Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Sonya Havill MBChB FRACP, Department of Dermatology, Waikato Hospital, New Zealand, 2001.
Reviewing dermatologist: Dr Ian Coulson (2023)
Introduction Purpose Scarring What to expect Wound aftercare
Excision biopsy refers to the removal of a skin lesion by completely cutting it out.
A common reason to excise a skin lesion is to remove skin cancer, such as a basal cell carcinoma, squamous cell carcinoma or melanoma.
Other reasons to remove a skin lesion include:
It is impossible to fully excise a skin lesion without scarring in some way. Careful surgical technique should aim to minimise scarring, for example by taking the skin surface tension lines into account.
Some people have an abnormal response to skin healing and these people may get larger and thicker scars than usual (keloid or hypertrophic scarring).
Your dermatologist will explain to you why the skin lesion needs excision and the procedure involved. You may have to sign a consent form to indicate that you understand and agree to the surgical procedure. Tell your doctor if you are taking any medication (particularly aspirin, clopidogrel, dabigatran and warfarin, which could make you bleed more), or if you have any allergies, medical conditions, or a pacemaker or implanted defibrillator. Remember, to tell your doctor about any over-the-counter supplements or herbal remedies as a number of these can also lead to abnormal bleeding.
The most common type of excision is an elliptical excision. The ellipse is often designed so that the resulting scar runs parallel with existing skin creases. This usually provides a wound under less tension and orientates the scar in a direction which is less noticeable to the eye.
The area to be excised is marked with a surgical marker. A local anaesthetic injection will rapidly numb the area of skin involved and keep it numb during the procedure. The dermatologist will then cut around and under the lesion with a scalpel and sharp scissors along with an appropriate margin of normal surrounding tissue. The lesion is placed in formalin ready to go to the pathology laboratory. Here, a pathologist will process and examine the specimen under the microscope, and provide your doctor with a report a few days later.
There may be some bleeding in the area from where the lesion has been removed during the surgery. The doctor may coagulate the blood vessels with a cautery. This can make a hissing sound and a burning smell, but will not be felt.
The edges of the ellipse will then be sewn together to make a thin suture line. This type of wound closure is called primary closure. There may be two layers of sutures (stitches) a layer underneath that is absorbable and a layer of sutures on the surface which will need to be removed in 4-14 days. Occasionally special skin glue is used to join the edges together, instead of sutures.
A dressing may be applied and instructions will be given on how to care for your wound and when to get the stitches out.
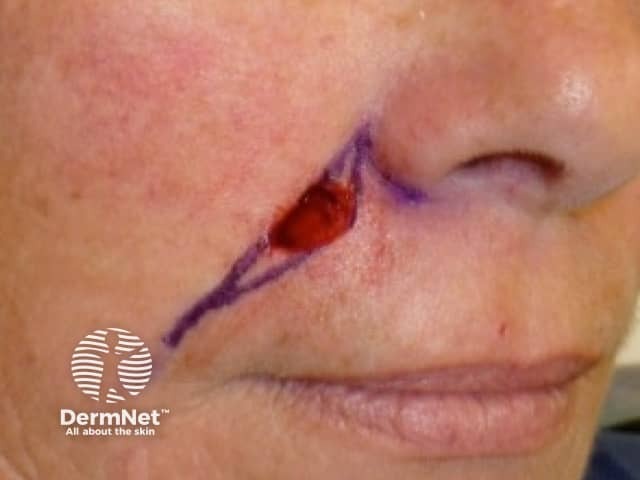
Excision wound
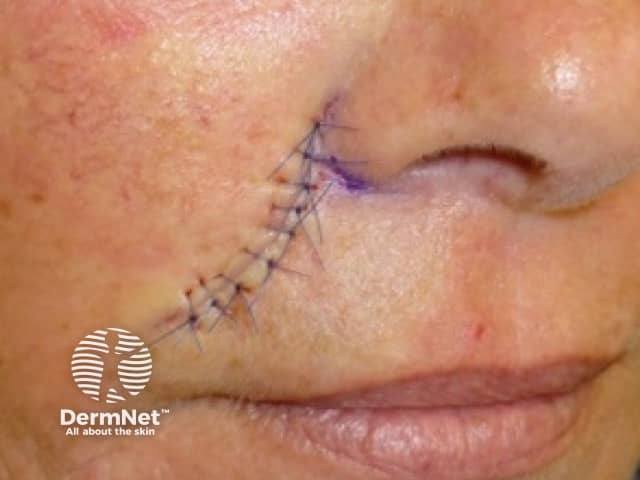
Sutured wound
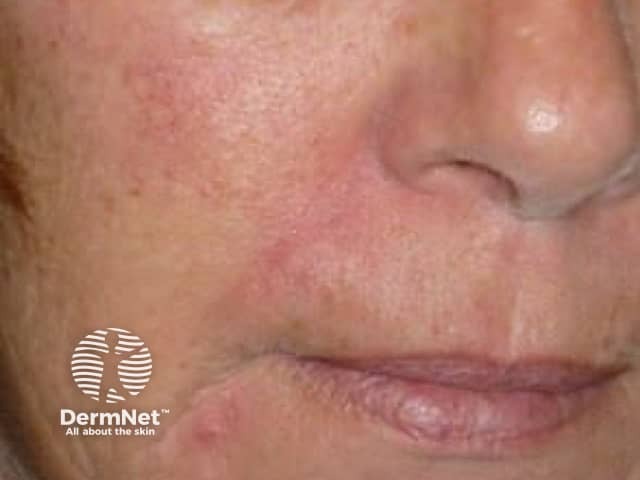
Healed wound
Your wound may be tender 1–2 hours after the excision when the local anaesthetic wears off.
Leave the dressing in place for 48 hours or as advised by your dermatologist. Avoid strenuous exertion and stretching of the area until the stitches are removed and for some time afterwards.
If there is any bleeding, press on the wound firmly with a clean folded towel without removing the existing dressing or looking at it for 20 minutes. If it is still bleeding after this time, seek medical attention.
Keep the wound dry for 48 hours. You can then gently wash and dry the wound. A small amount of pinkness and tenderness to touch around the wound edges is normal but, if the wound becomes increasingly red or painful, consult your dermatologist promptly — it could be infected and need a course of antibiotics.
The scar will initially be red and raised but usually reduces in colour and size over several months.