Introduction
Brodalumab (Siliq™; Valeant Pharmaceuticals, New Jersey, USA) is a human monoclonal IgG2 antibody that selectively binds to human interleukin-17 (IL-17) receptor and inhibits its interactions with a number of cytokines of the IL–17 family. Brodalumab targets the receptor for IL–17, which is a cytokine or messenger protein involved in inflammation resulting in psoriasis.
In February 2017, brodalumab received US Food and Drug Administration (FDA) approval to treat psoriasis in adult patients who have not responded to other treatments. In May 2017, the European Medicines Agency's Committee for Medicinal Products for Human Use recommended the granting of a marketing authorisation for brodalumab for the treatment of moderate–to–severe plaque psoriasis in adults who are candidates for systemic therapy (treatment using substances that travel through the bloodstream, after being taken by mouth or injected) or phototherapy (ultraviolet radiation treatment).
Chronic plaque psoriasis
Major trials supporting clinical efficacy of brodalumab
The approval of brodalumab was based on three phase 3 trials:
- AMAGINE–1 evaluated the efficacy, safety, and the withdrawal and retreatment effect of brodalumab compared with placebo.
- AMAGINE–2 and AMAGINE–3 were 12–week induction trials followed by re-randomisation at Week 12 and evaluated the efficacy and safety of induction and maintenance with brodalumab compared with ustekinumab and placebo.
AMAGINE–1
- AMAGINE–1 was a phase 3, randomised, double-blind, placebo-controlled trial including a 12-week induction phase followed by a withdrawal/retreatment phase from Weeks 12 through to 52.
- Using a 1:1:1 randomisation, 661 patients were randomised to biweekly injections of brodalumab 210 mg (n = 222), brodalumab 140 mg (n = 219), and placebo (n = 220) for 12 weeks.
- At week 12, patients achieving static Physician's Global Assessment score (sPGA) of 0 or 1 entered the withdrawal/retreatment phase and were re-randomised 1:1 to receive brodalumab 210mg every 2 weeks (n = 83) or placebo (n = 84) or brodalumab 140mg every 2 weeks (n = 57) or placebo (n = 59).
- All other patients with sPGA ≥ 2 received brodalumab 210 mg every 2 weeks (n = 208).
- All patients were followed up to Week 52.
- At Week 16 of the withdrawal/retreatment phase, patients who experienced return of disease (sPGA ≥ 3) were re-treated with their induction-phase doses of brodalumab.
- After a further 12 weeks of retreatment, those patients with inadequate response (sPGA ≥ 3), qualified for rescue treatment and received open-label brodalumab 210 mg every 2 weeks.
Results — Week 12 (AMAGINE–1)
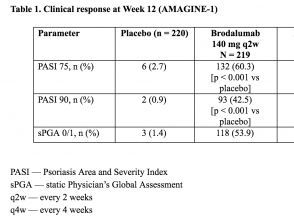
- At Week 12, the co–primary endpoint of a 75% reduction in the Psoriasis Area and Severity Index score (PASI 75) was achieved by 83% (95% confidence interval [CI] 78–88), 60% (95% CI: 54–67) and 3% (95% CI: 1–6) of patients randomised to brodalumab 210 mg every 2 weeks, brodalumab 140 mg every 2 weeks and placebo, respectively.
- The corresponding percentages for sPGA success were 76% (95% CI: 70–81), 54% (95% CI 47–61) and 1% (95% CI: 0–4) (p < 0.001) for brodalumab 210 mg every 2 weeks, brodalumab 140 mg every 2 weeks and placebo, respectively.
- The median times to both PASI 75 response and sPGA success were 4 weeks and 6 weeks in patients randomised to brodalumab 210 mg and 140 mg, respectively.
- Hospital Anxiety and Depression Scale scores were analysed at Week 12. Statistically significant decreases (p < 0.001) in mean depression were observed for brodalumab 210 mg (5.5% to 3.4%) and 140 mg (5.2% to 3.5%) doses from baseline at Week 12. The placebo arm was unchanged (5.3% at baseline and 5.5% at Week 12).
