Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2011.
Introduction
Demographics
Clinical features
Causes
Tests
Treatment - lentigo maligna
Treatment - lentigo maligna melanoma
Staging melanoma
Outlook
Lentigo maligna is a precursor to lentigo maligna melanoma, a potentially serious form of skin cancer. Lentigo maligna is also known as Hutchinson melanotic freckle.
Lentigo maligna is an early form of melanoma in which the malignant cells are confined to the tissue of origin, the epidermis, hence it is often reported as ‘in situ’ melanoma. It occurs in sun damaged skin so is generally found on the face or neck, particularly the nose and cheek. It grows slowly in diameter over 5 to 20 years or longer.
Lentigo maligna melanoma is diagnosed when the melanoma cells have invaded into the dermis and deeper layers of skin. Lentigo maligna has a lower rate of transformation to invasive melanoma than the other forms of melanoma in situ (under 5% overall). However, the risk of invasive melanoma is greater in larger lesions, with up to 50% of those with diameter of greater than 4 cm being reported to have an invasive focus.
Management of melanoma is evolving. For up to date recommendations, refer to Australian Cancer Council Clinical practice guidelines for the diagnosis and management of melanoma.
According to New Zealand Cancer Registry data, 2256 invasive melanomas were diagnosed in 2008 and about 10% were pathologically lentigo maligna melanoma. Rates of the precursor, lentigo maligna, are not reported by national cancer registries but it is thought to be the most common variant of melanoma in situ in New Zealand and Australia.
The risk of lentigo maligna relates to sun damage. Thus lentigo maligna is more common in outdoor workers, in older people and in association with solar damage and keratinocyte skin cancer (basal cell carcinoma, squamous cell carcinoma). Although often occurring in those with very fair skin (skin phototype 1 and 2), it may also occur in those who tan quite easily (phototype 3). It is rare in brown or black skin (phototype 4-6).
Lentigo maligna is more common in males than females. The majority of patients with lentigo maligna are older than 40 years, and the peak age of diagnosis is be between 60 and 80 years.
Unlike superficial spreading melanoma, lentigo maligna is not related to the number of melanocytic naevi (moles) or atypical naevi.
Lentigo maligna presents as a slowly growing or changing patch of discoloured skin. At first, it often resembles common freckles or brown marks (lentigines). It becomes more distinctive and atypical in time, often growing to several centimetres over several years or even decades. Like other flat forms of melanoma, it can be recognised by the ABCDE rule: Asymmetry, Border irregularity, Colour variation, large Diameter and Evolving.
The characteristics of lentigo maligna include:
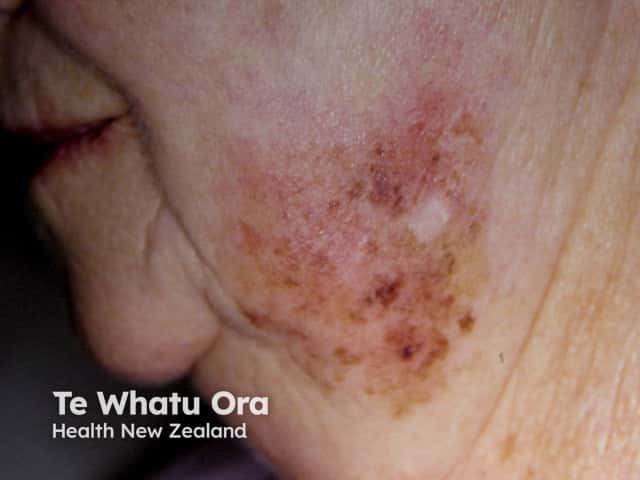
Lentigo maligna
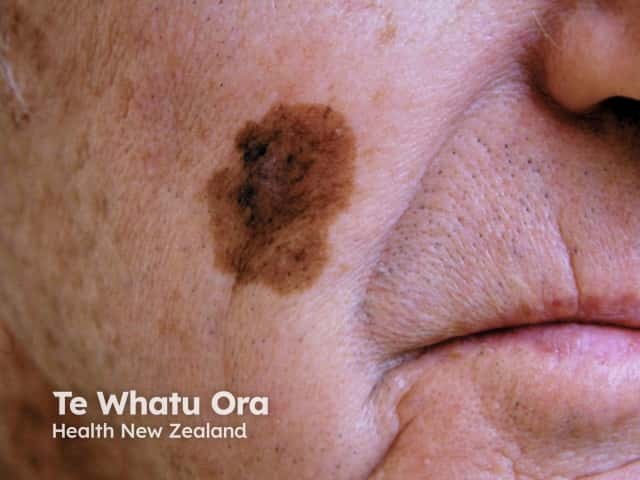
Lentigo maligna
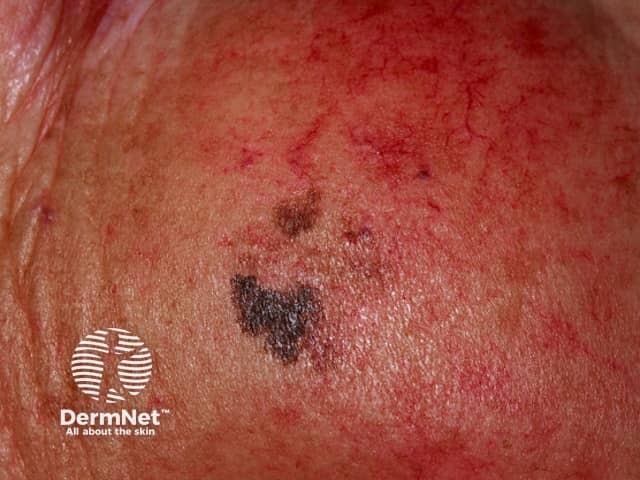
Lentigo maligna
Invasive melanoma is reported to arise within lentigo maligna in 3-10% of cases. It may be difficult to determine whether this has occurred just from the appearance, but the following features are very suspicious.

