What is intralymphatic histiocytosis?
Intralymphatic histiocytosis is a rare benign chronic skin condition most commonly associated with rheumatoid arthritis, orthopaedic metal implants, or cancer surgery. It was first described in 1994 as intravascular histiocytosis.
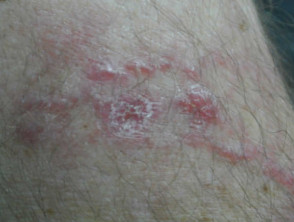
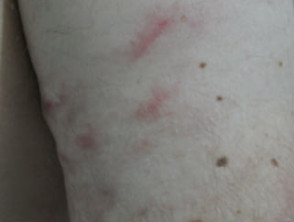
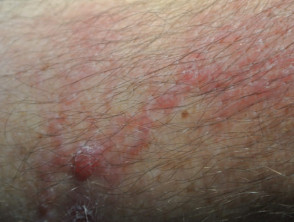
Intralymphatic histiocytosis
What causes intralymphatic histiocytosis?
The exact cause of intralymphatic histiocytosis is not known. It was initially thought to be a reactive angiomatosis, such as an early form of reactive angioendotheliosis (a proliferation of vascular endothelial cells). More recent theories about its cause include it resulting from lymphatic disruption due to inflammation causing lymphatic vessels to dilate with pooling of lymph and reduced clearance of antigens, leading to an accumulation or proliferation of macrophages (histiocytes). A role for tumour necrosis factor alpha in the causation of intralymphatic histiocytosis has been suggested after two patients with rheumatoid arthritis were treated with infliximab, and the skin lesions resolved.
Classification of intralymphatic histiocytosis
Intralymphatic histiocytosis has been classified into primary and secondary intralymphatic histiocytosis. Primary (or idiopathic) intralymphatic histiocytosis is where the patient has been otherwise well, and no associated trigger can be identified. This is much less common than the secondary form of intralymphatic histiocytosis where there is an associated condition, most commonly inflammatory or surgical.
What conditions are associated with intralymphatic histiocytosis?
The most common condition reported in association with intralymphatic histiocytosis has been rheumatoid arthritis, which has affected patients in over one-third of reported cases. Osteoarthritis has also been reported with intralymphatic histiocytosis, but less commonly.
- Twenty-five per cent of cases have been reported in association with orthopaedic metal implants from joint replacements or repairs after fractures.
- Cancer surgery, especially mastectomy for breast cancer, ranks third in the association with intralymphatic histiocytosis and is reported in 10% of patients with intralymphatic histiocytosis.
Other conditions that have been reported once or twice in association with intralymphatic histiocytosis include:
- Crohn disease
- Chronic tonsillitis
- Vulval necrosis
- Dermatomyositis
- Monoclonal gammopathy (the accumulation of abnormal proteins in the blood)
- Melanoma
- Merkel cell carcinoma.
Who gets intralymphatic histiocytosis?
Intralymphatic histiocytosis most commonly affects older adult women. In reported cases, it affects men and women as a ratio of 3:5, with an age range of 17–87 years, with a mean age of 65 years.
What are the symptoms and signs of intralymphatic histiocytosis?
Typically, intralymphatic histiocytosis presents as a rash on one limb, overlying or adjacent to the affected joint or scar. It does not usually cause any symptoms. The colour of the rash ranges from red through to brown and purple. The rash can be macular (completely flat) or may form slightly raised plaques. Papules, nodules, or vesicles may form, and a linear or livedo pattern is sometimes seen.
The arm is the most common site (reported in approximately 50% of cases), with the leg being the second most common site. It has also been reported on the trunk, especially over a mastectomy scar, face, oral mucosa, and the vulva.
There does not appear to be any correlation between the activity of rheumatoid arthritis and the skin rash, but the rash does closely relate to an involved joint.
There is no pitting oedema or other signs associated with lymphoedema.
How is intralymphatic histiocytosis diagnosed?
A biopsy is required to make the diagnosis. The histology of intralymphatic histiocytosis is diagnostic and requires the presence of dilated lymphatic vessels in the dermis, with CD68-positive histiocytes within the lumen. The cells forming the lymphatic vessel wall and within the lumen are normal in appearance. Sometimes, there may also be perivascular or granulomatous dermal inflammation of small lymphocytes, histiocytes, and plasma cells.
What is the treatment of intralymphatic histiocytosis?
Intralymphatic histiocytosis is usually resistant to all treatments that have been tried, including the use of topical, intralesional, and oral steroids. Temporary improvement may be seen but the skin disorder rapidly relapses.
The treatment of the associated condition may result in the clearance of intralymphatic histiocytosis, and this has been reported after a joint replacement for an arthritic knee, antibiotics and tonsillectomy for tonsillitis, and antibiotics and surgical debridement of vulval necrosis.
Infliximab has been reported to have cleared intralymphatic histiocytosis in two patients with rheumatoid arthritis. Methotrexate seemed to slowly clear the skin in one reported case.