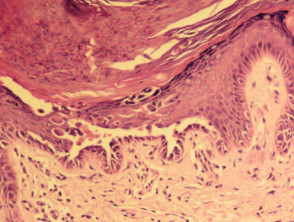
Lichenoid histology refers to liquefaction degeneration of basal layer, dermal infiltration of inflammatory cells hugging the basal layer, colloid bodies (degenerating keratinocytes) and dermal melanin.
Lichenoid histology
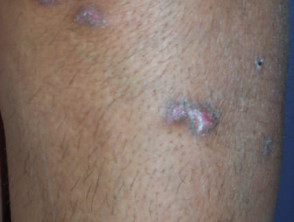
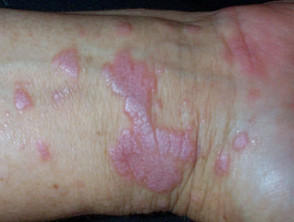
Idiopathic lichen planus has the following features:
- An occasional association with primary biliary cirrhosis, hepatitis-C and perhaps other liver diseases
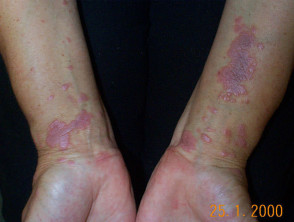
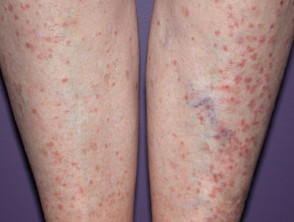
- Polygonal papules and plaques on ventral wrists, forearms and legs
- Lacy pattern of white marks on buccal mucosa &/or genitals
- Variable itching
- Koebnerisation (lichen planus arising in areas of minor skin trauma such as excoriation)
- Nail dystrophy (uncommon)
Follicular lichen planus (lichen planopilaris) results in perifollicular erythema and scaling in the scalp and other hair bearing areas. It may or may not arise in association with non-follicular or mucosal disease.
Lichen planus
Treatment of lichen planus may include:
- Potent topical steroids
- Systemic steroids
- Sometimes, immune suppressive agents or retinoids.
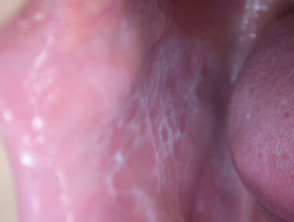
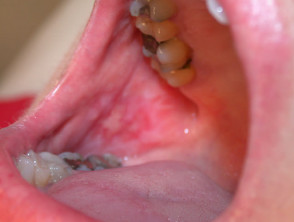
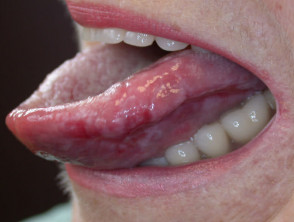
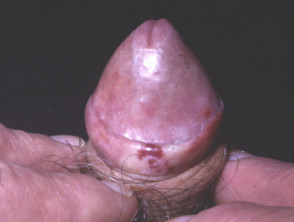
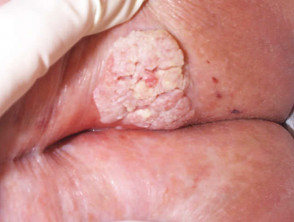
Erosive lichen planus affects the oral and/or genital mucosa. It may result in very painful ulceration and scarring.
Erosive lichen planus
Lichenoid drug eruption has similar histology, and sometimes clinical appearance. More often there is a diffuse eruption of mildly irritable flat dry patches on trunk and limbs. Common causes include thiazides, anti-malarials, gold and ACE inhibitors.
Chronic graft-versus-host disease (GVHD) also has lichenoid histology. Arising more than 100 days after bone marrow transplantation, there are lichen planus-like papules and dermal sclerosis.
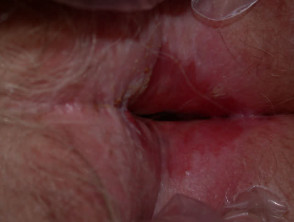
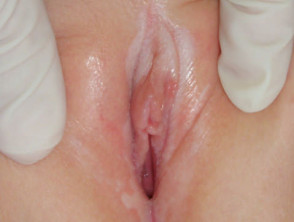
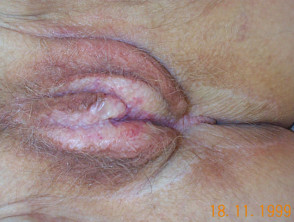
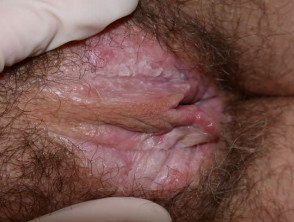
Lichen sclerosus is a common cause of vulval itching and soreness in menopausal women. Only ten percent of cases affect other sites or men. It is thought to have an autoimmune origin, with an extracellular matrix protein as antigen. On the vulva, perineum and perianal mucosa, it causes white plaques, atrophy, sclerosis (scarring), haemorrhage, blistering and ulceration. In children, it is often confused with the results of sexual abuse.
