Introduction
Adverse cutaneous reactions to psychotropic medications present a significant problem to clinical practice for several reasons:
- Psychotropic medications, taken as a class, are some of the most widely prescribed medications.
- Adverse cutaneous reactions are common, and occur in 2–5% of patients taking psychotropic drugs.
- While some adverse cutaneous reactions are mild and easily treatable, others are life-threatening.
- These reactions can complicate the treatment of psychiatric conditions, particularly in the presence of comorbidities.
Examples of adverse cutaneous reactions to psychotropic drugs
Erythema multiforme
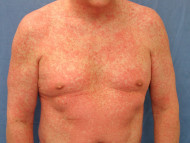
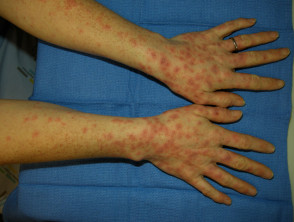
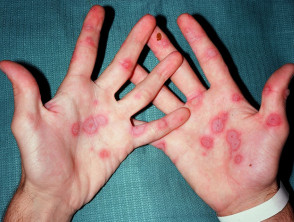
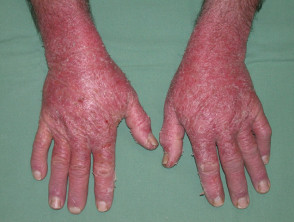
Erythema multiforme, a hypersensitivity reaction, most often presents as an acute eruption of papules, plaques and blisters on the limbs, soles of the feet and palms of the hands. It is accompanied by an elevated temperature and a general feeling of malaise. Mucosal involvement occurs in erythema multiforme major.
Although usually due to viral infection, erythema multiforme is occasionally caused by a drug, and then it usually occurs within a few days of starting the causative drug. Psychotropic drugs that can cause erythema multiforme include bupropion, clozapine and fluoxetine.
Erythema multiforme
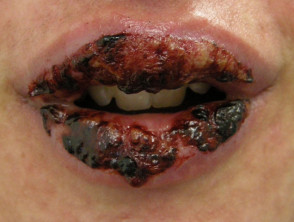
Stevens–Johnson syndrome/toxic epidermal necrolysis
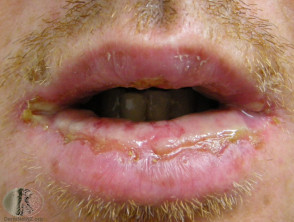
Stevens–Johnson syndrome/toxic epidermal necrolysis (SJS/TEN) is a severe, life-threatening illness with blistering of the mouth and other mucous membranes and widespread macular rash, with detachment of the epidermis from the dermis.
Psychotropic medications like alprazolam, duloxetine, sertraline and anticonvulsant medications can cause SJS/TEN.
Stevens-Johnson syndrome/toxic epidermal necrolysis
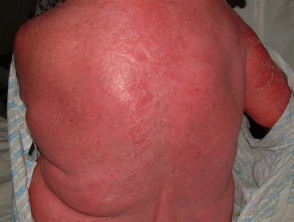
Erythroderma/exfoliative dermatitis
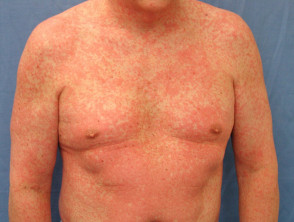
The use of the term erythroderma implies a skin disease affects ≥85% of the body surface. Exfoliative dermatitis describes widespread peeling. Drug-induced erythroderma/exfoliative dermatitis presents with pruritus, discomfort or tightness, redness, and peeling or scaling of the skin. It can lead to cardiac failure due to dilated blood vessels.
Psychotropic drugs that can cause erythroderma include aripiprazole, lamotrigine and lithium.
Erythroderma
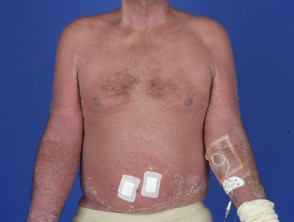
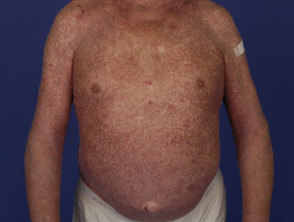
Drug hypersensitivity syndrome
Drug hypersensitivity syndrome is a potentially life-threatening severe adverse reaction to drugs with fever, generalised rash or erythroderma, and systemic involvement.
