Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Steven Lamb, Dermatology Registrar, Department of Dermatology, Waikato Hospital, Hamilton, New Zealand, 1998. Updated by Vanessa Ngan, Staff Writer, 1 February 2014. Updated by Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, October 2015.
Introduction
Demographics
More information
Clinical features
Complications
Diagnosis
Treatment
Why treatment fails
Prevention
Head lice are small, wingless insects that infest the human scalp. They are the most common of the 3 human lice species.
Head lice infestation is also called pediculosis capitis.

Louse

Louse

Head lice eggs
Head lice affect people of all ages and walks of life, all over the world. They are a very common problem in children 4–14 years of age.
Risk factors for infestation include:
Head lice can't jump or fly but spread by crawling along hair shafts by head to head contact.
The head louse, Pediculus humanus capitis, is an ectoparasite that feeds on human blood. It is 2–3 mm in length and has a flattened, elongated, grey coloured body that becomes reddish after feeding. The louse clings to the hair shaft by its 6 claws and rapidly moves from hair to hair.
Lice inject anticoagulant saliva into a person's scalp to suck up the blood up to five times a day. They die within one to two days away from the scalp if they are unable to feed.
After mating, the female louse attaches her eggs to the hair shaft close to the scalp in cool climates, and further down the shaft in warmer climates. The female louse can lay 50–100 eggs at a rate of 3–6 per day. The new egg cases are brown and hard to see. They are carried away from the scalp as the hair grows.
The eggs hatch after about 8 days. The empty egg case appears white and is more easily seen (the nit).
The louse nymph reaches full maturity around 10 days after hatching and the cycle begins again. An adult louse survives on the scalp for about one month, and away from the scalp for up to 48 hours.
Head lice usually cause an itch and irritation in the scalp. This can take several weeks to develop after the initial infestation.
Occasionally the eyelashes can become infested, although this is more frequently due to a different insect, the pubic louse.
Scratching can cause crusting and scale on the scalp. Hair pulling can lead to small areas of hair loss.
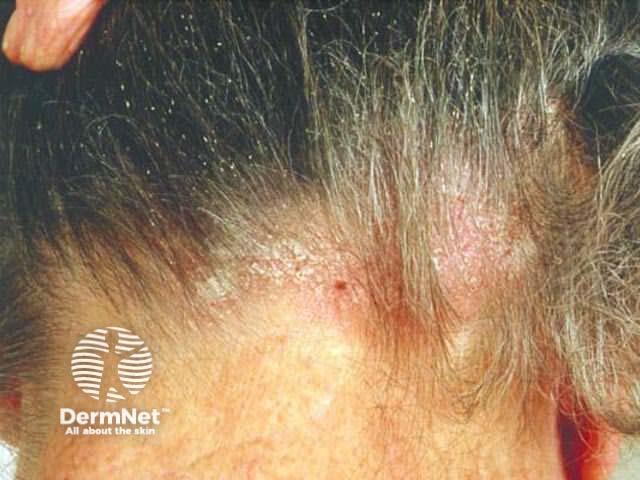
Nits and dermatitis
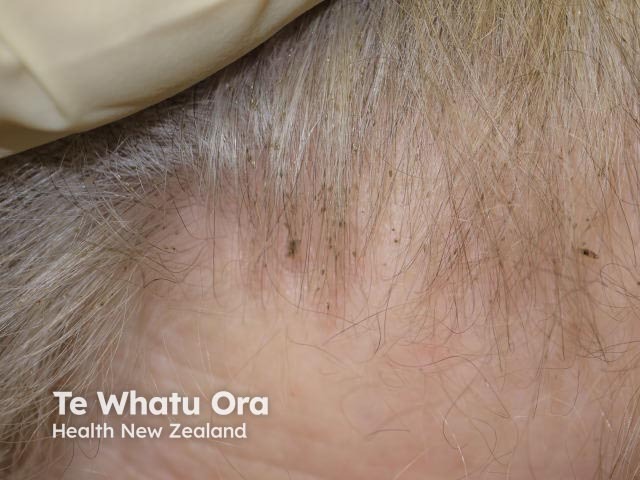
Nits and flaky skin
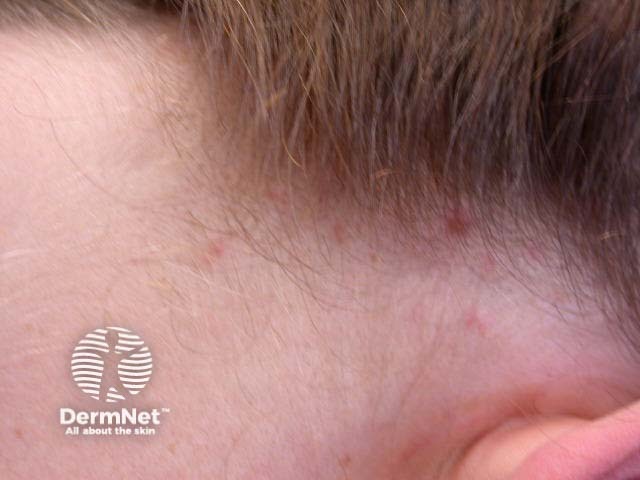
Nits and bites
The head lice do not carry any other infectious disease. A heavy infestation can lead to:
It is important to identify the lice (or nits) to make a correct diagnosis. The lice can be hard to detect, and there are usually only 10–20 adult lice in each colony.
It is easier to identify (and remove) live lice by wet combing using a lice comb, compared to visual inspection alone.
For information on trichoscopic findings of head lice (dermoscopy of the scalp and hair), see Trichoscopy of scalp infestations.
Treatment of head lice usually consists of at least 2 applications of an insecticide and/or physical methods. Note:
The main suffocating agent used to kill the adult and nymph head lice is 4% dimethicone (also spelt dimeticone). Lice are unlikely to develop resistance due to the mechanism of action, and the product is safe and well tolerated. Cure rates are reported to be 69–92% after two applications one week apart.
The most commonly used topical insecticides for head lice is malathion, but resistance has been reported and cure rates are reported to be as low as 33%. Resistance to permethrin, phenothrin and other pyrethrins has increased to the degree that they are no longer recommended in the UK. Other, more expensive, topical options include:
Lotions, liquids or cream are preferred to shampoo (which is too weak to be reliable). They are applied directly to the scalp. It is important to follow the manufacturer’s advice on how long to use it and how often to repeat it due to potential toxicity.
Physical methods of removing nits and lice are used in conjunction with insecticide treatments and may be required daily for several weeks.
Expect nit removal to take at least half an hour. Repeat daily until no lice are found on 3 consecutive occasions.
Electrical combs designed to 'zap' lice on the hair shaft are probably not effective.
The effectiveness of these treatments has not been extensively studied.
These include:
Failure to eradicate lice is a common and frustrating problem. It can be due to:
It is difficult to prevent head lice infestation in children. Discourage children from sharing or using another child’s hat, comb, or brush.
Community-wide or school-based education programmes informing parents of methods to eradicate lice, and community health teams in schools, are the most effective ways in keeping infestation rates down.