What is alopecia mucinosa?
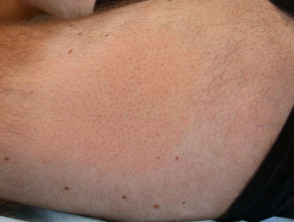
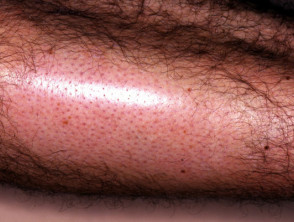
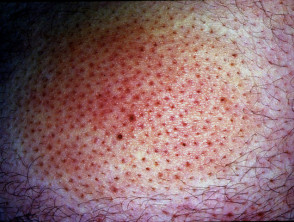
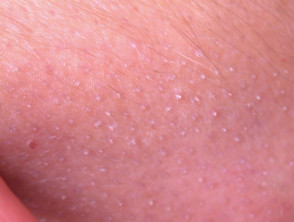
Alopecia mucinosa, also known as follicular mucinosis, describes the appearance of mucin around hair follicles as seen under the microscope. It is characterised by bald patches of skin in which hair follicles are prominent.
Mucins look like stringy clear or whitish goo mainly composed of hyaluronic acid, a normal component of the ground substance surrounding collagen in the dermis. Several other forms of mucinosis are described and classified.
- A primary and acute disorder occurring in children and adolescents (Pinkus type).
- A primary and chronic disorder occurring in people older than 40 years.
- A secondary disorder associated with benign or malignant skin disease.
- Urticaria-like follicular mucinosis (rare).
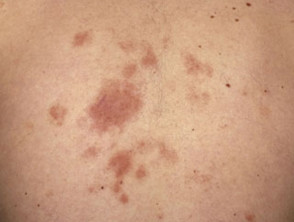
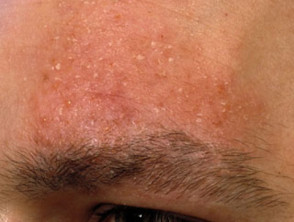
Alopecia mucinosa
What causes alopecia mucinosa?
The cause of alopecia mucinosa is unknown, but it may have something to do with circulating immune complexes and cell-mediated immunity. What is known is that mucinous material deposits and accumulates in hair follicles and sebaceous glands to create an inflammatory condition that subsequently breaks down the ability of the affected follicles to produce hair.
What are the clinical features?
Alopecia mucinosa most commonly affects face, neck and scalp, but any part of the body may be affected.
- It presents as grouped follicular papules within reddened, dry, patches or plaques.
- Patches or plaques are usually 2–5 cm in diameter but can be larger.
- One or more lesions may be present from onset or a single lesion may develop to multiple lesions over a few weeks or months.
- Hair loss is non–scarring and potentially reversible in the early stages, but in more advanced disease the hair follicles are destroyed, causing scarring alopecia.
Primary and acute alopecia mucinosa
- Affects people < 40 years.
- Usually, only one or a few lesions arise.
- They are often located on the head, neck and upper arm.
- Most resolve spontaneously within 2 months to 2 years.
Primary and chronic alopecia mucinosa
- Affects people > 40 years.
- Widespread and often numerous lesions may persist or recur indefinitely.
- It presents as flat or raised patches that may rarely ulcerate.
- Permanently bald patches are studded with horny plugs.
- Sometimes mucin can be squeezed out of affected follicles.
Urticaria–like follicular mucinosis
- Presents as itchy small bumps (papules) or raised areas (plaques).
- These are mostly found on the head and neck.
Secondary alopecia mucinosa
- Affects people > 40 years.
- Follicular mucinous degeneration may arise in inflammatory skin diseases such as lupus erythematosus and lichen simplex.
- It may also arise in malignant diseases such as cutaneous T-cell lymphoma (the most common association, affecting 10–30% of cases of alopecia mucinosa), Kaposi sarcoma and Hodgkin lymphoma (especially in children).
- Skin features typical of the underlying disease may also be present.
- A skin biopsy is necessary to distinguish these from primary alopecia mucinosa.
How is alopecia mucinosa diagnosed?
Alopecia mucinosa is diagnosed by its clinical appearance and supported by histopathological findings on biopsy:
- Accumulation of mucin in the pilosebaceous follicle and sebaceous glands
- Keratinous debris within a cystic cavity
- Inflammation
- Degeneration of follicular structures.
Histological features of the underlying disease are present in secondary alopecia mucinosa.
What is the differential diagnosis of alopecia mucinosa?
Secondary causes of alopecia mucinosa such as mycosis fungoides may not be diagnosed for some years, necessitating careful follow-up and biopsy. Other conditions that may need to be considered in the differential diagnosis include:
- Alopecia areata, which causes non-scarring localised bald patches
- Seborrhoeic dermatitis, psoriasis and tinea capitis, which may cause scaly plaques and hair loss
- Discoid lupus erythematosus and lichen planopilaris, which may cause localised areas of scaling and scarring alopecia.
What is the treatment for alopecia mucinosa?
There is no proven effective treatment for alopecia mucinosa. Usually, primary and acute alopecia mucinosa occurring in children resolves spontaneously. Because there is a small chance of spontaneous resolution for other forms of the disease, the effect of treatment can be difficult to assess. Some treatments that have been tried with limited success include:
- Topical, intralesional and systemic corticosteroids
- Oral antibiotics such as minocycline
- Dapsone
- Indomethacin
- Interferons
- Topical and systemic photochemotherapy (PUVA)
- Topical nitrogen mustard
- Radiation therapy
- UVA1 phototherapy
- Topical bexarotene 1% gel.
Secondary alopecia mucinosa should be treated appropriately for the underlying skin disease, particularly if it is cutaneous T-cell lymphoma.