Introduction
Intralymphatic histiocytosis manifests as quite non-descript erythematous patches or plaques. Autoimmune disease (eg, rheumatoid arthritis), joint replacements, and malignancy, rosacea appear to be aetiologic factors.
Histology of intralymphatic histiocytosis
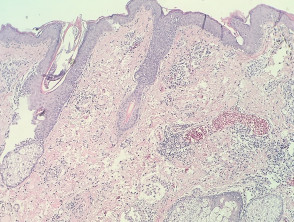
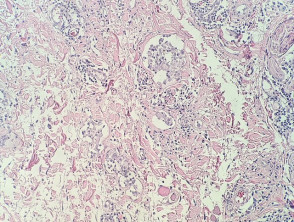
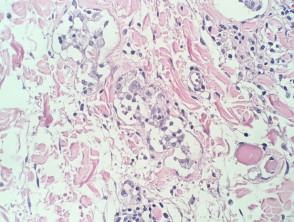
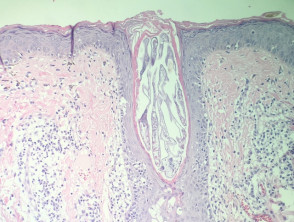
In intralymphatic histiocytosis, the histopathology shows dilated lymphatic spaces stuffed with histiocytes and associated lymphocytes (figures 1,2,3). There is often oedema of the surrounding dermis. The overlying epidermis is uninvolved. In cases occurring around the eyes, it is common to find Demodex species in follicular structures (figure 4).
Intralymphatic histiocytosis pathology
Special studies for intralymphatic histiocytosis
Immunohistochemical studies for lymphatics (eg, D2–40) highlight the lymphatic structures. Histiocyte markers (eg, CD68, CD143) highlight the histiocytes.
The differential diagnosis for intralymphatic histiocytosis
- Malignancy — intravascular carcinoma or melanoma needs to be excluded. Carcinoma or melanoma will generally stain positively with cytokeratins and melanocytic markers (eg, Sox-10) respectively
- Melkersson–Rosenthal syndrome — this disease often shows intralymphatic histiocytes but also shows extravascular granulomas.