Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Gout is a common disorder, which affects around 1% of the population. It is caused by excess uric acid, which exists as ionised urate in the blood. Saturated plasma urate (blood levels above 0.42 mmol/L) may slowly form monosodium urate (MSU) crystals that are deposited in the joints, kidneys, and soft tissues, eventually resulting in arthritis, kidney damage, and lumps under the skin respectively.
In healthy individuals, uric acid / urate is formed after eating certain high-protein foods. Usually most of the uric acid is then excreted by the kidneys in the urine. Excess urate in the blood can result from:
Other risk factors for gout include:
In most cases, the first attack of gout presents with extreme pain and swelling in a single joint, often the big toe (podagra). The pain begins abruptly and the joint is red, hot, and extremely tender. Occasionally the first attack of gout affects multiple joints simultaneously. Patients may have a fever, particularly if many joints are involved. Untreated attacks of gout usually last 7-10 days, following which the patient may be symptom-free until the next attack.
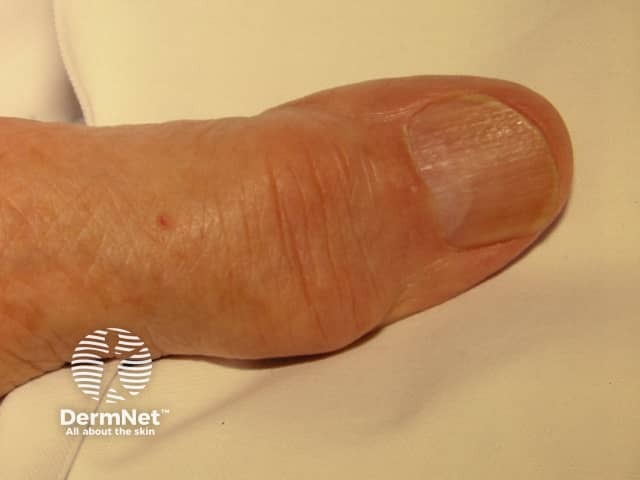
Acute gout
Initially, attacks of gout may be months or years apart. An attack of gout can be brought on by:
If gout remains untreated, the following complications can occur:
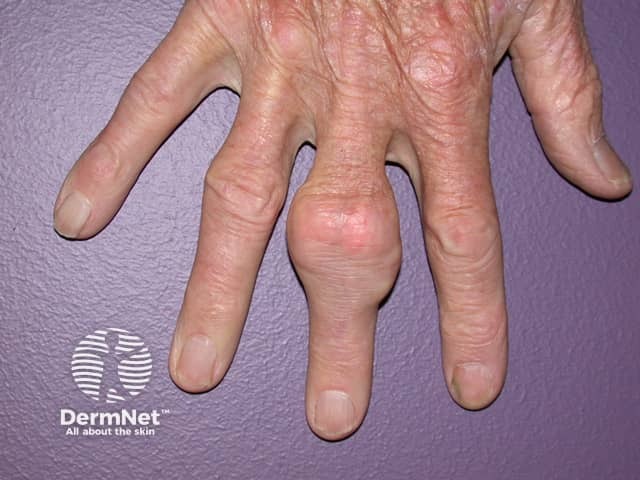
Gouty tophi
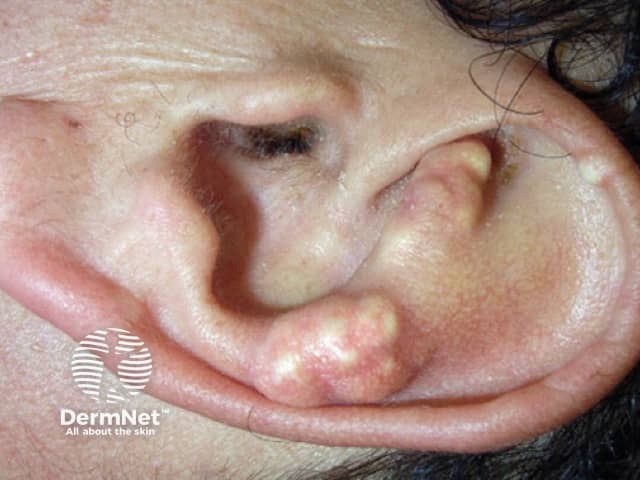
Gouty tophi
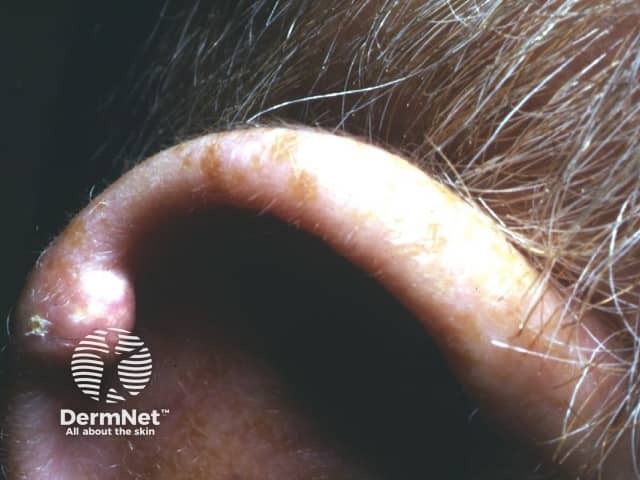
Gouty tophi
More images of gouty tophi ...
