What is exercise-induced anaphylaxis?
Exercise-induced anaphylaxis is a rare but potentially fatal hypersensitivity reaction triggered by physical activity. Symptoms are due to massive degranulation of mast cells. They include:
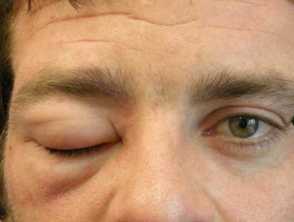
- Urticaria and angioedema
- Nausea and vomiting
- Respiratory difficulty due to airway constriction
- Hypotension (shock).
Urticaria and angioedema
What causes exercise-induced anaphylaxis?
The pathophysiology of exercise-induced anaphylaxis is not fully understood. Symptoms are caused by histamine and tryptase, which are released on the activation and degranulation of mast cells. Patients with exercise-induced anaphylaxis show a decrease in the threshold for mast cell degranulation, but the reason for this is unknown.
Who gets exercise-induced anaphylaxis?
Exercise-induced anaphylaxis accounts for 5–15% of cases of anaphylaxis. The prevalence of exercise-induced anaphylaxis is thought to be approximately 50 to 2,000 episodes per 100,000 persons per year.
Most affected patients partake in regular exercise but only occasionally experience anaphylaxis.
Exercise-induced anaphylaxis is usually sporadic, but there are some reported familial cases. Onset typically occurs between 10–30 years of age, but cases have been reported in children as young as 3 years. Women are twice as likely as men to experience exercise-induced anaphylaxis.
What kind of exercise triggers exercise-induced anaphylaxis?
Symptoms are usually triggered during moderate exercise, such as jogging, tennis, dancing, and cycling. Episodes are not fully predictable, as the same exercise may not trigger exercise-induced anaphylaxis every time.
What are the clinical features of exercise-induced anaphylaxis?
The clinical features of exercise-induced anaphylaxis are similar to other types of anaphylaxis. Typically, symptoms start within 30 minutes of beginning exercise, but they may occur at any time during physical activity. As exercise progresses, the symptoms become more severe, to the point of cardiovascular collapse. Ceasing exercise usually results in immediate improvement, but some patients continue to experience symptoms for up to 1 hour afterwards. The main systems and organs affected are the skin, respiratory tract, gastrointestinal tract, and cardiovascular system.
Prodromal symptoms include fatigue, generalised pruritus and erythema. Commonly, these are followed by:
- Pruritus (92%)
- Urticaria (86%)
- Angioedema (72%)
- Flushing (70%)
- Shortness of breath (51%).
Less frequently, exercise-induced anaphylaxis may be accompanied by gastrointestinal symptoms such as nausea, vomiting, abdominal cramping and diarrhoea, as well as syncope, dysphagia, chest tightness, sweating, choking, throat constriction, headache and hoarseness.
Food-dependent exercise-induced anaphylaxis
Food-dependent exercise-induced anaphylaxis affects one–third to a half of patients with exercise-induced anaphylaxis. An anaphylactic response can occur when exercise is taken between 1 and 3 hours after eating. Symptoms do not occur after food without exercise, nor do they occur during exercise if the triggering food has not been consumed.
The main foods likely to cause food-dependent exercise-induced anaphylaxis are:
- Wheat
- Shellfish
- Tomatoes
- Peanuts
- Corn.
Symptoms are the same as in exercise-induced anaphylaxis.
What are the complications of exercise-induced anaphylaxis?
One–third of patients with exercise-induced anaphylaxis experience cardiovascular symptoms, including fainting or altered consciousness. Death from exercise-induced anaphylaxis is rare, although this condition can be life-threatening and has to be treated urgently.
How is exercise-induced anaphylaxis diagnosed?
Diagnosis of exercise-induced anaphylaxis is based on clinical history and physical examination. The triggering events of the anaphylaxis should be determined, such as whether it is induced by exercise alone or has some association with food.
What is the differential diagnosis of exercise-induced anaphylaxis?
Other kinds of anaphylaxis that may accompany exercise include cold urticaria (exposure to cold while swimming) or drug–induced anaphylaxis (due to non-steroidal anti-inflammatory drugs [NSAIDs] taken during exercise).
If there is not a clear history of anaphylaxis, other disorders must be considered, including:
- Cholinergic urticaria
- Mastocytosis
- Hereditary angioedema
- Exercise-induced asthma
- Idiopathic anaphylaxis
- Phaeochromocytoma.
What is the treatment for exercise-induced anaphylaxis?
Anaphylaxis must be treated as a medical emergency. Management of exercise-induced anaphylaxis is similar to other types of anaphylaxis.
Treatment of type I hypersensitivity reactions includes:
- Adrenaline (intramuscularly, to decrease airway swelling and cardiovascular symptoms)
- Systemic glucocorticosteroids (to decrease the inflammatory reaction)
- Antihistamines (to counteract the effect of released histamine).
Patients should avoid the anaphylactic trigger in future. If exercise is part of the regular routine of a patient, they may need to be instructed on the use of an adrenaline pen or a pre-loaded adrenaline syringe for emergency situations. Patients should know how to identify the early symptoms of exercise-induced anaphylaxis.