What is drug-induced pigmentation?
Drug-induced pigmentation is a change in skin pigmentation due to a change in melanin synthesis, or the accumulation of drugs or their metabolites in the skin.
Common causes include chemotherapy, antimalarials, and nonsteroidal anti-inflammatory drugs. Hyperpigmentation is more common and results from the deposition of melanin or the implicated drug in an uneven manner, while hypopigmentation develops from melanin deficiency.
Drugs are responsible for 10–20% of acquired hyperpigmentation. Other causes include sun damage, hormonal changes, or inflammation.
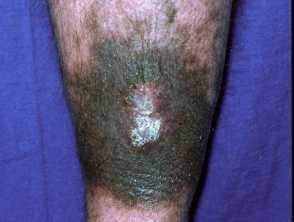
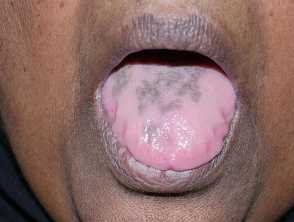
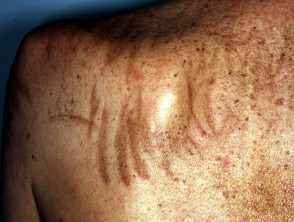
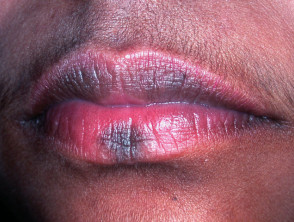
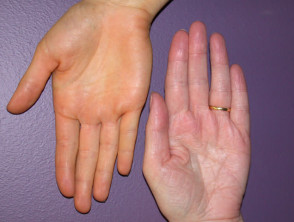
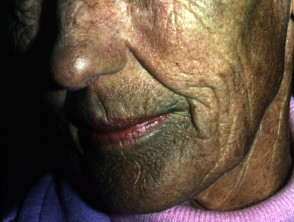
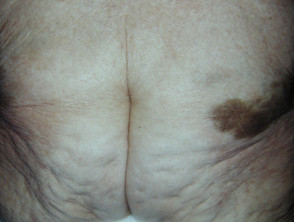
Blue-grey pigmentation due to long term amiodarone use Blue pigmentation due to long-term minocycline use for pyoderma gangrenosum Pigmentation of the tongue from hydroxychloroquine administration Bleomycin-induced flagellate hyperpigmentation Hyperpigmentation on the lip after resolution of an acute fixed drug eruption Orange pigmentation on the palm due to betacarotene medication Diffuse facial pigmentation due to a phenothiazine Pigmentation on the buttock due to iron after intramuscular injection for iron deficiency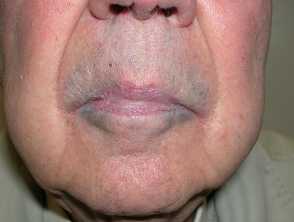
Who gets drug-induced pigmentation?
Drug-induced pigmentation affects all skin types and ethnicities, but certain combinations of skin types and medications may experience more significant pigmentation effects.
- More common in women and people of Asian or African descent.
- Incidence depends on the drug in question, its dosage, and the duration of therapy.
- Drug-induced hypopigmentation is less common than drug-induced hyperpigmentation.
- A meta-analysis found that 3.2% of patients on antimalarials experienced drug-induced hyperpigmentation.
What causes drug-induced pigmentation?
Medications that can cause drug-induced pigmentation include:
- Antimalarials
- Chemotherapeutic agents
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Antipsychotics
- Amiodarone
- Anticonvulsants
- Minocycline
- Heavy metals.
Kratom, a herbal substance used historically most often in South East Asia, can cause photodistributed hyperpigmentation. Its use in other parts of the world is increasing.
The pathophysiology is not completely understood and varies depending on the drug; proposed mechanisms for hyperpigmentation include:
- Indirect toxicity to the skin/melanocyte damage — eg, bleomycin and doxorubicin melanocyte damage
- Accumulation of drug/ drug metabolites in the skin — eg, chloroquine and hydroxychloroquine
- Immune mediation or an allergic reaction resulting in inflammation and pigment deposition — eg, gold (immune-mediated reaction)
- Stimulation of melanin production — eg, oral contraceptives and hormone replacement therapy (HRT) may stimulate melanin production
- Formation of drug-protein complexes causing inflammation and melanin deposition — amiodarone is proposed to cause pigmentation this way.
