What is granuloma inguinale?
Granuloma inguinale is a sexually transmitted infection (STI) caused by the bacteria previously classified as Calymmatobacterium granulomatosis and now reclassified as Klebsiella granulomatis.
It is also called donovanosis after ‘Donovan bodies’, which are cellular components that are seen when scrapings from the genital skin lesions are viewed under a microscope.
How common is granuloma inguinale?
Granuloma inguinale is most commonly found in tropical or subtropical areas such as Papua New Guinea, Southern India, Southern Africa, the Caribbean and South America. In Australia, it is largely confined to Aboriginal and Torres Strait Islander population in the remote northern region. A successful elimination program in Australia targeting this population was started in the mid-1990s. In countries where it is less frequently seen, cases are most probably related to foreign travel. Granuloma inguinale is extremely rare in New Zealand.
Who is at risk of granuloma inguinale?
Sexually active people are at risk of getting granuloma inguinale. The peak incidence is between 20 and 40 years of age. Vertical transmission during childbirth can also occur from contact with the bacteria in the genital tract. A small minority of people (mainly children) may be infected from direct skin-to-skin contact. Klebsiella granulomatis is of low pathogenicity and it may require repeated exposure to develop skin lesions.
What are the signs and symptoms of granuloma inguinale?
The time from exposure to the bacteria to the development of signs and symptoms of granuloma inguinale has not been well defined. The reported median is 50 days, but it can vary from a few days to up to a year.
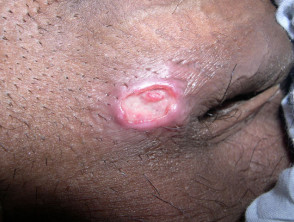
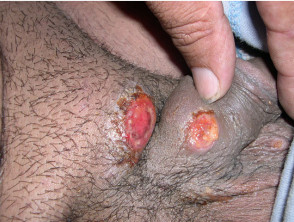
The initial lesion is usually a firm papule or subcutaneous nodule at the site of contact, that later ulcerates. The areas most commonly affected are the penis (corona, glans and prepuce), the vulva (labia minora and fourchette) and anal area (which is more common in men).
Ulcerovegetative type
The ulcerovegetative type of granuloma inguinale is the most common clinical presentation.
- Single or multiple painless firm papules and nodules (granulomas) arise at the site of contact.
- They then erode into soft, painless ulcers that bleed easily.
- In skin folds, they have a linear ‘knife cut’ appearance.
- The ulcer base consists of beefy red granulation tissue and the margins are sharp with rolled or heaped-up borders.
Without treatment, these ulcers continue to enlarge.
Nodular type
The nodular type of granuloma inguinale is less common than the ulcerovegetative type and consists of a mixture of papules and nodules that are soft and red, also with some granulation tissue.
Hypertrophic (verrucous) type
The hypertrophic type of granuloma inguinale consists of large vegetating masses, which has been described as a ‘walnut' appearance.
Necrotic type
The necrotic type of granuloma inguinale consists of a deep foul-smelling ulcer.
Cicatricial (sclerotic) type
Cicatricial granuloma inguinale consists of extensive plaques of scar tissue.
What are the complications of granuloma inguinale?
The infection can spread to the inguinal region where it can cause swelling and ulceration. This is called pseudobubo. Complications of chronic granuloma inguinale include bleeding, secondary infection, swelling from lymphoedema, and significant scarring causing destruction of the genital architecture.
Granuloma inguinale
Credit. Images supplied by Dr Shahbaz A. Janjua
How is granuloma inguinale diagnosed?
Due to the variation in presentation and significant overlap with other genital ulcers, granuloma inguinale can be difficult to diagnose clinically.
In the early stages, it may be difficult to differentiate it from chancroid. In the later stages, it may look like lymphogranuloma venereum. It may also be confused with other conditions, such as penile or vulvar cancer, genital herpes or syphilis.
Laboratory diagnosis is made by direct microscopy of Giemsa-stained crushed tissue smear looking for characteristics Donovan bodies or by histological examination of a tissue biopsy. Culture is very difficult. Nucleic acid amplification tests are not routinely available and serology testing is not useful.
What is the treatment for granuloma inguinale?
Granuloma inguinale is treated with antibiotics. In settings where this infection is very rare, it is recommended that management involve a sexual health or infectious diseases specialist.
The suggested preferred antibiotic is 1 g of weekly azithromycin for 3 or more weeks. Other treatment options include trimethoprim and sulfamethoxazole, doxycycline, erythromycin, with parenteral gentamicin as a treatment adjunct. Treatment should be continued for a minimum of 3 weeks or until the lesions heal completely; provided there is an adequate clinical response.
Sexual activity should not take place until all lesions are completely healed. A follow-up examination is necessary to ensure a complete recovery. Sexual contacts should be notified and undergo clinical examination for possible lesions. Antibiotic prophylaxis should be considered for a baby born to an infected mother with genital lesions.
A full sexual health screen should be done, in particular tests for genital herpes, syphilis and human immunodeficiency virus (HIV). Lesions that bleed easily increase the risk of HIV transmission and multiple infections can be present.
Can granuloma inguinale be prevented?
Like other sexually transmitted infections, the risk of acquiring this infection is reduced by safe-sex practices including limiting the number of sexual partners, avoiding sexual contact with individuals from a high-risk population, and using condoms.
If you think you are infected, stop all sexual contact and see your usual doctor or a specialist clinician at a sexual health clinic immediately.