What is erysipelas?
Erysipelas is a superficial form of cellulitis, a potentially serious bacterial infection affecting the skin.
Erysipelas affects the upper dermis and extends into the superficial cutaneous lymphatics. It is also known as St Anthony's fire due to the intense rash associated with it.
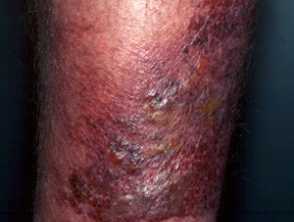
Erysipelas
Who gets erysipelas?
Erysipelas most often affects infants and older people but can affect any age group. Risk factors are similar to those for other forms of cellulitis. They may include:
- Previous episode(s) of erysipelas
- Breaks in the skin barrier due to insect bites, ulcers and chronic skin conditions such as psoriasis, athlete’s foot and eczema
- Current or prior injury (eg, trauma, surgical wounds, radiotherapy)
- In newborns, exposure of the umbilical cord and vaccination site injury
- Nasopharyngeal infection
- Venous disease (eg, gravitational eczema, leg ulceration) and lymphoedema
- Immune deficiency or compromise, such as
- Nephrotic syndrome
- Pregnancy.
What causes erysipelas?
Unlike cellulitis, almost all erysipelas is caused by Group A beta-haemolytic streptococci (Streptococcus pyogenes). Staphylococcus aureus, including methicillin-resistant strains (MRSA), Streptococcus pneumoniae, Klebsiella pneumoniae, Yersinia enterocolitica, and Haemophilus influenzae have also been found rarely to cause erysipelas.
What are the clinical features of erysipelas?
Symptoms and signs of erysipelas are usually abrupt in onset and often accompanied by fevers, chills and shivering.
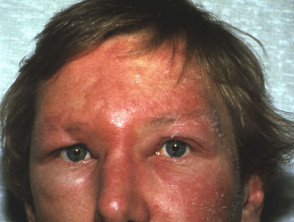
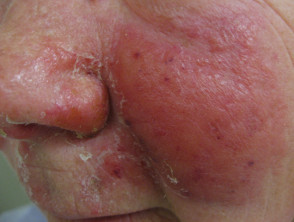
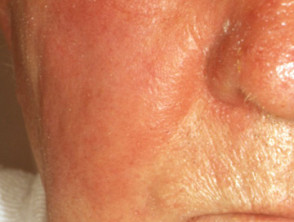
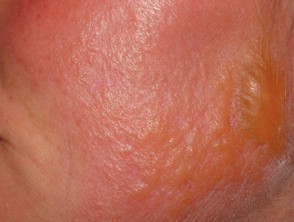
Erysipelas predominantly affects the skin of the lower limbs, but when it involves the face, it can have a characteristic butterfly distribution on the cheeks and across the bridge of the nose.
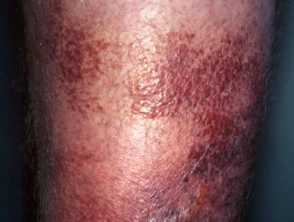
- The affected skin has a very sharp, raised border.
- It is bright red, firm and swollen. It may be finely dimpled (like an orange skin).
- It may be blistered, and in severe cases may become necrotic.
- Bleeding into the skin may cause purpura.
- Cellulitis does not usually exhibit such marked swelling but shares other features with erysipelas, such as pain and increased warmth of affected skin.
- In infants, it often occurs in the umbilicus or diaper/napkin region.
- Bullous erysipelas can be due to streptococcal infection or co-infection with Staphylococcus aureus (including MRSA).
Erysipelas
What are the complications of erysipelas?
Erysipelas recurs in up to one-third of patients due to:
- Persistence of risk factors
- Lymphatic damage (hence impaired drainage of toxins).
Complications are rare but can include:
- Abscess
- Gangrene
- Thrombophlebitis
- Chronic leg swelling
- Infections distant to the site of erysipelas
- Infective endocarditis (heart valves)
- Septic arthritis
- Bursitis
- Tendonitis
- Post-streptococcal glomerulonephritis (a kidney condition affecting children)
- Cavernous sinus thrombosis (dangerous blood clots that can spread to the brain)
- Streptococcal toxic shock syndrome (rare).
How is erysipelas diagnosed?
Erysipelas is usually diagnosed by the characteristic rash. The differential of erysipelas is similar to the cellulitis mimics. There is often a history of a relevant injury. Tests may reveal:
- Raised white cell count
- Raised C-reactive protein
- Positive blood culture identifying the organism.
MRI and CT are undertaken in case of deep infection.
For the skin biopsy findings, see erysipelas pathology.
What is the treatment for erysipelas?
General
- Cold packs and analgesics to relieve local discomfort
- Elevation of an infected limb to reduce local swelling
- Compression stockings
- Wound care with saline dressings that are frequently changed.
Antibiotics
- Oral or intravenous penicillin is the antibiotic of first choice.
- Erythromycin, roxithromycin or pristinamycin may be used in patients with penicillin allergy.
- Vancomycin is used for facial erysipelas caused by MRSA
- Treatment is usually for 10–14 days
What is the outlook for erysipelas?
While signs of general illness resolve within a day or two, the skin changes may take some weeks to resolve completely. No scarring occurs.
Long term preventive treatment with penicillin is often required for recurrent attacks of erysipelas.
Erysipelas recurs in up to one-third of patients due to the persistence of risk factors and also because erysipelas itself can cause lymphatic damage (hence impaired drainage of toxins) in involved skin which predisposes to further attacks.
If patients have recurrent attacks, long term preventive treatment with penicillin may be considered.