Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Causes
Demographics
Clinical features
Diagnosis
Treatment
Outcome
Cold urticaria is a relatively uncommon form of chronic inducible urticaria. Urticarial weals develop after being exposed to cold, cold water, and cold objects.
Acquired cold urticaria is now understood to be a completely different disorder from familial cold autoinflammatory syndrome (FCAS), previously known as hereditary cold urticaria. FCAS is one of the cryopyrin-associated periodic syndromes (CAPS).
Cold urticaria is caused by exposure to cold. Why the cold stimulus causes the activation of mast cells and the subsequent release of histamine, and other inflammatory mediators remain unknown.
Cold urticaria may be primary (idiopathic) or secondary to an underlying haematologic (blood condition) or infectious disease. Most cases are of the idiopathic (unknown cause) type.
Acquired cold urticaria is rare, affecting about 0.05% of the population. It is most often diagnosed in young and middle-aged adults, but it may present in children or the elderly. It is twice as common in women as in men.
It is commonly associated with the physical urticarias dermographism and cholinergic urticaria, and sometimes with ordinary urticaria. Underlying conditions that have been associated with secondary cold urticaria include:
Symptoms of cold urticaria become evident within 2–5 minutes after exposure and last for 1–2 hours. They include:
Swimming in cold water is the most common cause of a severe cold urticarial reaction. Severe reactions may also arise in patients exposed to cold rooms or during surgery under general anaesthesia.
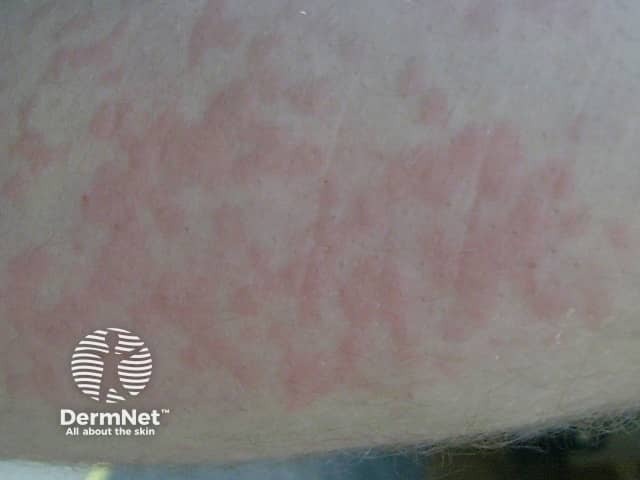
Cold urticaria
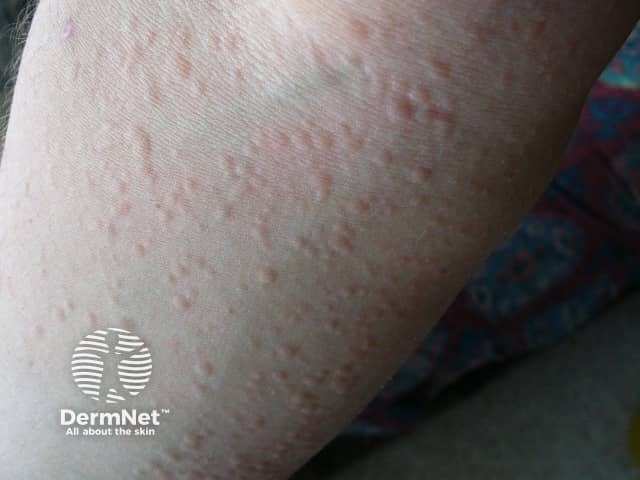
Cold urticaria
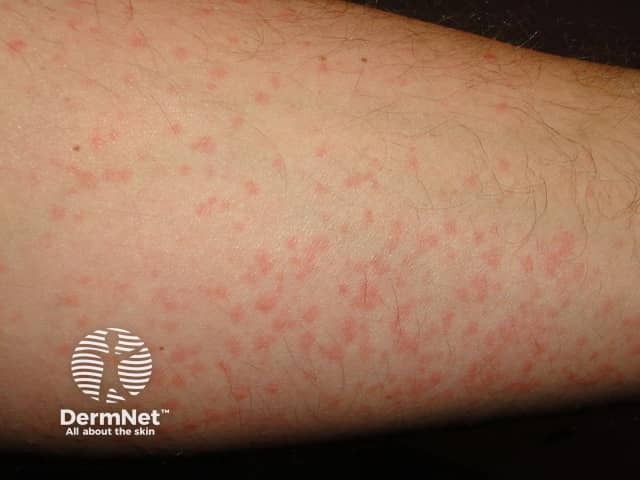
Cold urticaria
Cold urticaria can be diagnosed by applying an ice cube against the skin of the forearm for 1–5 minutes. A distinct red swollen rash should develop within minutes in the area exposed to the cold-stimulation test if a patient has cold urticaria. Complete blood counts and metabolic tests may also be performed to determine associated diseases.
