What are epidermal naevus syndromes?
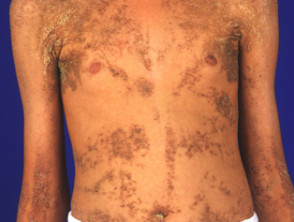
An epidermal naevus is a type of birthmark in which there is an overgrowth of one or more components of the epidermis or outer layer of skin. Epidermal naevus syndromes refer to the co-existence of a keratinocytic epidermal naevus or an organoid naevus with other abnormalities in the skin and other organs. They are sometimes called systematised epidermal naevi. They reflect mosaicism, in which there are two distinct cell lines with different genetics and are due to postzygotic mutation.
The epidermal naevus syndromes usually arise sporadically, with the exception of CHILD syndrome, which is familial.
Several authors have commented that the term 'epidermal naevus syndrome' is outdated now that the genetic causes are known for many of the disorders.
Keratinocytic epidermal naevus syndromes
Keratinocytic epidermal naevus
Three syndromes associated with a keratinocytic epidermal naevus are now well defined.
- CHILD (congenital hemidysplasia with ichthyosiform naevus and limb defects) syndrome
- Type 2 segmental Cowden disease
- Fibroblast growth factor receptor three epidermal naevus syndrome
CHILD syndrome
CHILD syndrome is inherited as an X-linked dominant disorder and is lethal in males. CHILD stands for Congenital Hypoplasia with Ichthyosiform naevus and Limb defects. It is due to mutations in the gene known as NSDHL (or NAD[P]H steroid dehydrogenase-like gene). This gene involved in the metabolism of cholesterol.
The CHILD naevus is variable, inflamed and covered by waxy yellowish scales. It is usually either strictly on one side of the body (most often the right) with clear-cut midline demarcation, or it may follow Blaschko lines or both. It often favours a body fold. The pathology characteristically shows foamy histiocytes in the dermal papillae. CHILD naevus can spontaneous disappear only to reappear later.
Other features may include:
- Thickened abnormal nails
- Strawberry-like lesions on the tips of a finger or toe
- Skeletal defects – shortened or absence finger(s) or limb(s)
- Long bone Xray changes – chondrodysplasia punctata
- The undergrowth of other bones
- Congenital heart, kidney or other organ defects
- Neurological diseases.
Type 2 segmental Cowden disease
Multiple hamartoma syndrome or Cowden disease can include a Cowden naevus when it is called Type 2 segmental Cowden disease. The Cowden naevus is a linear, thick, bumpy, wart-like growth. PTEN (phosphatase and tensin homologue) gene mutations have been detected, which are not present in Proteus syndrome, which type 2 segmental Cowden syndrome may resemble (see below). The PTEN gene's normal function is to suppress tumours. The features of Type 2 segmental Cowden disease include:
- Linear Cowden naevus
- Other naevi: vascular malformation, lymphatic malformation, lipomas
- Neurological defects including hydrocephalus, seizures
- Overgrowth of limbs and toes
- Jejunal or colonic polyps.
Fibroblast growth factor receptor three epidermal nevus syndrome
Fibroblast growth factor receptor 3 (FGFR3) epidermal naevus syndrome (García-Hafner-Happle syndrome) is caused by a mosaic R248C mutation of the FGFR3 Gene.
Organoid naevus syndromes
Sebaceous naevus
Schimmelpenning syndrome
Schimmelpenning syndrome has two Online Mendelian in Man entries (OMIM 163200, 601359). Its other names include:
- Schimmelpenning-Feuerstein-Mims syndrome
- SFM syndrome
- Linear sebaceous naevus syndrome
- Jadassohn naevus phakomatosis
- Naevus sebaceous of Jadassohn
- Organoid naevus phakomatosis.
Features include:
- Sebaceous naevus – which may have a minimal sebaceous overgrowth
- Skeletal defects – deformities of the face, trunk and limbs
- Ocular defects – conjunctival or corneal growth or coloboma
- Cerebral defects – intellectual disability, seizures, enlarged or shrunken brain tissue
- Hypophosphataemic rickets – vitamin D-deficient bone disease.
Phakomatosis pigmentokeratotica
Phakomatosis (sometimes spelt phacomatosis) pigmentokeratotica is an example of didymosis (twin spotting) because two distinct syndromes appear to overlap in one person. It is characterised by:
- Sebaceous naevus
- Papular naevus spilus (speckled lentiginous naevus).
