Submit your photo of COVID-19-related skin conditions
Please note that DermNet’s page is a summary about COVID-19 and may quickly become outdated.
Refer to Government websites for up-to-date information about COVID-19.
- World Health Organization (WHO)
- United States of America Centers for Disease Control (CDC)
- United Kingdom Government
- United Kingdom National Health Service
- Australian Government
- New Zealand Government Unite for the recovery
- New Zealand Ministry of Health
*Credit: CDC COVID-19 website
^Credit: New Zealand Government Unite against COVID-19 website (March 2020)
What is COVID-19?
COVID-19 (coronavirus disease 2019) is a contagious viral disease caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
COVID-19 was first reported in December 2019 after a cluster of pneumonia cases in
Wuhan, China. It subsequently spread worldwide, prompting the World Health Organization (WHO) to declare a global pandemic on 11 March 2020.
The SARS-CoV-2 virus is transmitted from person to person through respiratory droplets. Common symptoms of COVID-19 resemble those of the common cold, including fever, cough, runny nose, and muscle aches. Approximately 1 in 3 of those infected are asymptomatic, and the majority of symptomatic patients experience mild to moderate disease. In severe cases of COVID-19, respiratory failure, organ failure, and altered mental status can occur, and the disease can be fatal. Vaccination and general infection prevention measures have been widely employed to curb contagion.
Who gets COVID-19?
COVID-19 affects people of all ages. As of 31 August 2022, over 580,000,000 cases of COVID-19 have been reported worldwide with over 6,400,000 deaths.
Transmission of COVID-19 primarily occurs through exposure to contaminated respiratory droplets from infected persons. Some people may be at higher risk of severe disease such as the elderly, immunocompromised patients, and those with certain comorbidities such as:
Vaccination against COVID-19 has been shown to protect people from contracting the disease and from severe symptoms when infected.
What causes COVID-19?
COVID-19 is caused by SARS-CoV-2, an enveloped, positive-strand RNA virus. SARS-CoV-2 is a member of the Coronavirus family, which contains many other human viruses including those responsible for Middle Eastern Respiratory Syndrome (MERS), Severe Acute Respiratory Syndrome (SARS), and partly the common cold. SARS-CoV-2 is highly genetically similar to a bat-borne coronavirus, leading to suspicion that COVID-19 originated zoonotically.
The infection cycle for COVID-19 begins with the attachment of the virus to the surface of human cells. This is initiated by the binding of viral spike protein to the angiotensin-converting enzyme 2 (ACE2) receptor. The virus subsequently enters the cell and begins replicating using host cell machinery. Eventually, the virus escapes the host cell and infects other cells.
Since the discovery of SARS-CoV-2, multiple variants of concern have been identified:
- Alpha: first reported in the United Kingdom in September 2020
- Beta: first reported in South Africa in May 2020
- Gamma: responsible for a large outbreak in Brazil in November 2020
- Delta: first identified in India in December 2020
- Omicron: first reported in Botswana and South Africa in November 2021.
How is COVID-19 spread?
The SARS-CoV-2 virus is found in droplets spread by an infected individual coughing, sneezing, talking, or touching items. The droplets may land on surfaces such as door handles, computer keyboards, and tabletops. The virus remains infectious for several days on smooth surfaces but for shorter periods on paper, wood, or cloth.
An uninfected individual may touch an invisible droplet then touch their face, transmitting the virus through the mucous membranes of their mouth, nose, and eyes, resulting in infection.
Patients are often infectious for a few days before becoming unwell, when unwell, and for some time after clinical recovery from COVID-19.
Infected people without symptoms are also infectious, although their rate of spreading the infection is about half of those with symptoms; this group is thought to contribute to the spread of the SARS-CoV-2 virus tenfold worldwide. In countries with rapid community spread, restrictions on movement and crowds are required to prevent a logarithmic increase in cases.
What are the clinical features of COVID-19?
The severity of COVID-19 is variable. Approximately 80% of patients have mild symptoms or are asymptomatic. The incubation period is generally within 14 days of exposure; for most, the onset is 4–5 days. Those with shortness of breath can rapidly deteriorate, and therefore should be admitted to hospital for assessment and management.
The most common symptoms of COVID-19 are:
- Fever
- Headache
- Dry cough
- Shortness of breath
- Loss of smell and taste
- Fatigue
- Runny nose.
Less common symptoms include:
- Body aches and pains (myalgias)
- Sore throat
- Abdominal pain
- Diarrhoea
- Paediatric multisystem inflammatory syndrome (PIMS): abdominal pain, vomiting, diarrhoea, rash, and conjunctivitis
- Neurological symptoms such as confusion and coma.