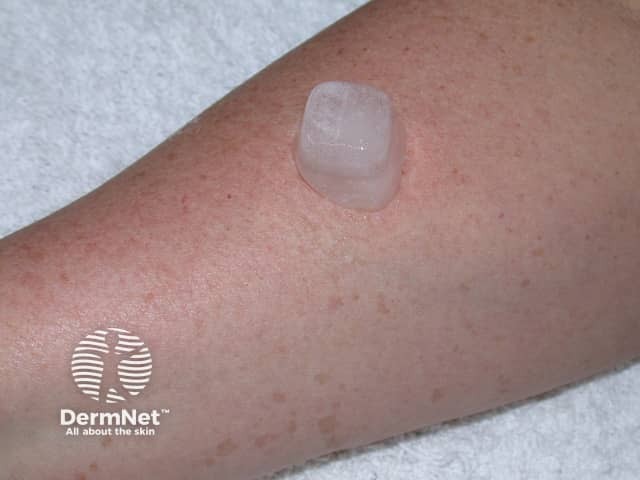
Ice applied to normal skin
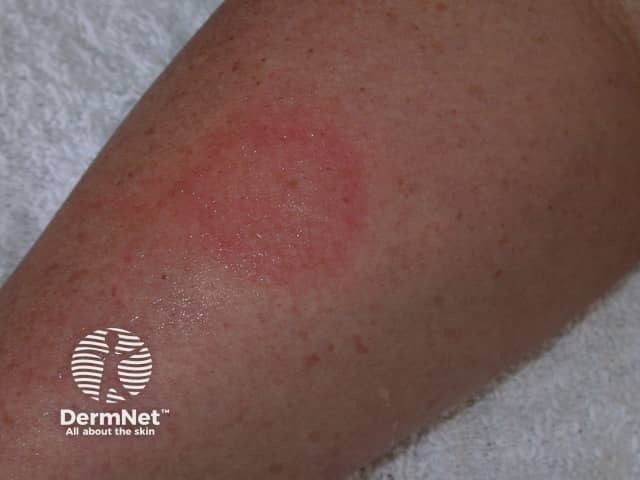
Red patch on removal of ice
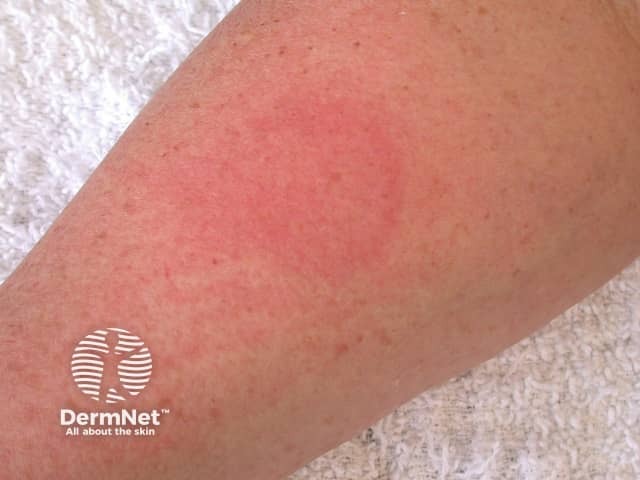
Enlarging weal 5 minutes later
Patients with cold urticaria should learn to protect themselves from a rapid drop in body temperature. Aquatic activities (such as swimming and surfing) should always be under supervision.
Patients who develop anaphylactic reactions should carry emergency adrenaline.
Regular doses of conventional antihistamines have generally proven to be ineffective, initially standard doses but if need be high doses of non-sedating antihistamines may be helpful (for example cetirizine up to 40 mg daily). Some related medications that have been found to be useful include cyproheptadine, doxepin and ketotifen.
Omalizumab in addition to antihistamines may be helpful in recalcitrant disease, initially 150 mg every 4 weeks, but the dose can be doubled if there is inadequate response.
There have been reports of successful treatment with leukotriene antagonists, ciclosporin, systemic corticosteroids, dapsone, oral antibiotics and the synthetic hormone, danazol.
Cautious induction of cold tolerance may be successful (desensitisation), by gradually hardening the skin to cold conditions and then exposing the skin to it regularly, for example, by taking regular cold showers.
The anaesthetist should be told in advance that the patient has cold urticaria. Staff must take precautions to keep the patient warm.
Cold urticaria usually lasts for some years. About 30% report resolution of symptoms within 5 to 10 years. A 20-year follow-up study of 41 patients diagnosed with cold urticaria showed it had resolved by 10 years in about a quarter of patients. Most affected individuals relied on lifestyle modifications to avoid flares.