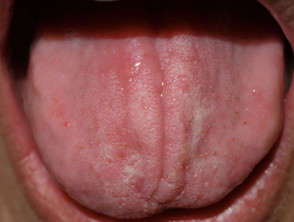
What is stomatitis?
Stomatitis means a sore mouth.
What is contact stomatitis?
Contact stomatitis is an uncommon allergic reaction affecting the inside of the mouth caused by contact with an allergen, usually flavourings, metals or other components in oral hygiene products, foods, dental restorations and medications. It may also be called allergic contact stomatitis to distinguish this form from intraoral irritant reactions.
Stomatitis to contact with rubber glove during a dental procedure
Who gets contact stomatitis and why?
Contact stomatitis is a delayed hypersensitivity (Type IV) reaction to a chemical in contact with the lining of the mouth. It occurs in people already sensitised to the allergen. However, it is quite uncommon compared to contact allergic dermatitis or contact cheilitis, probably because:
- Saliva constantly flushes the mouth so chemicals are diluted and do not stay in contact with the mucosa for very long
- There is a good blood supply to the lining of the mouth meaning any chemical absorbed through the mucosa is quickly removed from the area
- The lining of the mouth is not well keratinised so chemicals are less likely to bind to keratin protein to form an allergen.
Rarely, contact urticaria may present as stomatitis.
Which products cause contact stomatitis?
Oral hygiene products
- Toothpaste
- Dental floss
- Mouthwash
Foods
- Chewing gum
- Sweets/candies/lollies
- Foods especially flavoured with cinnamon
Dental restorations
- Orthodontic wires – brackets, bands
- Dental prostheses – dentures, plates
- Dental cement
- Dental restorations
- Dental amalgam
- Composite resin
- Gold
Medications — topical
Major sources of allergens causing contact stomatitis
There are many chemicals that have been identified as responsible for contact stomatitis.
- Flavourings and preservatives (food additives): cinnamon (cinnamaldehyde, cinnamon essential oil), carvone, spearmint essential oil, menthol essential oil, dodecyl gallate — see fragrance allergy
- Metals: nickel, palladium, gold, mercury, zinc
- Dental prostheses: formaldehyde, acrylate monomer, colophony
- Rubber /Latex: gloves, rubber dams, etc.
What are the clinical features of contact stomatitis?
The symptoms and signs of acute contact stomatitis usually develop within hours of contact with the allergen. The chronic form occurs when the allergen is always in the mouth such as with a dental restoration.
The pattern will depend on what form the allergen is in. For example, if the allergen is in a removable dental prosthesis, the pattern will reflect the shape and area of contact between the prosthesis and the oral mucosa. The reaction may be generalised when due to toothpaste or mouthwash. Stomatitis due to dental restoration or orthodontic devices will be adjacent to the restored tooth or wires.
All parts of the mouth can be affected. However, the most common sites involved in contact stomatitis are:
- Sides of the tongue
- Gums
- Inside of the cheeks
- Hard palate.
Contact stomatitis has a number of possible clinical features that may occur in various combinations. These include:
- Burning
- Swelling – may mimic contact urticaria or angioedema
- Redness
- Cracking
- Ulcers, erosions – erosive stomatitis
- Small blisters
- Peeling
- White patches or lines
- Pain.
A lichenoid amalgam reaction is also a form of contact stomatitis and is a type of oral lichen planus.
Plasma cell gingivitis is another specific form of contact stomatitis.
Contact urticaria and oral allergy syndrome are type 1 hypersensitivity reactions and occur and recover more quickly than contact stomatitis.
How is contact stomatitis diagnosed?
The diagnosis of contact stomatitis is mainly clinical, based on history and examination. Investigations may be done to exclude other possible diagnoses and to try to identify the responsible allergen.
A mucosal biopsy may be required to exclude other conditions such as various forms of oral leukoplakia, trauma, oral candidiasis (thrush), oral lichen planus and oral lichenoid drug eruption, lupus erythematosus or discoid lupus, or oral cancer. The histology of contact stomatitis itself is nonspecific. However, the presence of many plasma cells may be suggestive of a contact allergy.
The likely source of the allergen will often be identified on the history and examination with improvement when the source is avoided. Recurrence of the stomatitis following rechallenge with the allergen confirms the cause. Patch testing, including with the patient’s own products, may be helpful in identifying the responsible allergen but false negatives are common. The relevance of a positive patch test reaction must be assessed in the clinical setting.
How is contact stomatitis treated?
The most important treatment for contact stomatitis is the avoidance of the allergen. If it is due to a flavouring or preservative in food or dental hygiene products, the patient should be advised to stop using the product. It may take up to 2 weeks for complete resolution. A topical steroid application may be required for persistent, severe or chronic reactions.
In one case due to an acrylic monomer in a new denture, prolonged boiling of the denture resulted in full curing of the acrylate and the stomatitis resolved.
When the contact stomatitis is due to a dental restoration (particularly gold) or orthodontic device (nickel), replacement of the restoration or device may be considered if the stomatitis reaction is clearly related by site to the restoration/device and a positive patch test to the metal (nickel sulphate hexahydrate or gold sodium thiosulphate) has been shown.