Cutaneous signs of COVID-19
Rashes have been described in all types of patients with COVID-19; approximately 20% report rashes as the only clinical sign of COVID-19. It is unclear if cutaneous manifestations are associated with COVID-19 severity. The most common cutaneous manifestations include:
- Morbilliform rash: described at onset of illness as well as in recovery
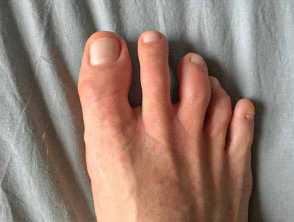
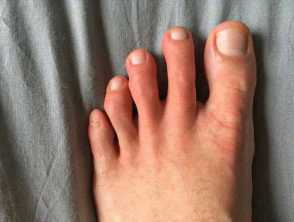
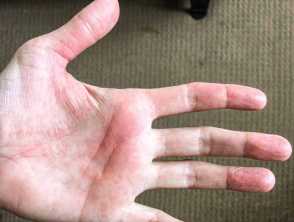
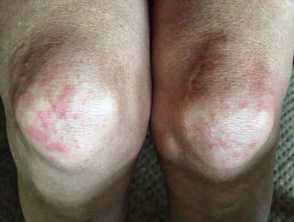
- ‘COVID toes’ (pernio/chilblain-like lesions): likely due to vascular injury caused by the virus
- Livedo reticularis (mottled lace-like eruption)/retiform purpura (purple coloured mottling with leakage of blood, non-blanching)/necrotic vascular lesions
- Acute urticaria
- Vesicular eruptions
- Purpuric eruptions
- Pityriasis rosea-like eruptions
- Cutaneous manifestations of paediatric multisystem inflammatory syndrome (PIMS) include a polymorphic erythematous eruption associated with swelling and redness of the hands and feet as well as oral mucositis and conjunctivitis
- Telogen effluvium (diffuse hair loss) during the recovery phase: usually 2–3 months after COVID infection with full recovery of normal hair density over 4–6 months
- Red half-moon sign in nails
- Other cutaneous manifestations have also been reported.
Cutaneous features due to COVID-19
Oral/mucosal signs of COVID-19
- Transient U-shaped lingual papillitis
- Aphthous ulcers
- Tongue swelling
- Glossitis with patchy depapillation
- Mucositis
- Burning mouth.
How do clinical features vary in differing types of skin?
Cutaneous manifestations of COVID-19 may present differently in darker skin types:
- Urticaria may appear skin-coloured to violaceous
- Maculopapular eruptions may present with more lichenification and hyperpigmentation on or around the lesions
- Exanthems can range from grey to brown to black in colour
- Livedoid and chilblain-like acral rashes may present with less pronounced erythema.
What are the complications of COVID-19?
Complications include hypoxic respiratory failure (acute respiratory distress syndrome or ARDS) that may require intensive care. There have been increasing reports of ‘long COVID’ where symptoms last for 6 weeks or longer. Other potentially fatal complications include:
- Acute kidney injury, which may require dialysis
- Elevated liver enzymes
- Cardiac complications including heart failure, pericarditis, pericardial effusion, arrhythmia, and sudden death
- Venous thromboembolism
- Delirium/encephalopathy.
How is COVID-19 diagnosed?
COVID-19 can be diagnosed using nasopharyngeal swabs.
Real-time reverse-transcriptase polymerase chain reaction (rRT-PCR) tests detect the SARS-CoV-2 virus. Rapid antigen testing (RAT) for the detection of viral proteins can be performed in the office or at home as a point-of-care test. However, it is less sensitive than PCR testing. RATs offer the most utility if performed within a week of symptom onset.
Other viruses can be tested in a similar manner including the influenza virus and respiratory syncytial virus (RSV). Antibody blood tests indicate whether someone has previously been exposed to SARS-CoV-2 and has mounted an immune response.
Breathless patients should have their oxygen saturations checked and monitored. Levels of oxygen saturation <94% on air are considered a marker of severity.
Additional tests can support diagnosis and evaluate severity of COVID-19, including:
- Chest imaging (eg, chest x-ray) showing lung consolidation
- Increased D-dimer
- Increased C-reactive protein (CRP)
- Increased lactate dehydrogenase (LDH)
- Increased troponin
- Increased ferritin
- Increased creatine kinase (CK)
- Reduced lymphocyte count
- Kidney function tests.
As SARS-CoV-2 is excreted in the faeces of infected people, testing of sewage plants has become routine in some countries with low rates of infection. It can inform health authorities of the viral presence in the local community.
What is the differential diagnosis for COVID-19?
- Viral respiratory tract infections including the common cold and influenza
- Bacterial pneumonia
- Tuberculosis
- Congestive heart failure (CHF)
- Chronic obstructive pulmonary disease (COPD)
What is the treatment for COVID-19?
