What is disseminated intravascular coagulation?
Disseminated intravascular coagulation (DIC) presents in a very ill patient as bleeding into the skin (purpura) and other tissues. It arises as a complication of different serious and life-threatening diseases. It covers the continuum of events that occur in the coagulation pathway. Initially, there is uncontrolled activation of clotting factors in the blood vessels, causing clotting of blood throughout the whole body. This depletes the body of its platelets and coagulation factors and results in a paradoxically increased risk of bleeding (haemorrhaging).
Hence, patients with DIC have a loss of balance between the clot-forming activity of thrombin (an enzyme that causes blood to clot) and the clot-lysing activity of plasmin (an enzyme that dissolves blood clots). DIC is not a specific diagnosis and its presence always indicates another underlying disease.
Classification of disseminated intravascular coagulation
There are two clinical forms of DIC, acute DIC and chronic DIC.
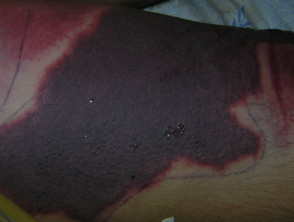
- Acute DIC is a haemorrhagic disorder characterised by multiple bruises (ecchymoses), bleeding from mucosal sites (such as lips and genitals) and depletion of platelets and clotting factors in the blood. Purpura fulminans is a severe and rapidly fatal form of acute DIC. It is sometimes associated with symmetrical peripheral gangrene (tissue death affecting hands and feet).
- Chronic DIC is subtler and involves the formation of blood clots in blood vessels (thromboembolism). Clotting factors and platelets may be normal, increased, or moderately decreased in chronic DIC.
What causes disseminated intravascular coagulation?
Acute DIC is a bleeding disorder caused by a number of conditions.
- The most common causes are infection, including:
- Gram-positive and gram-negative septicaemia (sepsis)
- Meningococcaemia
- Typhoid fever
- Rocky Mountain spotted fever
- Viraemia
- Parasites.
- Obstetric patients are at risk when complications such as abruptio placentae (premature separation of the placenta), amniotic fluid embolism, therapeutic abortions, and eclampsia occur.
- Acute tissue injuries such as certain snakebites, necrotising enterocolitis, freshwater drowning, heat stroke, brain and crush injury, massive tissue destruction, and renal homograft rejection.
Chronic DIC is a thromboembolic disorder that is usually associated with:
- Cancer, especially mucin-producing adenocarcinomas
- Certain severe connective tissue diseases
- Chronic infections (eg, tuberculosis, abscesses, osteomyelitis)
- Giant cavernous haemangioma (Kasabach-Merritt syndrome)
- Chronic kidney disease
- Venous thrombosis or pulmonary embolus (blood clots in legs and lungs)
- Dead fetus syndrome.
What are the signs and symptoms of disseminated intravascular coagulation?
| Acute DIC | Chronic DIC |
|---|---|
|
|
Purpura fulminans
What is the treatment for disseminated intravascular coagulation?
Identifying and treating the underlying disease is the mainstay of management for both acute and chronic DIC. Specific treatment of DIC may or may not be required depending on the signs and symptoms present.
| Treatment of acute DIC | |
|---|---|
| Without bleeding or evidence of ischaemia | No treatment required, observe |
| With bleeding | Blood components:
|
| With ischaemia | Anticoagulants such as heparin or low molecular weight heparin (LMWH) after bleeding is corrected with blood products |
| Treatment of chronic DIC | |
| Without thromboembolism | No specific therapy but prophylactic anticoagulants (e.g. low-dose heparin, LMWH) may be used for patients at high risk of thrombosis |
| With thromboembolism | Anticoagulant therapy with heparin or LMWH A trial of warfarin (variable response between patients) |