What are antibiotics?
Antibiotics are drugs used to treat bacterial infections.
- They are mainly derived from soil bacteria and fungi, but there are also semi-synthetic and synthetic varieties of antibiotics that are made purely in a laboratory.
- They have several different mechanisms of action, allowing them to be bacteriostatic (inhibit or stop bacterial growth) or bactericidal (kill bacteria).
What is an adverse drug reaction?
An adverse drug reaction (ADR) is an unintended response to a drug at doses normally used for disease therapy. Cutaneous ADRs are ADRs affecting the skin.
Cutaneous adverse reactions to antibiotics
Who gets adverse drug reactions?
Adverse drug reactions are common, particularly in hospital inpatients, with estimates of 2–3% of hospitalised patients experiencing an ADR, and one in 20 of them being potentially fatal.
Cutaneous ADRs account for 10–30% of ADRs, and are most commonly due to antibiotics. The reactions can vary in severity; most are mild-to-moderate, but severe reactions are estimated to occur in 0.1–2% of cases.
How are adverse drug reactions classified?
Adverse drug reactions can be classified as either non-immunological or immunological.
- The majority of ADRs are non-immunologically mediated.
- The reactions are often predictable pharmacological side effects.
- Dose-related ADRs may be due to underlying renal or hepatic disease.
- The ADRs can also be unpredictable and idiosyncratic.
- They can occur on a single occasion or on every occasion the drug is prescribed.
Non-immunological adverse drug reactions
Non-immunological ADRs caused by antibiotics include:
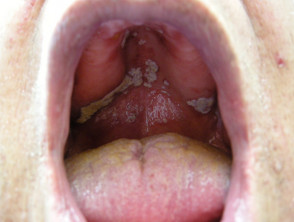
- Infection with other organisms such as yeasts (eg, oral candidiasis or vulvovaginal candidiasis due to broad-spectrum antibiotics, or Malassezia folliculitis or Gram-negative bacterial folliculitis due to long-term treatment with a tetracycline).
- Ototoxicity (damage to the inner ear) due to the build-up of aminoglycosides in renal failure.
- Pellagra can result from long-term use of the anti-tuberculous agents isoniazid and ethionamide due to inhibition of the tryptophan-niacin pathway.
Antibiotic-induced cutaneous infections
Immunological adverse drug reactions
There are four main types of immunologically mediated hypersensitivity or allergic responses to drugs. These immunological ADRs make up approximately 20% of ADRs.
- Type I hypersensitivity reaction is an immediate hypersensitivity reaction to a drug and occurs within minutes to hours, due to pre-formed antigen-specific immunoglobulin (Ig) E antibodies and mast-cell degranulation. This type of reaction results in anaphylaxis, angioedema, and drug-induced urticaria due to rapid vasodilation and increased vascular permeability.
- Type II sensitivity reaction is less common and is due to the development of specific antibodies to the drug, resulting in stimulation or inhibition of immune pathways.
- Type III hypersensitivity reaction results from drug and antibody immune complexities deposited in tissues (eg, cutaneous vasculitis, deposition and subsequent complement activation in the blood vessels of the skin leads to palpable purpura). Type III reactions can occur 1–3 weeks after exposure.
- Type IV hypersensitivity reactions or cell-mediated delayed responses to drugs develop over several hours. They are caused by immune T-cell responses and release of cytokines. Most severe cutaneous adverse reactions are Type IV reactions.
Severe ADRs to some antibiotics, such as Stevens-Johnson syndrome/toxic epidermal necrolysis (SJS/TEN) due to sulphonamides, are caused by complex immunological mechanisms.
How are cutaneous drug reactions classified?
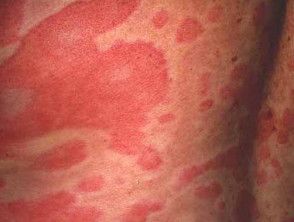
Rashes due to antibiotics are most often morbilliform (exanthematous) or urticarial.
It usually takes 7–10 days to become allergic to a drug, so if a reaction is rapid, it is either non-immunological, or it is due to a previous encounter with the same drug or a chemically similar substance.
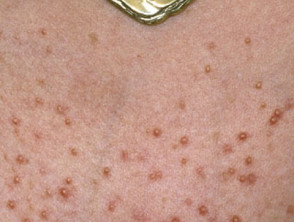
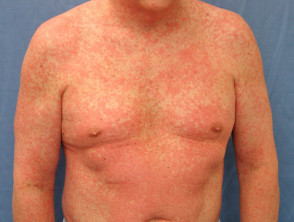
Morbilliform eruption
- Morbilliform eruption is the most common type of antibiotic rash. It is also called an exanthem.