The treatment of gout is divided into 3 phases: treatment of the acute attack, uric acid-lowering therapy, and prevention of acute flares.
Options for treatment to relieve the pain of an acute attack of gout include:
The above medicines do not prevent joint damage, tophi, or kidney disease.
Long term management of gout focuses on lowering urate levels, aiming for levels under 0.36 mmol/L, or better still, under 0.30 mmol/L. These medicines can prevent attacks of gouty arthritis and prevent MSU crystals from being deposited in the tissues. Medicines that lower urate levels should not be started during an acute attack of gout; instead they should be started a few weeks after the attack has resolved.
Allopurinol is an effective uric-acid lowering therapy, but it has a number of side effects and interactions with other medicines.
Dermatological side effects of allopurinol range from a mild morbilliform eruption (measles-like rash, which resolves when the drug is discontinued) to Stevens-Johnson syndrome / toxic epidermal necrolysis and drug hypersensitivity syndrome. Drug hypersensitivity syndrome is rare but potentially very severe. It usually occurs within the first 6 weeks of therapy but some cases have been reported up to 12 weeks after starting allopurinol.
The dose of allopurinol should start low at 100mg daily. The dose should be increased every 3-4 weeks, while monitoring blood urate level – aiming for a fall of under 0.04 mmol/L each month and eventual level below 0.36 mmol/L. Some patients may require doses of 600 to 900 mg daily to achieve this. The dose should be lower in those with kidney disease.
Febuxostat (trade name Adenuric®) is a new medication for gout that may be used to reduce urate levels in patients with poor kidney function or intolerant of allopurinol. Phase III clinical trials have reported febuxostat to be more effective than allopurinol at a dose of 300mg. It is funded in New Zealand for treatment–resistant patients or those unsuitable for allopurinol, with Special Authority criteria.
Probenecid is an alternative uric acid lowering medicine with fewer significant side effects than allopurinol.
It is important to drink plenty of fluids while on probenecid, to flush out the uric acid and prevent crystals forming within the kidneys or urinary tract.
The starting dose of probenicid is usually 250 mg twice daily but it may need to be increased to up to 1 g twice daily.
Benzbromarone is a new medication for gout that may be used to reduce urate levels where allopurinol and/or probenecid are contraindicated, not tolerated, or are ineffective. Liver function must be monitored on benzbromarone, as it is reported to cause hepatic toxicity.
Acute flares of gout can be precipitated by the sudden reduction in blood urate that occurs when uric acid lowering medicines are started. For this reason it is important to take a low (preventative) dose of a NSAID or colchicine to reduce the likelihood of a flare developing. In patients unable to take either of these medicines, an oral corticosteroid can be considered. Patients who have only occasional attacks of gout, may only need to take these medicines for 2-3 weeks. Whereas patients with multiple tophi may need to continue treatment for months.
Although lifestyle changes rarely result in adequate reduction in plasma urate without medication, the following are recommended.