Results — withdrawal/retreatment phase (AMAGINE–1)
- At Week 52, the percentages of patients with sPGA success were 83% and 0% for brodalumab 210 mg and placebo groups, respectively (p < 0.001 vs placebo).
- At Week 52, the percentages of patients with sPGA success were 70% and 5% for the re-randomised brodalumab 140 mg and placebo groups, respectively (p < 0.001 vs placebo).
- Patients with return of disease (sPGA ≥ 3 at Week 16) during the withdrawal phase qualified for retreatment with their induction dose of brodalumab.
- Among these patients, 97% receiving brodalumab 210 mg and 84% receiving brodalumab 140 mg achieved a sPGA score of 0 or 1 after 12 weeks of retreatment.
- The median time to recapture sPGA success for both brodalumab 210 mg and 140 mg was 4 weeks.
Table 1. Clinical response at Week 12 (AMAGINE–1)
Adverse events – Week 12 (AMAGINE–1)
The most frequent adverse events (≥ 5% in any group) at Week 12 were:
- Nasopharyngitis
- Upper respiratory tract infection
- Headache.
Table 2. Common adverse events at Week 12 (AMAGINE-1)
There were four fatal adverse events through Week 52: these included:
- A sudden death in a patient receiving brodalumab 210 mg (induction and retreatment/withdrawal phase)
- An intentional illicit drug overdose considered by the coroner to be suicide in a patient receiving placebo (induction phase) and brodalumab 210 mg (withdrawal phase)
- An oesophageal variceal haemorrhage in a patient with a history of cirrhosis receiving brodalumab 210 mg (induction and withdrawal/retreatment phases).
- A cerebrovascular accident in a patient receiving brodalumab 210 mg (induction phase), placebo (withdrawal phase) and brodalumab 210 mg (retreatment phase).
AMAGINE–2 and AMAGINE–3
- AMAGINE–2 and AMAGINE–3, were two large, parallel group, double-blind, active comparator controlled, multinational phase 3 trials involving a 12-week induction phase and 40-week maintenance phase.
- During the 12-week induction phase, patients were randomised utilising a 2:2:1:1 ratio to receive brodalumab 210 mg or 140 mg every 2 weeks, ustekinumab (45 mg for subjects < 100 kg in weight and 90 mg for subjects > 100 kg) every 4 weeks, or placebo.
Induction phase results – Week 12 (AMAGINE–2 and AMAGINE–3)
- The primary aims were to evaluate the superiority of brodalumab over placebo at Week 12 with respect to PASI 75 response and a sPGA score of 0 or 1 (clear or almost clear skin), and the superiority of brodalumab over ustekinumab at Week 12 with respect to a 100% reduction in PASI 100.
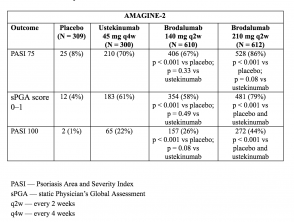
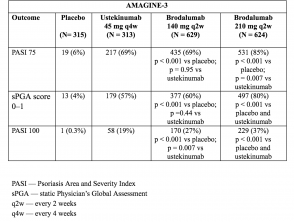
- At Week 12, the PASI 75 response rates were higher with brodalumab 210 mg and 140 mg than with placebo (86% and 67% respectively, vs. 8% [AMAGINE-2] and 85% and 69% respectively, vs 6% [AMAGINE–3]; p < 0.001).
- The median time to PASI 75 response was 4 weeks for brodalumab 210 mg versus approximately 2 months for ustekinumab.
- The rates for sPGA scores of 0 or 1 were also higher with brodalumab 210mg versus ustekinumab (p < 0.001).
- The Week 12 PASI 100 response rates were significantly higher with 210 mg of brodalumab than with ustekinumab (44% vs. 22% [AMAGINE–2] and 37% vs 19% [AMAGINE–3]; p < 0.001).
Tables 3 & 4. Clinical response at week 12 — AMAGINE–2 and AMAGINE–3
Results maintenance phase — AMAGINE–2 and AMAGINE–3
- At Week 12, patients who were originally randomly assigned to receive brodalumab underwent repeat randomisation, in a 2:2:2:1 ratio, to one of four maintenance regimens: brodalumab 210 mg every 2 weeks, 140 mg every 2 weeks, 140 mg every 4 weeks, or 140 mg every 8 weeks, stratified according to Week 12 body weight (≤ 100 kg or > 100 kg), induction regimen, and Week 12 response (sPGA score, 0 or ≥1).
