What is cutis verticis gyrata?
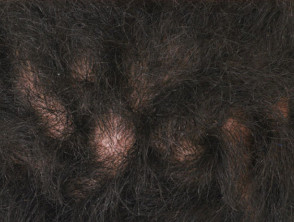
Cutis verticis gyrata is an overgrowth of the scalp skin resulting in convoluted folds and deep furrows of skin that resemble the surface of the brain.
Cutis verticis gyrata
Who gets cutis verticis gyrata?
Cutis verticis gyrata occurs more commonly in males than in females. The primary form of cutis verticis gyrata has a reported male-to-female ratio of 5:1. The incidence of cutis verticis gyrata may be reported as lower in women because longer hair may camouflage the condition.
Most primary cases develop after puberty and typically occur before age 30 years. Some secondary forms of cutis verticis gyrata, such as cerebriform intradermal naevus, can be present at birth.
What is the cause of cutis verticis gyrata?
Cutis verticis gyrata is the result of overgrowth of the scalp skin. It can be classified as:
- Primary essential cutis verticis gyrata: no other associated abnormalities. Primary means the cause of the condition is unknown.
- Primary nonessential cutis verticis gyrata: associated with neuropsychiatric disorders including cerebral palsy, epilepsy, seizures, and ophthalmologic abnormalities, most commonly cataracts.
- Secondary cutis verticis gyrata: consequence of a number of diseases that produce changes in scalp structure including:
- Acromegaly
- Melanocytic naevi (moles)
- Birthmarks, including connective tissue naevus, fibromas and naevus lipomatosus
- Inflammatory processes (eczema, psoriasis, Darier disease, folliculitis, impetigo, atopic dermatitis, acne).
What are the clinical features of cutis verticis gyrata?
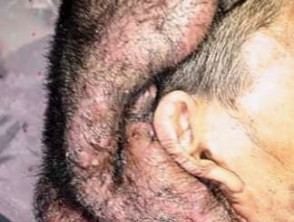
Cutis verticis gyrata typically affects the central and back of the scalp, but some forms can involve the entire scalp. The folds are soft and spongy. The folds are unable to be corrected with pressure. The skin colour is not affected. The number of folds can vary from 2 to more than 10.
Cutis verticis gyrata
How is cutis verticis gyrata diagnosed?
Cutis verticis gyrata is usually a clinical diagnosis.
Investigations may be undertaken for associated neurological conditions or underlying disorders including:
- skin biopsy
- radiology such as MRI.
What is the treatment of cutis verticis gyrata?
The treatment of cutis verticis gyrata includes good scalp hygiene to avoid accumulations of secretions in the furrows of the scalp.
Definitive treatment by surgery may be requested for cosmetic reasons. Small localised lesions can be excised in one procedure. Larger lesions can be removed with serial excision, requiring multiple procedures.
What is the outcome of cutis verticis gyrata?
Cutis verticis gyrata is a progressive condition. It is mainly troublesome due to cosmetic appearance. Rarely, it can be complicated by melanoma developing within a melanocytic naevus.