- The exact pathogenesis is unclear. Some morbilliform eruptions do not recur when the patient is re-exposed to the causative drug.
- Many antibiotics cause morbilliform eruptions.
- A morbilliform rash usually starts within 7–14 days of starting a new antibiotic, and lasts for 5–10 days. It may occur more quickly on re-exposure to the same drug.
- It can look similar to a viral exanthem but is usually pruritic, whereas similar viral rashes are not particularly itchy.
- The morphology consists of fine pink macules or papules; hence, it is sometimes called a maculopapular eruption.
- The rash starts as a relatively symmetrical, but often widespread, eruption on the trunk and progresses to involve the proximal limbs and then the distal limbs.
- There is no mucosal involvement.
- The rash may be more prominent on pressure-bearing points.
- Systemic features may include fever and leukocytosis or lymphopenia (reduced lymphocytes) on blood testing.
Acute urticaria
- Acute urticaria is the second most common form of cutaneous drug reaction (see Drug-induced urticaria).
- Many antibiotics can cause urticaria.
- Urticaria presents as pruritic, pale, or erythematous weals.
- Individual weals last less than 24 hours.
- The most common antibiotics causing urticaria are beta-lactams, sulfonamides, and tetracyclines.
Adverse cutaneous reactions to antibiotics
Several other ADRs affecting the skin can be due to antibiotics and are listed below alphabetically.
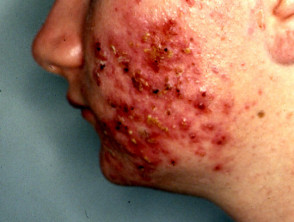
Acneform rash
- An acne-like facial folliculitis can be caused by isoniazid, rifampicin, and tetracyclines.
- Antibiotics may rarely cause a localised pustular eruption called acute localised exanthematous pustulosis.
Acute generalised exanthematous pustulosis
- Acute generalised exanthematous pustulosis (AGEP) is a rare reaction where sterile, superficial, small pustules, 1–2 mm in diameter, develop in areas of extensive erythema.
- AGEP is most often caused by beta-lactams, sulfonamides and tetracyclines.
- It usually develops within 1–2 days of starting a new drug.
- Pustules are followed by desquamation, with healing after approximately two weeks.
- Internal organ involvement is rare.
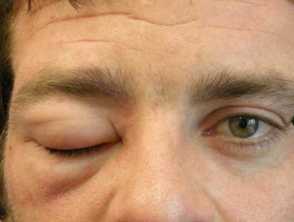
Angioedema and anaphylaxis
- Angioedema, anaphylaxis and urticaria in combination are due to an immediate Type-I hypersensitivity reaction.
- Antibiotics are the most frequent drug cause.
- These reactions are characterised by widespread vasodilation and increased vascular permeability, and subsequent deep soft tissue swelling, hypotension, and airway obstruction.
- Anaphylaxis is a life-threatening medical emergency. Angioedema can also be life-threatening due to airway involvement and can be persistent.
Drug hypersensitivity syndrome
- Drug hypersensitivity syndrome (DHS) is also known as 'drug reaction with eosinophilia and systemic symptoms (DRESS)'.
- Antibiotic causes include sulfonamides and, less often, fluoroquinolones and minocycline. DHS is a rare, life-threatening syndrome typically defined by the triad of fever, skin eruption, and internal organ involvement.
- It usually begins 2–6 weeks after drug exposure.
- There is usually a widespread morbilliform rash, high fever, lymphadenopathy, haematological abnormalities, and internal organ involvement, such as hepatitis.
Severe cutaneous reactions to antibiotics
Drug-induced pemphigus
- Drug-induced pemphigus is caused due to autoantibodies reacting with desmogleins.
- Antibiotic causes of pemphigus include penicillin, cephalosporin and vancomycin.
- Blistering may resolve after drug withdrawal, but more often persists with the same natural history as non-drug-associated pemphigus.
Erythema multiforme
- Erythema multiforme (EM) is characterised by target lesions: these are darker in the centre, paler peripherally, with concentric rings of erythema.
- It is classified into EM minor and EM major (in which there is mucosal involvement).
- EM is most commonly caused by infection, especially by herpes simplex virus.
- Some cases of EM due to antibiotics have been reported. Causative antibiotics include sulfonamides and penicillins.
- Note that EM is a different reaction to SJS/TEN (see below), but these diseases were originally thought to be due to the same immunological process.
Fixed drug eruption
- Fixed drug eruption presents as one or more localised skin lesions that recur with repeated drug exposure in the same location.