Lichen sclerosus
Patients with lichen sclerosus should be under the care of a dermatologist. Ultrapotent topical steroids are generally successful but should be used with caution because of potential adverse effects.
Ichthyosis
Ichthyosis refers to a group of disorders of keratinisation characterised by excessively dry and scaly skin (abnormal differentiation and desquamation of the epidermis). Genetic analysis is identifying the protein abnormality responsible in specific subtypes.
The most common types of ichthyosis are:
Autosomal dominant ichthyosis vulgaris
- The most common type (1:250)
- Histology: absent granular layer
- Most severe in childhood but may persist in adult life
- Predisposes to atopic dermatitis
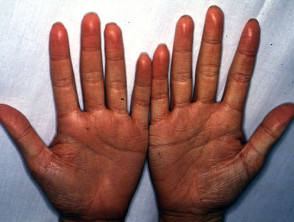
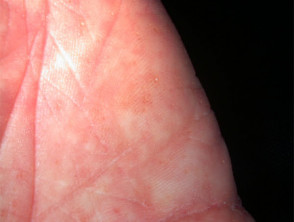
- Generalised dryness most prominent on upper arms
- May have hyperlinear palms
Autosomal recessive lamellar ichthyosis
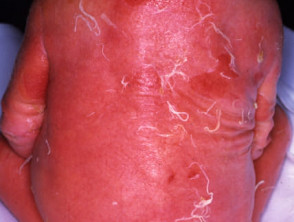
- Collodion baby (neonate encased in a membrane)
- Extensive scaling on erythematous base
- Mutation in gene coding for glutaminase (and other mutations)
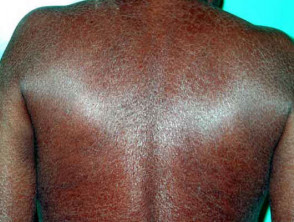
X-linked recessive ichthyosis
- Deficiency of steroid sulphatase in affected child and carrier mother
- Large scales on trunk and limbs
- Flexures may be spared
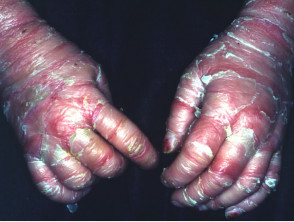
Bullous ichthyosiform erythroderma
- Blistering and erythematous skin in infants
- Prominent scaling on erythematous base in adults
- Autosomal dominant mutation in keratin 1 and 10
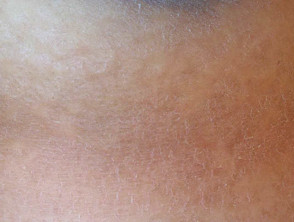
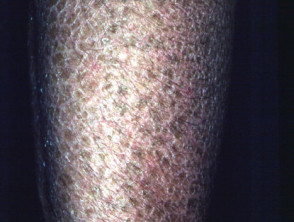
Acquired ichthyosis is the dry skin associated with cachexia and certain forms of cancer and lymphoma. It is also characteristic in heavy consumers of kava.
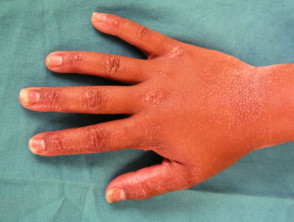
Ichthyosis
Treatment of ichthyosis requires regular application of emollients containing urea and/or lactic acid and the use of soap substitutes when bathing. Oral retinoids may be prescribed for severe cases.
