DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Scaly skin diseases Phototherapy CME
Scaly skin diseases
Phototherapy
Created 2009.
Learning objectives
- Describe indications for phototherapy and photochemotherapy and their common complications
Introduction
Phototherapy is the use of non-ionising portions of the electromagnetic spectrum for its therapeutic effect. It may involve partial or whole-body exposure. In dermatology, the term phototherapy is usually applied to the use of ultraviolet (UV) radiation in the treatment of skin diseases.
- Broadband UVB (BB-UVB, 290-320nm)
- Narrowband UVB (NB-UVB, wavelength 311-313nm)
- Photochemotherapy: PUVA (Psoralen with UVA, wavelength 320-400nm)
- Excimer laser: for localised psoriasis, not yet available in New Zealand (308nm)
Most phototherapy units depend on fluorescent lamps. These are low-pressure mercury discharge lamps with a phosphor coating inside the tube. Electrons from the power source excite the mercury atoms to produce UVC, which is then re-emitted by the phosphors as longer wavelengths. Differing phosphors and filters result in lamps with differing and continuous spectral outputs, i.e. primarily UVB, UVA or visible light (as used for office lighting).
Phototherapy requirements
Broadband UVB has been used for treating psoriasis for many years but has now largely been replaced by narrowband UVB, which is more effective at treating skin disease and less likely to result in phototoxic erythema (burning).
Psoralen, either applied topically or taken as oral capsules, interacts with UVA to produce a therapeutic effect on inflammatory skin diseases – UVA on its own does little. Unfortunately, although PUVA is more effective than UVB therapy, it is more likely to cause skin cancer, especially squamous cell carcinoma. It is now usually limited to a maximum of 100-200 treatments depending on skin type (three to six courses of 30 treatments).
Indications for phototherapy
In general, the same skin diseases may be treated with phototherapy using UVB or photochemotherapy (PUVA). The most common conditions treated include:
- Psoriasis (80% patients)
- Atopic dermatitis
- Other forms of dermatitis
- Pruritus
- Vitiligo
Many other skin diseases may also respond to treatment.
Phototherapy has risks and side effects and may be inconvenient and expensive, so it is limited to those with extensive or severe disease on exposed and relatively hairless skin.
Contraindications for phototherapy
Relative contraindications include:
- Childhood
- Pregnancy and breastfeeding (PUVA)
- Immobility or inability to stand unassisted for 10 minutes or longer
- Very fair skin (skin type 1 and 2, especially PUVA)
- Past excessive exposure to natural sun light or phototherapy
- Immunosuppressive medication
- Photosensitising creams or medications
- Past skin cancer, especially melanoma
Other possible topical or systemic treatments may be selected instead of or as well as phototherapy. Careful eye protection is mandatory for all patients.
UVB phototherapy
UVB phototherapy is available at the larger public hospitals and some private dermatologists’ offices in New Zealand. Children with extensive skin diseases may be treated with UVB under careful and experienced medical and nursing supervision.
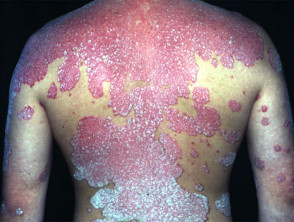
Psoriasis is the most common skin disease treated with UVB. NB-UVB phototherapy clears about 75% of patients, where clearance is defined as 90% or greater reduction in extent of psoriasis compared to baseline. The number of treatments required ranges from 10 to 40, delivered two to five times weekly (most often three times weekly). The initial dose and incremental increases in dose each week depend on skin type and response to treatment. For most patients the whole body is treated except the face and genitals.
Effect of UVB
UVB is most likely to be successful with acute guttate and thin plaque psoriasis, especially if there is a history of improvement on exposure to sunlight. It is less likely to be successful with very thick plaques, especially if there is dense surface scale. Many patients are treated with additional topical or systemic therapy.
An increasing range of skin diseases is reported to clear or improve with NB-UVB but these respond less predictably and may require a greater number of treatments.