- Patients who were originally randomly assigned to receive placebo were switched to brodalumab 210 mg every 2 weeks and patients who were originally randomly assigned to receive ustekinumab continued to receive ustekinumab every 12 weeks until Week 52.
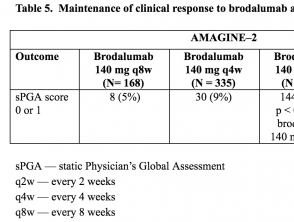
- At Week 52, the proportion of patients with an sPGA score of 0 or 1 was significantly higher among those who received brodalumab 210 mg or 140 mg every 2 weeks than those who received the other brodalumab maintenance regimens (p < 0.001).
- The PASI response-over-time curves for patients who received brodalumab 210 mg throughout the study or ustekinumab throughout the study showed that response rates increased through Week 12 and stabilised during Weeks 16 to 52.
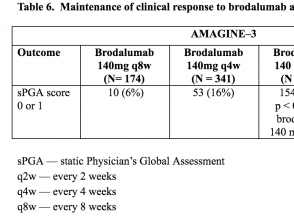
Tables 5 & 6. Maintenance of clinical response to brodalumab at Week 52 — AMAGINE–2 and AMAGINE–3
Adverse events — AMAGINE–2 and AMAGINE–3
- In the induction phase, the most common adverse events were nasopharyngitis, upper respiratory tract infection, headache, and arthralgia.
- With the exception of upper respiratory tract infection, these events were more frequent with brodalumab than with placebo or ustekinumab in the AMAGINE–2 study.
- Arthralgia was more frequent with brodalumab than placebo or ustekinumab in the AMAGINE–3 study.
- The rates of serious adverse events per 100 patient-years through week 52 were 8.3 with brodalumab and 13.0 with ustekinumab in the AMAGINE–2 study and 7.9 and 4.0, respectively, in the AMAGINE–3 study.
- There were no clinically apparent differences in the types of serious adverse events among the study groups.
- Candida infections occurred more frequently with brodalumab than with ustekinumab or placebo during the induction phase; all the infections were graded as mild or moderate, and none were systemic. This trend continued through Week 52.
- The rates of serious infectious episodes per 100 patient-years of exposure to brodalumab through Week 52 were 1.0 in the AMAGINE–2 study and 1.3 in the AMAGINE–3 study; the corresponding rates with ustekinumab were 0.8 and 1.2.
Brodalumab — future potential
- The IL–17 cytokine pathway plays an important role in psoriasis.
- Three phase 3 studies with brodalumab have validated the important role of the IL–17 receptor in moderate-to-severe psoriasis.
- Brodalumab was shown to have efficacy superior to that of placebo and ustekinumab with respect to PASI 100 response in a comparison of brodalumab 210 mg every 2 weeks with ustekinumab.
- Brodalumab treatment resulted in a rapid reduction of the signs and symptoms of psoriasis.
- The median time to a PASI 75 response was 4 weeks with brodalumab 210 mg every 2 weeks — approximately twice as fast as the median time to a PASI 75 response with ustekinumab.
- Based on efficacy alone, brodalumab and other IL-17 class biologicals could become first-line therapy for moderate to severe plaque psoriasis.
- However, safety considerations in relation to depression and suicidality could hamper the use of brodalumab in favour of the other IL-17 biologicals secukinumab and ixekizumab.
- To provide a full understanding of the safety profile of brodalumab, further clinical trials including large numbers of patients and longer follow-up periods may be necessary.
We suggest you refer to your national drug approval agency such as the Australian Therapeutic Goods Administration (TGA), US Food and Drug Administration (FDA), UK Medicines and Healthcare products regulatory agency (MHRA) / emc, and NZ Medsafe, or a national or state-approved formulary eg, the New Zealand Formulary (NZF) and New Zealand Formulary for Children (NZFC) and the British National Formulary (BNF) and British National Formulary for Children (BNFC).