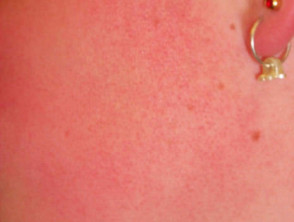
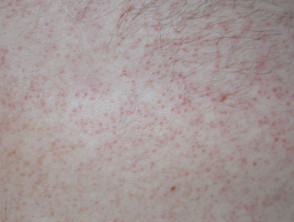
Keratosis pilaris
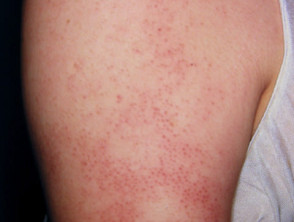
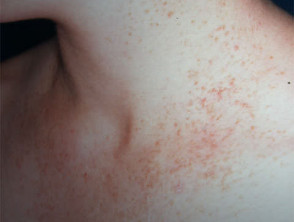
Keratosis pilaris affects up to 50% of adolescents and may present from neonate to middle-age.
- Common sites are outer aspect of upper arms and anterior thighs
- The rough skin is due to follicular plugs of keratin
- May result in non-pruritic erythema (keratosis rubra pilaris)
- Rarely causes loss of the lateral eyebrows (ulerythema oophyrogenes)
- May cause red dry cheeks (keratosis pilaris faciei)
Keratosis pilaris
Keratosis pilaris rarely clears with treatment. Urea-containing emollients may soften the affected areas. Topical retinoids encourage normal follicular keratinisation with improvement in the appearance in some patients but may irritate.
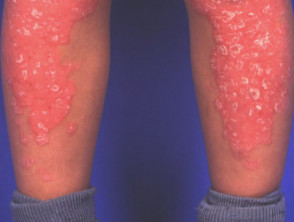
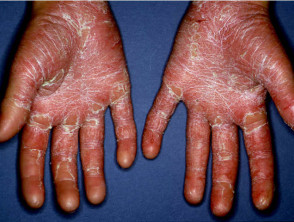
Pityriasis rubra pilaris
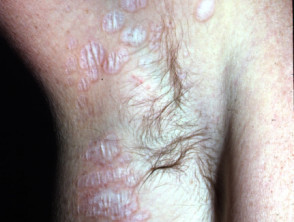
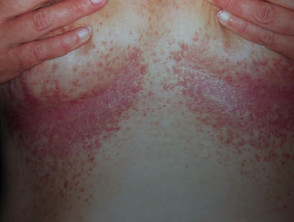
Pityriasis rubra pilaris (PRP) is the name given to a group of rare skin disorders resulting in localised erythematous scaly plaques rather like psoriasis. However there is less scaling and prominent follicular involvement. Keratoderma of palms and soles is usual. Both juvenile and adult types may result in erythroderma.
Pityriasis rubra pilaris
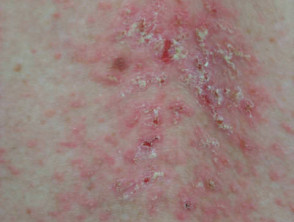
Darier disease
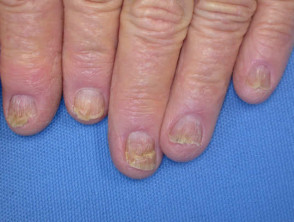
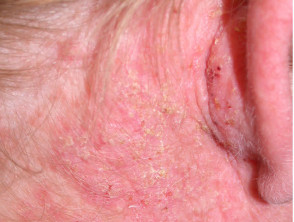
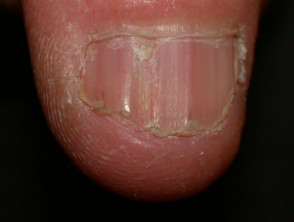
An uncommon inherited disorder with disordered keratinisation, resulting in characteristic greasy reddish papules in scalp and trunk, palmar pitting and nail changes. The onset of skin lesions is generally during adolescence. Darier disease may be complicated by sunburn, staphylococcal infection, and herpes simplex virus infection
Darier disease
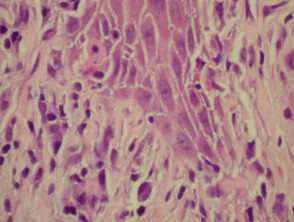
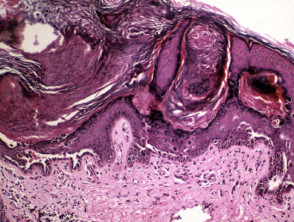
Darier histology has the following features:
- Hyperkeratosis, papillomatosis and acanthosis
- Acantholytic dyskeratotic kerinocytes (‘corps ronds’ and ‘grains’)
- Suprabasal lefts or lacunae due to acantholysis
Darier histology
Activity
Review the molecular genetics of keratin disorders.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Dermatology topics
- Merck Manual Professional:
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.