- It may be caused by tetracycline antibiotics, trimethoprim + sulphamethoxazole, amoxicillin, ciprofloxacin, clarithromycin, and others; antibiotics in meat have also been incriminated.
- Lesions usually appear 1–2 weeks after the first exposure, and within hours or a few days on subsequent exposure.
- Lesions have a predilection for the face, lips, genitalia, and buttocks, although they can appear anywhere.
- The fixed drug eruption starts an erythematous macule and progresses over a few days to form a blistered plaque.
- The rash may itch or cause a burning sensation.
Hypersensitivity vasculitis
- The hallmark of hypersensitivity vasculitis is palpable purpura (ie, through papules, plaques, bullae, and erosions/ulcers).
- Beta-lactam and sulfonamide antibiotics are the most common group of drugs to cause vasculitis.
- Palpable purpura most commonly affects the lower legs but may become widespread.
- The interval from exposure to the causative drug to the onset of rash ranges from days to weeks.
- Serum sickness-like reaction is a form of hypersensitivity vasculitis with specific skin features: erythema on the sides of fingers, hands, and toes, followed by a more widespread morbilliform or urticarial eruption. The rash usually occurs two weeks after exposure to the causative drug, accompanied by a low-grade fever and arthralgia.
- Complement levels are low in drug-induced hypersensitivity vasculitis.
Blistering adverse reactions to antibiotics
Photosensitive reactions
- Antibiotics such as tetracyclines, sulfonamides and fluoroquinolones may cause drug-induced photosensitivity, which is usually a confluent erythematous rash in sun-exposed areas.
- Minocycline may rarely cause photosensitivity associated with drug-induced lupus erythematosus.
- Isoniazid and ethionamide can rarely cause pellagra which presents as a photosensitive rash.
Stevens–Johnson syndrome / toxic epidermal necrolysis
- SJS/TEN is a serious, potentially fatal, systemic mucocutaneous reaction that is nearly always caused by a drug.
- The most common antibiotics known to cause SJS/TEN are sulfonamides and penicillins, but this reaction has also been reported with many other antibiotics.
- SJS/TEN occurs 4–28 days after the start of drug treatment.
- Management is supportive, and the patient's SCORTEN score can be used to predict morbidity and mortality.
Symmetrical drug-related intertriginous and flexural exanthem (SDRIFE)
- Symmetrical drug-related intertriginous and flexural exanthem (SDRIFE) is a delayed hypersensitivity reaction.
- Amoxicillin and other penicillins account for about 50% of SDRIFE cases.
- SDRIFE characteristically causes erythema in the intergluteal and inguinal folds.
- The rash presents and extends more widely over hours to days.
What is the differential diagnosis for antibiotic reactions?
It is sometimes difficult to determine whether an antibiotic has caused a rash. Drugs are rarely deliberately given to the affected patient again, as re-challenge has the potential to cause a life-threatening response in some cases. This means the true incidence of ADRs is difficult to calculate.
There are important differential diagnoses to consider when examining a suspected cutaneous drug reaction; these include:
- Underlying bacterial infection or toxin-related rash (eg, staphylococcal scalded skin syndrome and toxic shock syndrome)
- Viral exanthems, including measles, rubella, human immunodeficiency virus (HIV), roseola due to human herpes-virus 6, Epstein-Barr virus and many others
- Irritant contact dermatitis
- Folliculitis
- Sweat-induced miliaria or transient acantholytic dermatosis (Grover disease)
- Erythema multiforme due to non-drug causes
- Idiopathic generalised pustular psoriasis (AGEP may mimic this)
- Non-drug-induced cutaneous lupus erythematosus
- Autoimmune blistering diseases
- Other causes of erythroderma (eg, eczema, psoriasis, and lymphoma).
Classification of antibiotics causing cutaneous adverse drug reactions
A large number of antibiotics have the potential to cause cutaneous drug reactions.
Beta-lactams
The four classes of beta-lactam antibiotics are penicillins, cephalosporins, carbapenems, and monolactams. Allergic reactions to beta-lactam antibiotics are the most common cause of immunological ADRs. This is thought to be due to the structure of beta-lactams. IgG antibodies to penicillin can be detected in allergic patients and non-allergic patients taking penicillin.
There is some cross-reactivity between penicillins and cephalosporins. If a patient has an anaphylactic response to penicillins, cephalosporins should be avoided.
Cutaneous ADRs caused by beta-lactams include:
- Anaphylaxis and angioedema
- Morbilliform drug eruption
- Urticaria
- SJS/TEN
- AGEP
- Fixed drug eruption
- Drug-induced pemphigus
- Serum sickness-like reaction.
