What is IgG?
IgG or immunoglobulin G is the most common form of antibody, an essential group of proteins in the humoral or circulating immune system.
IgG is composed of 4 peptide chains: 2 heavy chains and two light chains. There are four subclasses of IgG.
What is IgG subclass deficiency?
IgG deficiency is an inherited condition in which there is a normal total level of IgG but low levels of at least one of the IgG subclasses. Each of these subclasses has a slightly different immune function:
- IgG-1 forms antibodies against protein antigens like tetanus
- IgG-2 forms antibodies against antigens like pneumococcal polysaccharides
- IgG-3 forms antibodies to antigens similar to IgG-1
- IgG-4 forms antibodies to extracellular parasites
In patients with IgG subclass deficiency, other components of the immune system function normally.
What causes IgG subclass deficiency?
The pattern of inheritance connected with IgG subclass deficiency is not known. IgG subclass deficiency can affect both males and females. Partial gene deletion may prove to be a cause of IgG subclass deficiency (and is a known cause of selective IgA deficiency).
What are the signs and symptoms of IgG subclass deficiency?
Patients with IgG subclass deficiency may present with:
- Frequent or chronic infections, especially from Streptococcus, Haemophilus and Branhamella catarrhalis species
- Common diseases such as otitis media, sinusitis, pneumonia, and bronchitis
- Recurrent bouts of sepsis and meningitis
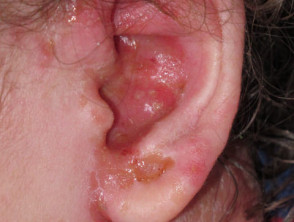
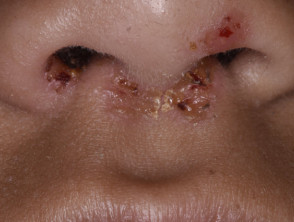
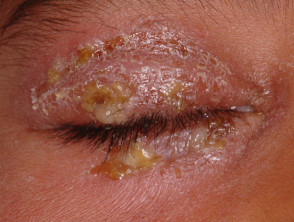
- Asthma and atopic dermatitis.
Infected eczema
How is IgG subclass deficiency diagnosed?
Diagnosis of IgG subclass deficiency is made in a patient with a history of chronic bacterial infections. IgG subclasses can be measured, but the results of this testing are not always conclusive. Levels should be tested again in several months to determine if the values are truly abnormal.
Diagnosis should also take into account the patient’s overall health, presenting symptoms, and response to vaccines.
How is IgG subclass deficiency treated?
IgG subclass deficiency is treated with:
- Antibiotics for infection control
- A pneumococcal vaccine to strengthen the immune response against pneumococcal infection
- IgG therapy, if more conservative measures are not successful.