General measures
- Stay at home if mild or asymptomatic COVID-19 to prevent transmission.
- Symptomatic relief with over-the-counter cough and cold medication.
- Those with significant shortness of breath, symptoms of ARDS, or considerable risk factors should consider evaluation in the hospital setting.
- Antiviral medications have the best outcomes earlier in the infection course, thus prompt diagnosis is recommended.
Specific measures
- Remdesivir (intravenous antiviral).
- Nirmatrelvir with ritonavir (oral antiviral for ages >12 years).
- Bebtelovimab (intravenous monoclonal antibody for ages >12 years).
- Molnupiravir (oral antiviral for adults).
Individual patient suitability will include considering factors such as renal function, disease severity, concomitant medication, antiviral availability and accessibility, and duration of disease prior to treatment.
How do you prevent COVID-19?
COVID-19 can be prevented. Many countries have enforced a ‘lockdown’ and have required people to stay at home. Consult your local guidelines for current recommendations.
Physical distancing
Keeping a minimum distance between yourself and others to prevent physical contact and possible contamination is an essential step in preventing the spread of the virus.
- Staying at home during lockdowns; do not go out unless absolutely necessary. Visiting a doctor, supermarket or pharmacy, or physical exercise limited to your neighbourhood is usually permitted; follow your local guidelines.
- Avoid being closer than 2 metres from others.
- Greet people by waving instead of shaking hands.
- Keep in touch with family and friends remotely by phone or via the Internet.
Quarantine
- Many countries have required incoming travellers to enter supervised quarantine with nasopharyngeal swabs on arrival and before release into the community.
- Close contacts of people with COVID-19 have also been asked by some governments to self-quarantine and undergo testing.
- Please consult your local guidelines for up-to-date recommendations.
Hygiene practices
- Wash your hands frequently with soap and water; hand sanitiser with alcohol 60% or higher is also effective.
- Do not touch your eyes, nose, or mouth unless your hands are clean.
- Cough and sneeze into your inner upper arm to prevent contaminating your hands.
- Face masks, when correctly worn, minimise the risk of you passing the virus on to others especially when asymptomatic.
- If tissues are used, throw them away immediately and wash your hands properly.
- Wipe down surfaces using bleach or antiseptic products.
- Don’t share food and drink, toothbrushes, clothing, bedding, or towels.
- If involved in healthcare for patients with COVID-19, wear properly applied personal protective equipment after thorough training in its use.
Vaccination
- In response to the pandemic, a number of vaccines for COVID-19 were developed, and mass vaccination programmes began in December 2020.
- The World Health Organization (WHO) has advised that countries should continue to work towards vaccinating at least 70% of their populations, prioritising the vaccination of health workers and vulnerable groups (eg, people >60 years of age and those who are immunocompromised or have underlying health conditions).
- Vaccination has been found to reduce the risk of transmitting COVID-19 to others, developing severe infection, and requiring hospitalisation.
- Booster doses are recommended to help maintain immunity.
- As at January 2022, vaccines granted Emergency Use Listing (EUL) by WHO included the:
- Pfizer/BioNTech Comirnaty vaccine
- SII/COVISHIELD and AstraZeneca/AZD1222 vaccines
- Janssen/Ad26.COV 2.S vaccine developed by Johnson & Johnson
- Moderna COVID-19 vaccine (mRNA 1273)
- Sinopharm COVID-19 vaccine
- Sinovac-CoronaVac vaccine
- Bharat Biotech BBV152 COVAXIN vaccine
- Covovax (NVX-CoV2373) vaccine
- Nuvaxovid (NVX-CoV2373) vaccine.
See also: COVID-19 immunisation and immunomodulators/biologic agents and skin reactions to COVID-19 vaccines.
What is the outcome for COVID-19?
The outcome for COVID-19 depends on the severity of the illness. Typically, those with mild symptoms will recover within 2 weeks, however, severe cases can take three to six weeks or sometimes longer. Some are describing variable and often debilitating symptoms for months after contracting the infection (‘long COVID’) and this is under active investigation.
Death from COVID-19 has been reported in young, healthy people, although this is not common. Mortality from COVID-19 is highest in older people, especially those over 70 years. Mortality is higher in those with comorbidities associated with severe disease. ICU admission carries a poorer prognosis. National case fatality rates for COVID-19 range between 0.1–5.2% globally.
For more information
In New Zealand, refer to:
- The Government website, https://covid19.govt.nz.
- Wang C, Rademaker M, Baker C, Foley P. COVID-19 and the use of immunomodulatory and biologic agents for severe cutaneous disease: An Australia/New Zealand consensus statement. Australas J Dermatol. 2020 Apr 7. doi: 10.1111/ajd.13313. Epub ahead of print. PMID: 32255510.