What is a diabetic foot ulcer?
Diabetic foot ulcer is a skin sore with full thickness skin loss on the foot due to neuropathic and/or vascular complications in patients with type 1 or type 2 diabetes mellitus.
Who gets diabetic foot ulcer?
Diabetic foot ulcer has an annual incidence of 2–6% and affects up to 34% of diabetic patients during their lifetime. Risk factors for developing a diabetic foot ulcer include:
- Type 2 diabetes being more common than type 1
- A duration of diabetes of at least 10 years
- Poor diabetic control and high haemoglobin A1c
- Being male
- A past history of diabetic foot ulcer.
What causes diabetic foot ulcer?
Diabetic foot ulcers are caused by neuropathic and/or vascular complications of diabetes mellitus.
Neuropathic ulcer
High blood sugar levels can damage the sensory nerves resulting in a peripheral neuropathy, with altered or complete loss of sensation and an inability to feel pain. Peripheral neuropathy develops in approximately 50% of adults with diabetes, increasing the risk of injury to the feet from pressure, cuts, or bruises.
Vascular ulcer
Blood vessels can also be damaged by long-standing high blood sugar levels, decreasing blood flow to the feet (ischaemia) and/or skin (microangiopathy). This can result in poor wound healing.
What are the clinical features of diabetic foot ulcer?
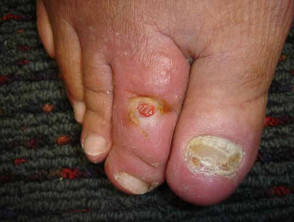
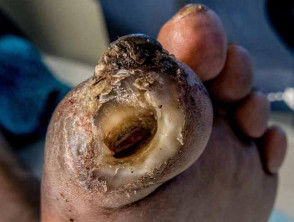
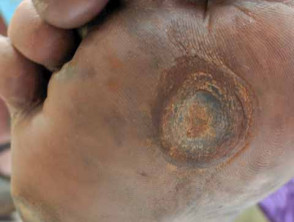
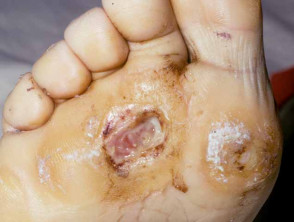
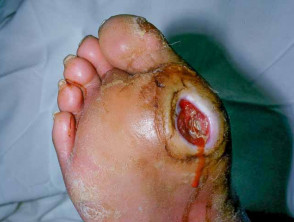
A diabetic foot ulcer is a skin sore with full thickness skin loss often preceded by a haemorrhagic subepidermal blister. The ulcer typically develops within a callosity on a pressure site, with a circular punched out appearance. It is often painless, leading to a delay in presentation to a health professional. Tissue around the ulcer may become black, and gangrene may develop. Pedal pulses may be absent and reduced sensation can be demonstrated.
Diabetic foot ulcer
The severity of a diabetic foot ulcer can be graded and staged. There are many different classification systems. The University of Texas (UT) classification is a widely used, validated system (Table 1).
Table 1. University of Texas (UT) classification of diabetic foot ulcer
| UT Grade | UT Stage |
| 0: Pre- or post-ulcerative or healed wound | A: No infection or ischaemia |
| 1: Superficial wound not involving tendon, capsule, or bone | B: Infection present |
| 2: Wound penetrating to tendon or capsule | C: Ischaemia present |
| 3: Wound penetrating to bone or joint | D: Infection and ischaemia present |
Grading foot ulcer
What are the complications of diabetic foot ulcer?
Diabetic foot ulcer is particularly prone to secondary infection resulting in:
- Wound infection
- Cellulitis
- Osteomyelitis.
How is diabetic foot ulcer diagnosed?
Diabetic foot ulcer is a clinical diagnosis of a painless foot ulcer in a patient with a long history of poorly controlled diabetes mellitus.
Investigations may include:
- Swabs for secondary infection
- X-rays for bone involvement
- Angiography.
What is the differential diagnosis for diabetic foot ulcer?
- An ulcer associated with other causes of peripheral neuropathy, such as leprosy
- Other causes of arterial ulcer
- Venous ulcer
What is the treatment for diabetic foot ulcer?
Prevention of diabetic foot ulcer
- Optimise diabetes control to reduce neuropathic and vascular complications
- Smoking cessation
- Regular examination of the at-risk foot, and careful toenail trimming
- Prompt treatment of non-ulcerative conditions such as tinea pedis or cracked heels
- Appropriate footwear — properly fitting soft shoes or made-to-measure insoles
- Exercise and physiotherapy
- Education of patient, family, and healthcare providers
General measures
- Multidisciplinary care — may include endocrinologist, podiatrist, diabetes education nurse, wound care nurse, neurologist, vascular surgeon, and/or orthopaedic surgeon
- Pressure reduction — appropriate footwear, crutches
- Control of blood sugar levels
- Prevention of secondary infection
Specific measures
- Treatment of secondary infection
- Ulcer debridement
- Dressings
- Adjuvant therapies — negative pressure wound therapy, ulcer excision and grafting, topical or hyperbaric oxygen, human growth factors, and/or amputation
What is the outcome for diabetic foot ulcer?
Diabetic foot ulcer may:
- Heal over weeks to months
- Re-ulcerate — recurrence rate is 40% within one year, 60% by three years, and 65% at five years
- Result in lower extremity amputation in 14–24%.
The five-year mortality rate has been estimated to be 42%.