Though structurally similar, carbapenems can usually be safely used in patients with anaphylactoid reactions to penicillin. The major non-cutaneous side effects of beta-lactam use are diarrhoea, increased Clostridium (Clostridioides) difficile, and drug-induced liver injury, particularly due to clavulanic acid/amoxicillin.
Macrolides
In comparison to most other antibiotics, macrolides are considered relatively safe drugs.
- Their side effects tend to be due to interactions with other drugs, due to their inhibition of the cytochrome p450 system.
- Reports of morbilliform and urticarial rashes, and rarely SJS/TEN, have been reported with macrolides.
- Other non-cutaneous reactions with macrolides include QT prolongation (delayed heart ventricular response) and liver injury.
Tetracyclines
Tetracycline antibiotics are frequently used in dermatology. Possible cutaneous reactions include:
- Photosensitivity — tetracyclines, in particular, doxycycline, are the most common antibiotic cause of photosensitive rashes; it is important to advise the use of sun protection and avoid direct sunlight for one week after treatment
- Fixed drug eruption, most often with doxycycline and minocycline
- Drug-induced lupus erythematosus with minocycline
- Urticaria
- Drug hypersensitivity syndrome with minocycline
- Drug-induced skin pigmentation after prolonged use of minocycline.
Fluoroquinolones
Several older generation fluoroquinolones have been withdrawn from the market due to severe adverse reactions including photosensitivity.
Side effects of current-generation quinolones include tendinopathy and QT prolongation. Common cutaneous reactions include:
- Hypersensitivity vasculitis
- Serum sickness-like reaction
- Morbilliform or urticarial rashes occurs in <0.5–2% of cases; they happen most commonly with ciprofloxacin (1%) and levofloxacin (0.3%)
- Fluoroquinolone photosensitivity can vary in severity, due to how they are altered by light (photodegradability) of the different fluoroquinolones; the most severe reactions are reported with lomefloxacin, with ciprofloxacin causing a mild reaction, and levofloxacin and gemifloxacin are unlikely to cause photosensitivity.
- AGEP
- SJS/TEN.
Sulfonamides
Co-trimoxazole is a sulfonamide antibiotic commonly used in immunocompromised individuals, who are already more at risk of ADRs. The most frequent ADRs are morbilliform or urticarial rash; however, serious ADRs can result, most commonly SJS/TEN. Observed cutaneous drug reactions with sulfonamides include:
- SJS/TEN
- Anaphylaxis
- Fixed drug eruption
- Serum sickness-like reaction
- Drug hypersensitivity syndrome.
Non-cutaneous reactions with sulfonamides include thrombocytopenia, anaemia, and electrolyte abnormalities.
Glycopeptides
- 'Red man' syndrome is a histamine-mediated reaction to the rapid infusion of vancomycin and is not an allergic reaction. This reaction can be minimised by administering the drug slowly when given intravenously.
- Drug hypersensitivity syndrome is also seen with glycopeptides.
- Non-cutaneous adverse reactions include thrombocytopenia.
Other antibiotics
- Aminoglycosides cause urticarial reactions. Renal damage and ototoxicity are serious non-cutaneous adverse reactions with aminoglycosides.
- Metronidazole may cause fixed drug eruption, while peripheral neuropathy is a non-cutaneous reaction of concern.
- Dapsone may cause fixed drug eruption.
- Nitrofurantoin can cause fixed drug eruption and drug-induced lupus erythematosus. Pulmonary fibrosis is a significant non-cutaneous side effect with nitrofurantoin.
How are antibiotic reactions diagnosed?
It is essential to take a careful history in the diagnosis of cutaneous drug reactions. Many affected patients have been taking several drugs. In these cases, it helps to form a timeline, including the initiation of any new drugs and the rash onset.
Sometimes, a skin biopsy will be taken to clarify the inflammatory pattern. The presence of eosinophils can be a helpful clue of an underlying drug cause but is non-specific.
Skin testing is sometimes undertaken, especially for penicillin.
What is the treatment for antibiotic reactions?
The first principle of management is the withdrawal of the causative drug.
Other measures include:
- Frequent emollients to improve dryness and symptoms
- Topical steroids to reduce inflammation and itching
- Oral antihistamines for symptomatic relief of urticaria
- Systemic steroids for drug hypersensitivity syndrome
- Consideration of ciclosporin or intravenous immunoglobulins for SJS/TEN, though there is limited evidence for these measures.
Conclusion
Antibiotics are one of the most significant discoveries in medicine, but they are not without complications.
Cutaneous side effects are commonly experienced and have the potential to be life-threatening, especially in at-risk groups. Among the classes, penicillins, cephalosporins, sulfonamides, and fluoroquinolones are the most common causes of cutaneous reactions, particularly severe ones.