Naevus spilus is a type of congenital melanocytic naevus. It presents as a flat brown café au lait macule in a baby and later develops darker speckles and papules.
Phakomatosis pigmentokeratotica may include features associated with Schimmelpenning syndrome (above) and with papular naevus spilus syndrome. These are:
- Hyperhidrosis (excessive sweating)
- Muscular weakness
- Dysaesthesia (sensory disturbance).
Many other abnormalities have been described in individual cases.
Didymosis aplasticosebacea
Didymosis aplasticosebacea is the association of sebaceous naevus with aplasia cutis congenita.
SCALP syndrome
SCALP syndrome is didymosis aplasticosebacea in association with a giant melanocytic naevus. The name is an acronym for Sebaceous naevus, Central nervous system abnormalities, Aplasia cutis, Limbal dermoid, and Pigmented naevus.
Comedo naevus syndrome
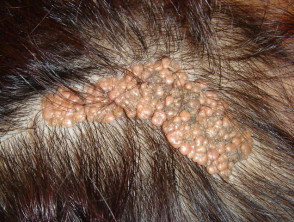
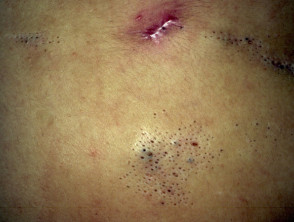
The comedo naevus is composed of a group of open comedones plugged with keratin and may arise on the head, trunk or limbs. The comedo naevus has sometimes been reported in association with other defects:
- Cataract on the same side as the naevus
- Bone defects on the same or opposite side
- Webbing of the fingers or toes (syndactyly)
- Neurological defects on the same or opposite side.
Various other features have been described in individual cases.
Comedone naevus
Angora hair naevus syndrome
The Angora hair naevus is an epidermal naevus covered with long soft white hair. The Angora hair naevus or Schauder syndrome may also include:
- Neurological defects — such as intellectual disability, seizures, spasticity, hemiparesis
- Optic defects — such as cataract and coloboma
- Skeletal defects — mainly facial malformations such as frontal bossing, malformed ears and large tongue.
Becker naevus syndrome
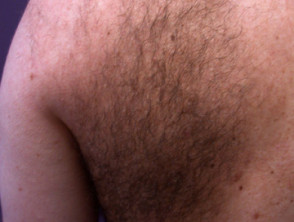
The Becker naevus presents as darkened skin patches, often with a map-like or checkerboard outline. It is most commonly found on the upper back or shoulders. It tends to be more prominent in males because of the growth of dark hair within it at puberty. The syndrome may also include:
- Poor breast or nipple development on the affected side – more obvious in females
- Supernumerary nipples
- Loss of subcutaneous fat
- Loss of axillary hair
- Musculoskeletal abnormalities and asymmetry.
Becker naevus
Differential diagnosis of epidermal naevus syndromes
Proteus syndrome
Proteus syndrome is characterised by overgrowth of skin, connective tissue, fat, bones and other tissues.
- Soft, velvety, flat keratinocytic epidermal naevus in 50% of cases
- Other naevi, e.g., vascular malformation, lymphatic malformation, cutis aplasia, lipomas
- Brain-like (cerebriform) overgrowth of palms or soles
- Enlarged finger(s) or toe(s)
- Overgrowth of any other bone or tissue
- Neurological defects including mild intellectual disability and seizures
Other epidermal naevus syndromes
There are numerous individual case reports or small series of cases that do not fit into the descriptions above. Some of these have been given names:
- Naevus trichilemmocysticus syndrome
- Gobello syndrome: epidermal naevus characterised by hypertrichosis and follicular hyperkeratosis in association with multiple bone defects.
- NEVADA syndrome: Naevus Epidermicus Verrucosus with AngioDysplasia and Aneurysms
- CLOVE syndrome: Congenital Lipomatous Overgrowth, Vascular malformations and Epidermal naevus (similar but distinct from Proteus syndrome).
Verrucous epidermal naevus with skeletal defects
How are epidermal naevus syndromes diagnosed?
The epidermal naevus syndromes are diagnosed clinically by a careful history and examination. Supportive investigations in a child with systemic or neurological symptoms may include:
- Skeletal survey
- Chest X-ray
- Computerised tomography (CT) scan or magnetic resonance imaging (MRI)
- Molecular testing.
What is the treatment for epidermal naevus syndromes?
A multidisciplinary approach is often necessary to optimise the management of symptoms. There is no cure.