What is bullous systemic lupus erythematosus?
Bullous systemic lupus erythematosus (SLE) is an autoimmune subepidermal blistering disease that occurs in patients with SLE. It can be associated with antibodies against type VII collagen.
Bullous SLE is also called bullous eruption of SLE and vesiculobullous SLE.
Bullous systemic lupus erythematosus
Who gets bullous systemic lupus erythematosus?
The incidence of bullous SLE was estimated to be 0.22 and 0.26 cases per million per year in France and Singapore. In a large cohort of sera taken from patients with immunobullous disorders, 1–2% were identified as bullous SLE [1,2].
Like SLE, bullous SLE has been reported most commonly in women of African descent in their thirties. However, bullous SLE occurs in all ages, sexes, and ethnicities.
Bullous SLE may be the presenting sign of SLE in approximately one third of patients. In the majority though, SLE has already been diagnosed, in some cases many years prior.
What causes bullous systemic lupus erythematosus?
Bullous SLE is classified into three types based on immunohistochemistry.
- Type I bullous SLE is the most common type and is defined by auto-antibodies targeted against type VII collagen, specifically the non-collagenous type 1 and type 2 (NC1 and NC2) domains. The NC1 domain plays an important role in maintaining the structure of the dermal-epidermal junction (DEJ) [3–5].
- In type II bullous SLE, antibodies are targeted against other antigens of the DEJ including BP130, BP280, and laminin 5 or 6.
- Type III bullous SLE is characterised by staining in the epidermis with or without staining in the dermis.
The three types cannot be distinguished clinically.
Predisposing factors include adverse drug reactions to hydralazine, penicillamine, methimazole; and exposure to ultraviolet (UV) B radiation.
Bullous SLE type I is similar to epidermolysis bullous acquista (EBA) in that both have autoantibodies to type VII collagen on indirect immunofluoresence [6]. However bullous SLE and EBA differ clinically and the IgG autoantibodies have now been shown to be different.
What are the clinical features of bullous systemic lupus erythematosus?
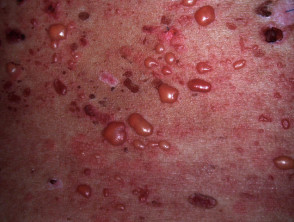
In bullous SLE, tense vesicles, bullae and erosions arise on normal or erythematous skin, usually in sun-exposed sites.
- The face is often affected; mucosal surfaces can also be involved.
- The onset of bullous eruption does not correlate with the activity of the systemic disease.
- The bullae may have clear or haemorrhagic content.
- The blisters heal without scarring.
- Pruritus is absent or mild.
- Milia are not a prominent feature.
- Erythematous annular urticarial plaques may arise.
What are the complications of bullous systemic lupus erythematosus?
The complications of bullous SLE are those of the underlying SLE. The development of bullous SLE is often associated with a flare of lupus nephritis.
How is bullous systemic lupus erythematosus diagnosed?
Investigations are necessary to distinguish bullous SLE from SLE with a concomitant blistering disorder.
Histopathological findings resemble dermatitis herpetiformis, in that they both show:
- Subepidermal splitting
- A neutrophil predominant infiltrate in the upper dermis
- Papillary micro-abscesses
- Leucocytoclasis
- Mucin deposition in the dermis.
Basal layer vacuolation, characteristic for other forms of cutaneous LE, is not present.
The characteristic direct immunofluorescence (DIF) finding in a perilesional skin biopsy of bullous SLE is linear or granular immunoglobulin (Ig)G, IgM, IgA or C3 at the dermoepidermal junction (DEJ). Type I bullous SLE is typically associated with the linear pattern.
Serum autoantibodies detected by the indirect immunofluorescence test or enzyme-linked immunosorbent assay (ELISA) are against type VII collagen in type I bullous SLE. BP 230, BP 180, or laminin 5 or 6 are detected in type II bullous SLE.
Serration pattern analysis of DIF microscopy differentiates tissue bound auto-antibodies against type VII collagen, where a u-serrated pattern is seen, from all other anti-DEJ antibodies where an n-serrated pattern is seen [7].
Diagnostic criteria for bullous SLE requires:
- A diagnosis of SLE based on the American College of Rheumatology criteria
- An acquired vesiculobullous eruption
- Histopathology evidence of a subepidermal blister and neutrophil-predominant dermal infiltrate resembling dermatitis herpetiformis
- DIF microscopy showing linear or granular deposits of immunoglobulin (Ig)G or IgM and often IgA at the basement membrane zone
- Positive or negative indirect immunofluorescence for circulating basement membrane zone autoantibodies.
What is the differential diagnosis for bullous systemic lupus erythematosus?
The differential diagnosis of bullous SLE is SLE with blisters. Other blistering conditions that may arise in SLE include:
- Bullous drug eruption — band-like deposits of IgG, IgM, and IgA may be present, however, linear or granular deposits are not seen
- The pemphigoid group of diseases — bullous pemphigoid, linear IgA disease, epidermolysis bullosa, and dermatitis herpetiformis
- Skin lesions of highly active SLE — these can rarely blister due to extensive vacuolation at the DEJ.
What is the treatment for bullous systemic lupus erythematosus?
Dapsone, at a dose of 1.0–1.5 mg/kg/day, is considered the treatment of choice. It is effective in the vast majority of patients and leads to rapid clinical improvement within days or a few weeks. This rapid response differentiates bullous SLE from SLE with a concomitant autoimmune blistering disease.
Where dapsone fails, prednisolone (systemic steroids) and azathioprine are used. Patients successfully treated with methotrexate or rituximab have been reported [8–11].
What is the outcome for bullous systemic lupus erythematosus?
Bullous SLE is transient in the majority of cases and usually completely regresses with no further flares, irrespective of the activity of the systemic disease. It typically resolves without milia or scarring but can leave hypo- or hyper-pigmentation.