Drug-induced pigmentation may also be dictated by genetic variables. Those with polymorphisms in the UGT1A4 gene, for instance, may be more vulnerable to chloroquine-induced pigmentation.
What are the clinical features of drug-induced pigmentation?
Clinical features vary widely depending on the drug involved, duration of treatment, and individual patient characteristics.
Cutaneous features include:
- Hyperpigmentation
- Hypopigmentation
- Mottled pigmentation: with both hyper- and hypopigmentation
- Blue-grey pigmentation: particularly in sun-exposed areas
- Orange-yellow pigmentation: particularly in the palms and soles.
Non-cutaneous features include:
- Ocular changes: pigmentation in the conjunctiva or sclera
- Nail changes: pigmentation of nails and surrounding skin
- Oral mucosa changes: pigmentation of the oral mucosa results in a blue-black discolouration of gums and tongue.
The pattern of pigmentation may suggest a particular implicated drug; localised pigmentation on the face, lip, or genitalia may suggest a resolved fixed drug eruption. Flagellate pigmentation is a feature of a bleomycin eruption.
The following table details the clinical features with reference to each class of drug.
| Drug/drug group | Clinical features |
| Heavy metals (iron, gold, silver) |
|
| Tetracyclines (minocycline, doxycycline) |
|
| Antipsychotics (chlorpromazine and related phenothiazines) |
|
| Anticonvulsants |
|
| Antimalarials |
|
| Cytotoxic drugs |
|
| Amiodarone |
|
| NSAIDs |
|
Drug-induced pigmentation images
How do clinical features vary in differing types of skin?
Drug-induced pigmentation can affect any skin type, especially those with Fitzpatrick skin phototypes IV to VI.
What are the complications of drug-induced pigmentation?
Complications are largely cosmetic. Some pigmentation changes may be irreversible, even after the causative medicine has been discontinued. However, some skin changes may represent serious underlying illnesses, such as drug-induced lupus erythematosus.
How is drug-induced pigmentation diagnosed?
- The diagnosis is clinical and relies on the patient’s medication history and pattern of pigmentation, including its location, colour, and distribution on the body.
- The time course between the commencement of the drug and the emergence of pigmentation can be highly variable.
- Skin biopsy can be performed to confirm the diagnosis and exclude other conditions. The biopsy may show pigment in the dermis or epidermis and allergic-like inflammatory changes, but the histopathological features are non-specific.
- Patch or skin prick testing can be used to test for an allergic response as some cases are allergic in nature.
What is the differential diagnosis for drug-induced pigmentation?
- Postinflammatory hyperpigmentation
- Melasma
- Lichen planus pigmentosus
- Drug-induced photosensitivity
- Haemochromatosis
- Addison disease
- Wilson disease
- Vitamin deficiencies
- Naevus of Ota, Ito, or Hori
- Other pigmentation disorders such as idiopathic and drug-induced vitiligo
What is the treatment for drug-induced pigmentation?
General measures
- Discontinue the causative medication, if possible.
- Sun protection is essential to prevent the worsening of pigmentation.
- In most cases, the pigmentation will resolve over time once the medication is stopped; however, it may be prolonged or permanent.
Specific measures
- Persistent pigmentation can be very challenging to treat.
- Topical therapies such as hydroquinone, retinoids, and azelaic acid may be helpful.
- Chemical peels and laser therapy can sometimes be effective.
- Laser treatment has been successful in treating amiodarone-induced skin pigmentation, however, it can also lead to postinflammatory hyper- and hypopigmentation so should only be carried out by those with experience.
How do you prevent drug-induced pigmentation?
- Avoid medications known to cause pigmentation changes in individuals with a history of drug-induced pigmentation or those at risk for developing it.
- Sun protection to prevent exacerbation of existing pigmentation changes.
What is the outcome for drug-induced pigmentation?
Prognosis is generally good, as drug-induced pigmentation typically fades over time after discontinuing the causative medication. In rare cases, the pigmentation may be permanent.