Psychotropic drugs associated with drug hypersensitivity syndrome include amitriptyline, and anticonvulsants such as carbamazepine and valproic acid.
Drug hypersensitivity syndrome
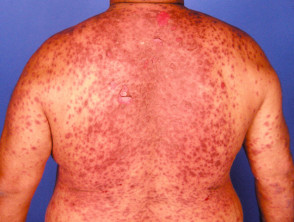
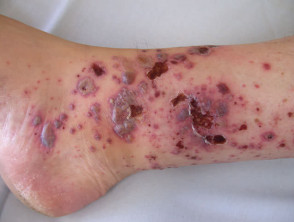
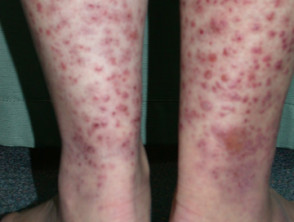
Cutaneous vasculitis
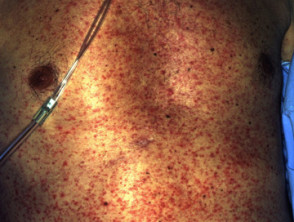
Cutaneous vasculitis is a group of disorders characterised by inflamed blood vessels in the skin. It presents with palpable purpura or urticarial eruptions, and in some cases, evidence of systemic vasculitis.
Psychotropic medications that can cause vasculitis include oxcarbazepine, methylphenidate and clomipramine.
Cutaneous vasculitis
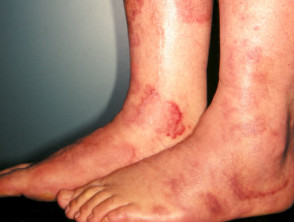
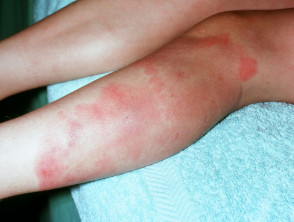
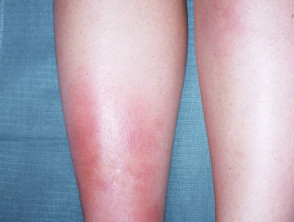
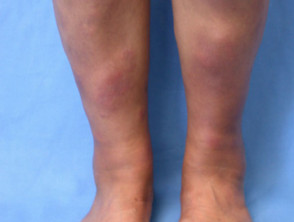
Erythema nodosum
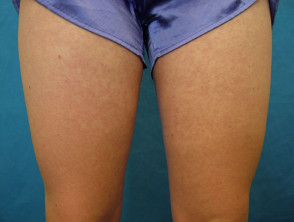
Erythema nodosum is an inflammatory disorder presenting with painful, red, indurated plaques, usually on the lower extremities. These plaques result from the inflammation of fat cells under the skin.
Drugs that may cause erythema nodosum include fluoxetine, paroxetine and venlafaxine.
Erythema nodosum
Other cutaneous adverse drug reactions
Other cutaneous adverse drug reactions to psychotropic medications include:
- Exanthematous, morbilliform, seborrhoeic, lichenoid and psoriasiform eruptions
- Phototoxic reactions
- Diffuse drug-induced alopecia
- Drug-induced urticaria
- Drug-induced hyperhidrosis.
Other cutaneous adverse drug reactions
Reducing the risk of a cutaneous drug reaction
Risk factors for cutaneous drug reactions include:
- African ancestry
- Being female
- Age over 70 years
- A personal and family history of cutaneous adverse reactions.
The risk of cutaneous adverse reaction to a psychotropic drug is reduced by:
- Careful assessment of the individual prior to prescribing a new medication, including their medical history, past history of drug reactions, and family history of drug reactions
- Sun protection when taking photosensitising medications; a protective hat and clothing should be worn as well as sunscreen.