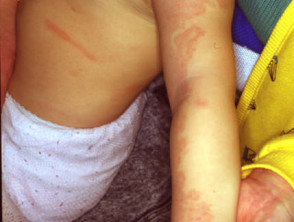
What is Klippel–Trénaunay syndrome?
Klippel–Trénaunay syndrome (KTS) is a rare congenital vascular bone syndrome characterised by a triad of signs; these being:
- Capillary vascular malformation (port-wine stain)
- Venous malformation (eg, varicose veins)
- Limb hypertrophy (usually affecting only one extremity) [1,2].
The syndrome is also called Klippel–Trénaunay–Weber syndrome or angio-osteohypertrophy syndrome, and is an example of haemangiectactic hypertrophy.
Klippel–Trénaunay syndrome
Who gets Klippel–Trénaunay syndrome?
Klippel–Trénaunay syndrome is a rare disease, affecting one in 20,000–40,000 children. It affects both sexes equally and is seen in all races [1]. While it mostly occurs sporadically, some inherited cases have been reported [3].
What causes Klippel–Trénaunay syndrome?
While the exact cause of Klippel–Trénaunay syndrome is not clear, several genes and pathways have been identified in its pathogenesis. Notably, PIK3CA gene mutations have been detected in some cases of Klippel–Trénaunay syndrome. PIK3CA encodes for a subunit of the phosphoinositide 3-kinase enzyme, which is involved in cell proliferation and migration. Gain-of-function mutations can lead to tissue hypertrophy in the bone, soft tissue, and blood vessels [2,4].
The angiogenic gene VG5Q has also been implicated in Klippel–Trénaunay syndrome [5].
What are the clinical features of Klippel–Trénaunay syndrome?
Capillary vascular naevus
One or more capillary vascular malformations (port-wine stains) are present in the overwhelming majority of patients with Klippel-Trénaunay syndrome and this is usually the first noticeable feature [1,2,6]. Commonly, the capillary malformation occurs over the affected hypertrophic limb, but it can also be present at other sites. Rarely, the affected area can blister and bleed [2].
Venous malformations
Varicose veins are a common feature of Klippel–Trénaunay syndrome. They tend to be larger than normal varicose veins and they can be painful. Varicose veins may not be present initially. They usually become noticeable in late infancy, childhood, or adolescence. Deep veins can also be affected, increasing the risk of developing deep vein thrombosis (DVT) [1–3,6].
Persistent embryonic veins can result in a lateral marginal vein or persistent sciatic vein. Bleeding can also occur, which may result in bleeding from the rectum or blood in the urine [6–9].
Malformations in Klippel-Trénaunay syndrome are of slow-flow venous vessels. Fast-flow arteriovenous malformations (clumps of blood vessels that link between arteries and veins) as seen in Parkes Weber syndrome are not present. Bruits (murmurs caused by the narrowing of arteries) tend to be absent on examination [8].
Limb hypertrophy
Limb hypertrophy affects the lower limb in most cases (up to 95%), but hypertrophy can also involve the trunk, and head and neck. Limb enlargement is disproportionate, with the girth of the limb enlarging more than length. Increased girth is due to hypertrophy of the skin and muscles whereas increased limb length is due to bone overgrowth. The average difference in limb length is around 2 cm. The length discrepancy can cause uneven walking, unstable gait, or pain. The child might appear to have scoliosis [1–3,6,9].
Many other malformations have been reported in Klippel-Trénaunay syndrome including lymphangioma circumscriptum and syndactyly (fusion of fingers or toes) or polydactyly (extra fingers or toes).
What are the complications of Klippel–Trénaunay syndrome?
The possible complications of Klippel-Trénaunay syndrome include [1,2]:
- DVT due to malformations of deep veins
- Pulmonary embolism
- Cellulitis
- Lymphoedema
- Internal bleeding.
How is Klippel–Trénaunay syndrome diagnosed?
The diagnosis of Klippel–Trénaunay syndrome is made clinically when two of the three classic signs of port-wine stain, varicose veins, and limb hypertrophy are present. While a diagnosis of Klippel-Trénaunay syndrome can be suspected in a newborn when a port-wine stain is present, the confirmation comes later when other symptoms become more apparent [1–3].
Diagnostic tests that may be required include:
- Magnetic resonance imaging
- Magnetic resonance angiography
- Computed tomography (CT) or CT venography
- Colour duplex ultrasonography
- Ultrasound during pregnancy [3,10].
What is the differential diagnosis for Klippel–Trénaunay syndrome?
Conditions that can be mistaken for Klippel–Trénaunay syndrome include:
- Parkes Weber syndrome — this is characterised by fast-flow arteriovenous malformations and fistulae [8]
- Proteus syndrome — in which there are usually no obvious deformities/features at birth; Proteus syndrome presents later with progressive and more generalised musculoskeletal deformities [11].
- Macrodystrophia lipomatosa — in this form of limb hypertrophy, there is an absence of soft-tissue vascular malformations and a lack of limb-length discrepancy [12].
What is the treatment for Klippel–Trénaunay syndrome?
There is no specific cure for Klippel–Trénaunay syndrome, and generally, most patients can be managed conservatively. Specific treatments and procedures can also be used to reduce symptoms and prevent complications [1,6,10].
Conservative management
Compression stockings are often used to control the symptoms of varicose veins, alleviate pain and swelling, and prevent complications such as bleeding. Dressings, leg elevation, and rest are required for bleeding [1,10].
If the difference in leg lengths is small (< 2 cm), shoe raisers might be recommended to allow the child to walk more easily and prevent compensatory scoliosis. Physiotherapy can also help reduce swelling in the affected limb [1,10].
Ligation and stripping
Ligation of the veins (the surgical tying off of veins) can be used to treat varicose veins in conjunction with vein stripping after confirming an adequate deep venous. system (See DermNet's page of Leg vein therapies). This treatment is not advised in children [1,7,10].
Sclerotherapy
Sclerotherapy refers to the injection of a sclerosing agent into the veins in order to collapse them. It is used to treat complications arising from varicose veins so they are no longer noticeable on the surface of the skin. It can be used in children after detailed scans of the veins in the leg have been made. Several sclerotherapy sessions months apart are usually required [1,7,10].
A variation of this procedure is foam sclerotherapy, which involves injecting a foaming agent (in addition to the sclerosing one) into the veins [7].
Laser therapy
Laser therapy can be used to treat or manage the port-wine stains, although to a limited extent. It is also used to treat small varicose veins and as an adjuvant for sclerotherapy or endovascular ablation (see below) [7,10].
Endovascular thermal ablation
Problematic varicose veins can be closed off by using high-frequency radio waves to create local heat in the affected vein. This is generally associated with fewer risks and faster recovery compared to ligation and stripping [7].
Epiphysiodesis
If the asymmetry between the affected and unaffected legs is predicted to be greater than 2 cm, epiphysiodesis can be performed to slow the growth in the longer leg. This procedure involves prematurely fusing the growth plate of a bone and needs to be timed correctly to match the lengths of the legs by the end of the growth phase [6,7].
Alternatively, the normal leg can also be lengthened surgically to achieve matching size [1].
What is the outcome for Klippel–Trénaunay syndrome?
Patients with Klippel–Trénaunay syndrome tend to do very well. While it is not a life-threatening condition and most patients end up having normal lives, ongoing care is required. This is best provided by a multidisciplinary team of dermatologists, vascular and orthopaedic surgeons, and general surgeons [1,10]. Some people may require counselling to adjust to the cosmetic aspects of the disease [3].