The mechanism of action of UVB on various skin diseases but is probably related to the suppression of major components of cell-mediated immune function.
Sub-erythemal UVB may be effective in clearing the skin disease but it is difficult to select the perfect dose. Localised or generalised erythema is a common complication of treatment. It begins 2 to 6 hours after exposure, peaks at 12-18 hours after exposure and generally persists for 48 hours.
Complications of UVB phototherapy
Acute complications include:
- Acute sunburn effect: tender erythema &/or pruritus
- Photokeratitis: ocular grittiness, pain, photophobia, tearing and blepharospasm
- Photosensitivity
- Worsening skin disease
Long-term complications are not seen in children. They may include:
- Photo-ageing: wrinkling, freckling, xerosis, telangiectasia, elastosis and atrophy
- Skin cancer: actinic keratoses, squamous cell carcinoma, basal cell carcinoma and melanoma.
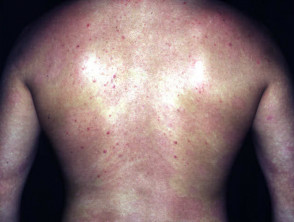
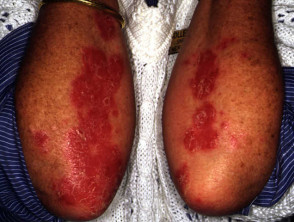
Photoxic erythema and blistering following excessive NB-UVB
PUVA
PUVA is used for more severe long-lasting and resistant disease and is delivered two to four times weekly. It is not often used nowadays, and very rarely in children.
Psoralens are a group of natural furocoumarins, commercially derived from Ammi Majus, a plant found in Egypt. They are present in celery, carrots, parsley, parsnip and other vegetables. Most patients are treated with 8-methoxypsoralen (methoxsalen) orally 2 hours prior to exposure to UVA. If UVA is unavailable, UVB may be used instead. Paints, creams or soaks are sometimes used for localised disease such as dermatoses affecting the hand and foot.
Effect of PUVA
Psoralen interacts with UVA in the epidermis to form DNA photo-adducts. The resulting photoproduct: Slows down keratinocyte proliferation Suppresses the cutaneous immune reaction Affects melanocytes, fibroblasts and endothelial cells
PUVA results in inflammation (phototoxicity) and melanogenesis (tanning) in normal skin. Phototoxic inflammation reaches a peak 48-96 hours after exposure and lasts days to weeks.
As photosensitivity persists for some hours after taking methoxsalen, patients should wear covering clothing, apply broad-spectrum sunscreen and wear wrap-around UVA-blocking sunglasses at least until nightfall of the treatment day.
Complications of PUVA
Acute complications are similar to those described for UVB with the addition of medication-related anorexia, nausea, headache and dizziness. Phototoxicity can result in tender erythema &/or deep pruritus for several weeks or longer
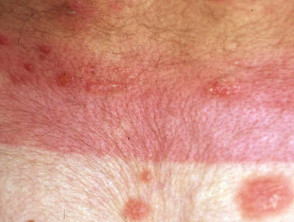
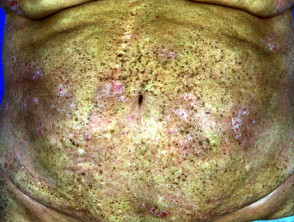
Extensive freckling and dryness due to PUVA in patient with severe psoriasis
Long-term complications of PUVA are more marked than from UVB and include:
- Photo-ageing: wrinkling, freckling, xerosis, telangiectasia, elastosis, white macules, skin atrophy, cataracts
- Skin cancer: actinic keratoses, squamous cell carcinoma (SCC) (x10) >> basal cell carcinoma (BCC) and melanoma. Genital skin cancer risk is alarming (x286): always shield genitalia.
Activity
Discuss possible psychosocial issues related to UVB phototherapy in children.
Related information
On DermNet NZ:
Information for patients
Phototherapy course for health professionals
Other websites:
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.