What is Cowden syndrome?
Cowden syndrome is a rare, autosomal dominant, inherited condition characterised by hamartomas in various organs, including breast, thyroid, uterus, brain, and mucocutaneous tissues with increased risk of malignancies. It is also known as ‘Cowden disease’ or ‘multiple hamartoma syndrome’.
Cowden disease is one of a spectrum of disorders labelled the PTEN Hamartoma Tumour Syndromes (PHTS), which also include Bannayan-Riley-Ruvalcaba syndrome, Proteus syndrome, and Proteus-like syndrome.
Cowden disease
Who gets Cowden syndrome?
The incidence of Cowden syndrome is 1/200,000, with a female predominance. Most patients have been Caucasian. Skin involvement typically begins in the second or third decade of life.
What causes Cowden syndrome?
Cowden syndrome involves the loss of function mutations in the phosphatase and tensin homolog (PTEN) tumour suppressor gene on chromosome 10q23. This results in over-proliferation of cells that form hamartomatous growths.
Approximately 45% of cases may be caused by de novo mutations in PTEN.
What are the clinical features of Cowden syndrome?
Mucocutaneous features
Hamartomas of the skin and mucosa are present in nearly all cases. They may begin in childhood but may not be clearly evident until the second or third decade of life.
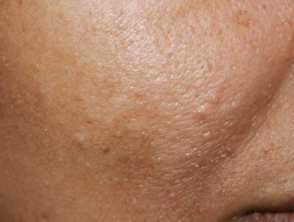
- Trichilemmomas
- Skin coloured or yellow-brown, flat topped, 1–5 mm warty papules on the central face surrounding the eyes, nose, and mouth.
- Sclerotic fibromas
- Well circumscribed, skin-coloured smooth papules.
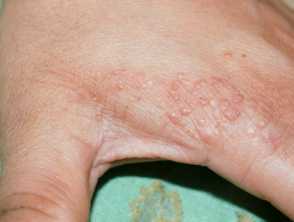
- Acral keratoses
- Hyperkeratotic, warty lesions on the palmoplantar or dorsal surfaces of the hands and feet; sometimes seen on the face and trunk; they are usually clear or translucent with a central indentation.
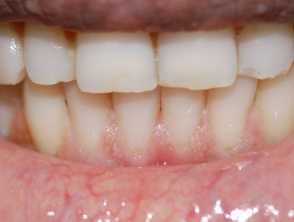
- Oral papillomata
- In particular, the lips, tongue, buccal mucosa, and gingivae are seen in nearly all patients by the second decade.
- Extensive papillomatosis may give a cobblestone appearance to the mucosa.
- Soft tissue lipomas.
- Mucocutaneous neuromas.
- Multiple lentigines of the glans penis.
- Vascular anomalies such as angiolipomas seen in up to 35%.
- Melanoma can be seen in up to 5% of patients.
- Glycogenic acanthosis in up to 80%.
Non-cutaneous features
- Central nervous system
- Lhermitte-Duclos disease (dysplastic gangliocytoma of the cerebellum) is a hamartoma described in 15% of case reports, although the true prevalence is unknown. Its onset may be in childhood or adult life, with adult onset more strongly associated with Cowden disease.
- Autism spectrum disorders are associated. Developmental delay and intellectual disability are seen in about 15% of patients.
- Skeletal
- Macrocephaly in at least 80% of individuals with Cowden disease
- High-arched palate
- Scoliosis
- Thyroid
- Goitre
- Thyroglossal duct cyst
- Thyroid adenoma
- Thyroid cancer in 10–30% of patients, with over-representation of follicular cancer
- Breast
- Fibrocystic disease and fibroadenomas
- Breast cancer (in 85% of females)
- Gastrointestinal
- Hamartomatous gastrointestinal polyps
- Colon cancer
- Genitourinary
- Renal cell carcinoma (lifetime risk may be as high as 34%)
- Endometrial cancer risk of 5–28% with the highest relative risk in women under 50 years of age.
How do clinical features vary in differing types of skin?
The majority of patients reported to have Cowden disease have been Caucasian.
What are the complications of Cowden syndrome?
At least 40% of patients with Cowden disease have at least one cancer. Complications will vary depending on the organ system affected by the malignancy.
How is Cowden syndrome diagnosed?
In 1996, the International Cowden Consortium proposed a set of diagnostic criteria which, with some small adjustments, have been used ever since.
Pathognomonic criteria
Mucocutaneous lesions:
- Trichilemmomas (facial)
- Acral keratoses
- Papillomatous lesions
- Mucosal lesions
Major criteria
- Breast cancer
- Thyroid cancer, particularly follicular thyroid carcinoma
- Macrocephaly (occipital circumference = or > 97th centile)
- Lhermittie-Duclos disease
Minor criteria
- Other thyroid lesions
- Cognitive impairment (IQ = or < 75)
- Hamartomatous intestinal polyps
- Fibrocystic disease of the breast
- Lipomas
- Fibromas
- Genitourinary tumours (uterine fibroids, renal cell carcinoma) or malformations
Cowden syndrome is diagnosed if a patient has any of the following:
- Two major criteria with one being macrocephaly or Lhermittie-Duclos disease
- One major and three minor criteria
- Four minor criteria
- Mucocutaneous lesions or palmoplantar keratosis can meet criteria alone if there are six or more, three of which are trichilemmomas
- Facial papules and oral mucosal papillomatosis
- Oral mucosal papillomatosis and acral keratoses
- Six or more palmoplantar keratoses.
Diagnosis in a family in which one other individual has Cowden disease is made when:
- Any single major criterion with or without minor criteria is met
- Two minor criteria are met.
What is the differential diagnosis for Cowden syndrome?
- Birt-Hogg-Dube syndrome
- Multiple endocrine neoplasia types 1, 2B, and 3
- Bannayan-Riley-Ruvalcaba syndrome
- Tuberous sclerosis
- Sporadic multiple facial tumours; eg, trichilemmomas, trichofolliculomas, and syringomas
- Darier disease
- Oral papillomatosis
What is the treatment for Cowden syndrome?
Patients with Cowden disease need to undergo annual medical and physical examinations, laboratory tests, and radiographic tests to regularly check for internal malignancies.
Genetic counselling of relatives is very important, especially for females who are at most risk for malignant complications.
Treatment of the cutaneous features includes:
- 5-fluorouracil cream
- Oral retinoids, usually acitretin, which may temporarily control some of the cutaneous lesions. Lesions often reappear when treatment is stopped.
- mTOR inhibitors are under investigation
- Surgical care of facial papules using chemical peels, laser resurfacing, surgery and/or shave excisions.
What is the outcome for Cowden syndrome?
If cancers are detected early and treated appropriately, the cure rate is high and life expectancy may be close to normal.