DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Cutaneous signs of systemic disease Miscellaneous genetic diseases CME
Cutaneous signs of systemic disease
Miscellaneous genetic diseases
Created 2009.
Learning objectives
- Recognise cutaneous signs of neurofibromatosis, tuberous sclerosis and pseudoxanthoma elasticum
Introduction
The three conditions described on this page are the most common genetic syndromes that may present initially to a dermatologist. A number of mutations in specific genes have been described for them, resulting in quite variable clinical presentations. Spontaneous mutations are probably responsible for about 50% of cases.
Neurofibromatosis
Neurofibromatosis is a neurocutaneous condition but can involve many organs. There is autosomal dominant inheritance due to many different mutations in the neurofibromatosis gene. Neurofibromatosis 1, NF-1 or peripheral neurofibramtosis, is the most common type affecting the skin but the mosaic form, segmental NF, is occasionally seen.
Cutaneous signs of NF-1 include:
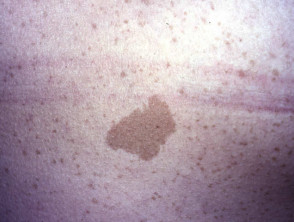
- Six or more café au lait macules, which appear in early childhood. Well circumscribed pale brown macules.
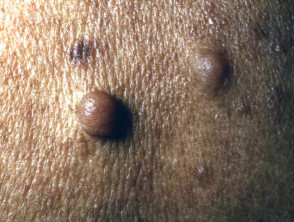
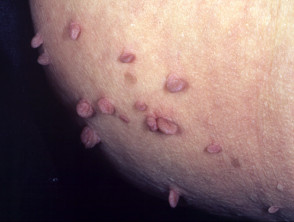
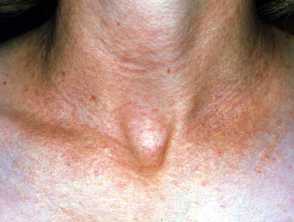
- Neurofibromas, which arise in adolescence and adult life. Pink, brown or skin coloured cutaneous or subcutaneous firm or soft nodules. The diagnosis is confirmed by ‘buttonhole invagination’ when pressing with a finger. The plexiform neurofibroma is a larger irregular plaque.
- Skin tags
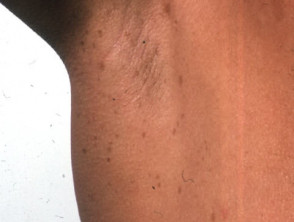
- Axillary and perineal freckling
Other signs may include:
- Lisch nodules: dome shaped superficial lesions around the iris
- Bone defects
- Tumours of acoustic nerve or optic nerve
- Intracranial tumours
- Schwannomas: more common in NF-2, which affects cranial and spinal nerves
- Learning difficulties or mental retardation
- Endocrine problems
- Malignant tumours: these arise in about 10% of patients.
Annual examination of the skin, eyes and hearing should be carried in childhood. Neurofibromas that increase in size or become painful should be excised as these may be signs of malignant change.
Neurofibromatosis
Tuberous sclerosis
Tuberous sclerosis, also known as epiloia, is an autosomal dominant genetic neurodermatosis affecting cellular differentiation and proliferation resulting in hamartoma formation in many organs.
It presents with epilepsy, mental retardation and cutaneous signs. These include:
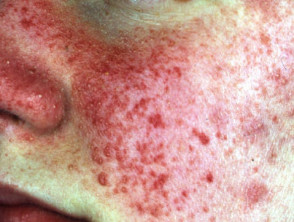
- Angiofibromas (firm pink papules on nose, cheeks and oral mucosa)
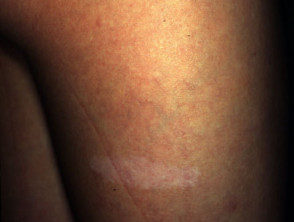
- Ash-leaf hypopigmented macules on trunk and limbs (present at birth)
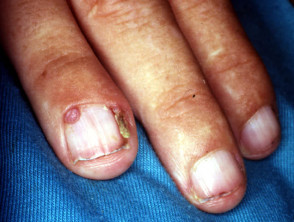
- Periungual fibromas (smooth nodules around nails)
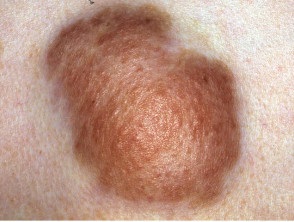
- Connective tissue hamartomas (skin-coloured firm plaque on trunk called Shagreen patch)
The facial angiofibromas may be quite disfiguring. They may be successfully treated by a vascular or ablative laser.
Tuberous sclerosis
Pseudoxanthoma elasticum
Pseudoxanthoma elasticum (PXE) is a group of inherited disorders in which elastic tissue in skin, blood vessels and eyes is defective. The result is groups of yellowish bumps on the neck, axillae and elsewhere associated with gastrointestinal haemorrhage, hypertension, peripheral vascular disease and ocular “angioid” streaks and retinal haemorrhages. PXE is generally diagnosed in young adults.
Pseudoxanthoma elasticum (PXE)
Activity
Describe the genetic defects resulting in neurofibromatosis, tuberous sclerosis and PXE.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Pediatric diseases
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.