What is gold contact allergy?
Contact allergy to gold is a delayed type hypersensitivity reaction following exposure to gold or its alloys, typically manifesting as an allergic contact dermatitis.
Gold was named Contact Allergen of the Year in 2001 by the American Contact Dermatitis Society.
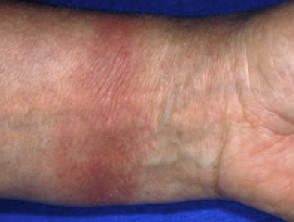
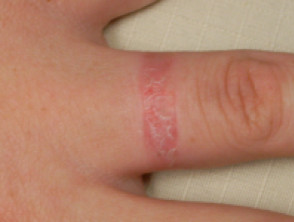
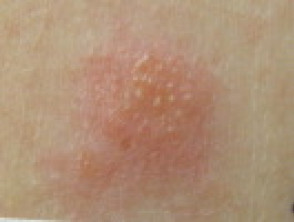
Gold jewellery reaction
Who gets gold contact allergy?
Individuals with gold contact allergy have usually been exposed to gold in jewellery, dental restorations, or occupationally.
Gold allergy is diagnosed most frequently in women (90%). This is probably due to women typically wearing more gold jewellery and having more piercings than men.
Those with gold allergy are often also allergic to nickel and cobalt. Gold has been found in some patch test series to be the second most common metal allergen after nickel, although the clinical relevance of this must be questioned.
What causes gold contact allergy?
Gold allergy is a type IV hypersensitivity reaction which often develops following skin piercing and the immediate wearing of gold studs allowing the dermis to come into direct contact with gold.
Titanium dioxide found in various sunscreens and cosmetics can potentiate the release of gold from jewellery. Copper in low-carat gold jewellery can also cause gold release, resulting in gold allergy despite the limited gold content.
What are the clinical features of gold contact allergy?
The most common clinical presentation of gold contact allergy is a localised dermatitis or chronic papular reaction at or near the site of exposure such as the earlobes due to gold earrings, or on fingers or neck where gold jewellery is worn.
The face and eyelids are also commonly affected sites suggesting transfer of the allergen following the handling of gold or airborne exposure.
Gold allergy associated with dental restorations can present with oral symptoms, including cheilitis, mucosal erosions, contact stomatitis, or an oral lichenoid reaction.
A gold allergy reaction can be widespread such as a generalised dermatitis.
What are the complications of gold contact allergy?
Gold contact allergy can proceed to a persistent nodular reaction, particularly in piercings. Histology may show a pseudolymphomatous or sarcoidal inflammatory reaction.
Cutaneous contact allergy to gold can result in localised or generalised reactions with subsequent exposure to gold-containing implants or medications.
How is gold contact allergy diagnosed?
Gold contact allergy is diagnosed through a detailed history, survey of rash distribution, and confirmation on patch testing. Gold contact allergy should be considered in cases of eyelid or face dermatitis, or where the skin changes relate to gold jewellery contact.
Gold patch testing
Gold sodium thiosulfate (GST) of various concentrations in petrolatum is the most commonly used gold allergen in patch testing. Gold patch test allergens are a known irritant to atopic skin. The allergic patch test reaction can be delayed, appearing up to 3 weeks after patch removal and can be persistent, lasting months.
The clinical relevance of a positive patch test reaction to GST must then be assessed. The relevance of a positive gold patch test is low compared to many other allergens, and may explain the clinical presentation in only 10–15% of cases.
Persistent nodular reactions may require a skin biopsy of the affected site to exclude other diagnoses.
What is the differential diagnosis for gold contact allergy?
Differential diagnoses to gold contact allergy may include:
- Contact allergic dermatitis due to other allergens (such as nickel) in the jewellery
- Atopic dermatitis
- Irritant contact dermatitis due to soap and water under gold rings.
What is the treatment for gold contact allergy?
Treatment of gold contact allergy is as for all allergic contact reactions — avoidance of the allergen, and treatment of the inflammatory reaction. Despite avoidance, gold contact reactions can be quite persistent. Some individuals will be able to slowly reintroduce wearing gold jewellery for limited time periods whereas others will have to avoid gold indefinitely depending on the severity of the reaction.
Chronic dermatitis may need treatment with emollients and topical corticosteroids.
Surgical excision may be required for persistent nodules.
What is the outcome for gold contact allergy?
Further contact with gold can be avoided and gold dental restorations can be removed if necessary. Occupational exposure to gold should be minimised by wearing appropriate personal protective equipment.
Patients with known gold allergy and rheumatoid arthritis should undergo patch testing with gold sodium thiosulphate prior to starting treatment with gold-containing medication due to the risk of systemic allergic contact dermatitis.