What skin changes occur due to cold?
Acrocyanosis
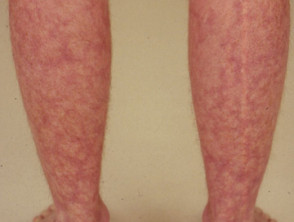
Acrocyanosis is the name given to mottled cold peripheries with cyanosis (blue discolouration) or erythema (reddened skin). It predisposes to chilblains.
Chilblains (pernio)
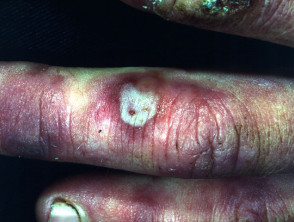
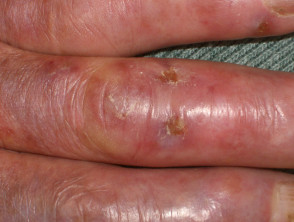
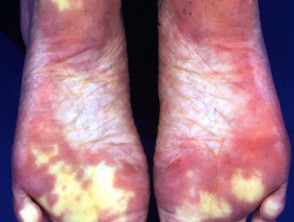
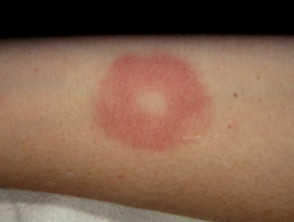
Chilblains arise because of a localised cold injury in exposed areas (most often fingers, toes, ears). They present with erythema, cyanosis, oedema, blisters and ulceration. The lesions usually heal within several weeks as long as there is no further exposure to significant cold. Severe pernio may be the presenting sign of connective tissue disease, especially systemic lupus erythematosus (chilblain lupus) or systemic sclerosis. However, they are also an occupational hazard for dairy farmers, fishermen and other outdoor workers.
Severe cold injury can damage the small bones in the digits, leading to microgeodic disease, swelling and sometimes, bone fracture.
Prevention of chilblains requires keeping the digits and ears warm and dry. A vasodilator medicine such as oral nifedipine may be helpful.
Chilblains
Raynaud phenomenon
The term Raynaud disease refers to primary Raynaud phenomenon. Secondary Raynaud phenomenon is associated with many underlying diseases, especially systemic sclerosis.
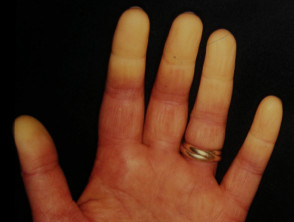
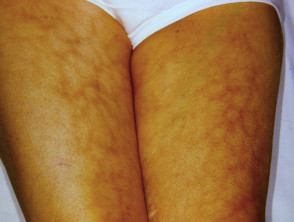
Characteristically, painful attacks follow exposure of the digits to cold. They become white then, in turn, cyanosed and erythematous before returning to a normal colour.
Raynaud phenomenon
Frostbite
Frostbite is due to severe cold injury (temperatures below freezing). Early signs are blanching and numbness.
Treat areas exposed to severe cold by rapid re-warming in a water bath at 40° (providing no risk of further re-freezing). Late sequelae include pain, numbness, cold sensation, hyperhidrosis, dystrophic nails, fibrosis, osteoporosis, and cold intolerance.
Cryoglobulinaemia
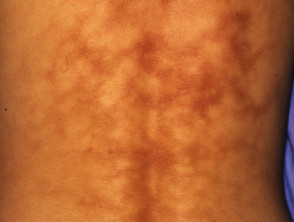
Cryoglobulinaemia is a condition in which proteins are circulating in the bloodstream that may solidify in cold conditions. Cold-precipitable proteins are deposited in cool areas (ears, toes, fingers). Cryoglobulinaemia may present as livedo reticularis or superficial infarction or cutaneous vasculitis.
Livedo reticularis
Cold urticaria
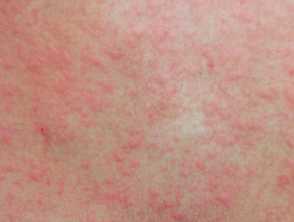
Cold urticaria is a rare type of chronic inducible urticaria that arises during re-warming after cold exposure. It usually affects children and young adults.
Weals may affect any site, most often the face and exposed places. The weals persist for up to two hours. Cold urticaria may result in anaphylactoid symptoms, for example when swimming in cold water.
Urticaria induced by ice
What skin changes occur due to heat?
Erythema ab igne
Erythema ab igne is due to local heat such as a hot water bottle or sitting close to a fire. It presents as erythema in a vascular distribution and is often followed by postinflammatory pigmentation. No treatment is effective, but the appearance improves with time.
Erythema ab igne
Erythromelalgia
Erythromelalgia results in burning pain when feet or hands are warm. Affected areas are erythematous or cyanotic. Some cases are associated with polycythaemia, thrombocythaemia or lupus erythematosus. In these secondary cases, symptoms may respond to low-dose aspirin.
Heat urticaria
Heat urticaria is a local wealing reaction to heat and is rare.
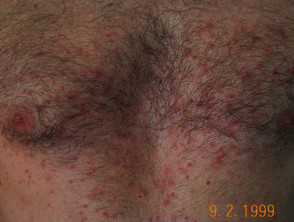
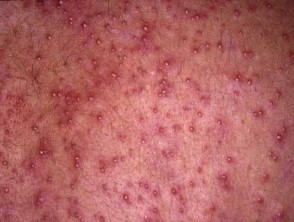
Cholinergic urticaria
Cholinergic urticaria is a type of chronic inducible urticaria caused by heat, emotional stress and exercise. The mechanism is uncertain as wealing may occur without sweating. It usually presents with numerous pruritic 2–3 mm weals surrounded by a red flare, which persist for 15–30 minutes and are at least sometimes associated with exercise. Treatment may include oral antihistamines, phototherapy, propranolol or scopolamine with variable efficacy.
Cholinergic urticaria
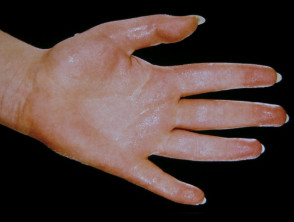
Hyperhidrosis
Excessive eccrine secretion or hyperhidrosis may be generalised or localised (most often to hands, feet, axillae and face). Most cases present in adolescence or young adult life and appear to be due to idiopathic hypothalamic stimuli. Hyperhidrosis is rarely due to systemic disorders such as hyperthyroidism or hypothalamic disease when it is more likely to present later in adult life.
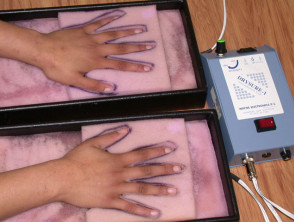
Hyperhidrosis is aggravated by thermal, emotional or gustatory stimulae. It may result in bromhidrosis and occupational difficulties. All patients should use medical grade antiperspirant lotions, which contain aluminium salts. Other treatments include iontophoresis, oral propantheline, propranolol, intradermal botulinum toxin, axillary liposuction or excision of the affected skin, or in severe cases, sympathectomy.
Hyperhidrosis
Miliaria
Miliaria refers to sweat rash (prickly heat) due to obstructed sweat glands and perhaps localised hyperproliferation of specific commensal microorganisms such as strains of Staphylococcus epidermidis. It presents with non-follicular superficial papules, vesicles or pustules mainly arising on the trunk. Treatment requires cooling; calamine lotion may be soothing.
Miliaria