Lentigo maligna
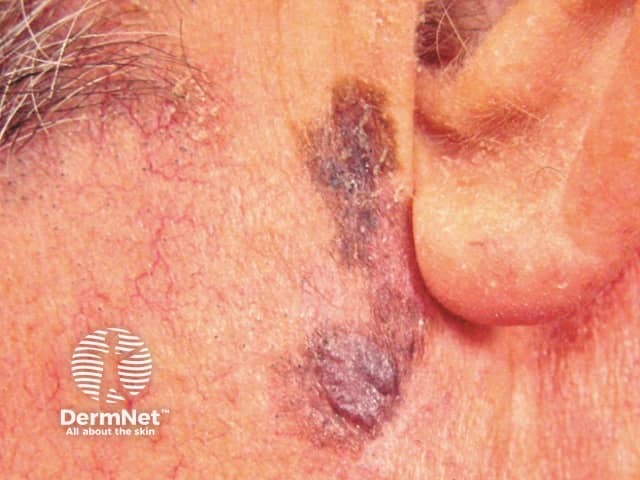
Lentigo maligna
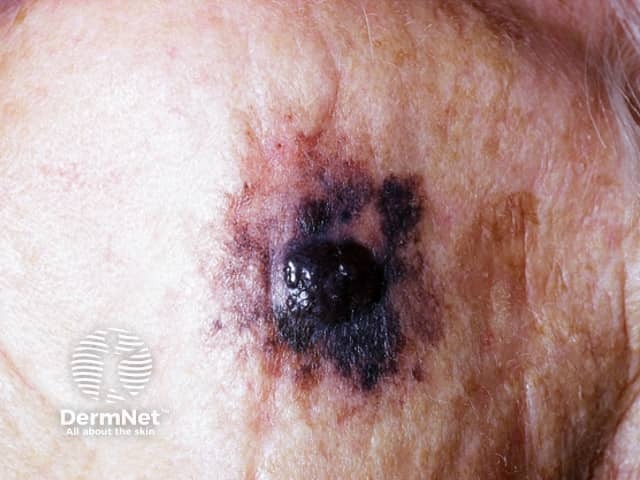
Lentigo maligna
See more images of lentigo maligna melanoma ...
Lentigo maligna is a proliferation of malignant pigment cells (melanocytes) along the basal layer of the epidermis and within the hair follicle. What triggers the cells to become malignant is unknown but genetic mutations may start within primitive stem cells.
Solar damage results in a degree of immune tolerance, allowing abnormal cells to grow unchecked.
It is essential to diagnose lentigo maligna and lentigo maligna melanoma accurately. Clinical diagnosis is aided by dermoscopy and in some centres, by confocal microscopy. New techniques are being evaluated to help identify the margin of lentigo maligna prior to excision biopsy.
Other tests are not necessary in the majority of patients but those with invasive melanoma that is more than 1 mm thick may be advised to have imaging studies, lymph node biopsy and blood tests.
New tests are being developed to determine specific genetic mutations with lentigo maligna melanoma, which may inform future targeted therapy.
Dermoscopy (also called dermatoscopy), or the use of a dermatoscope, by a dermatologist or other doctor trained in its use, can be very helpful in distinguishing lentigo maligna from other types of skin lesion. However, the dermoscopic appearance of early lentigo maligna can be difficult to distinguish from other pigmented lesions, particularly on the face.
Facial pigmented lesions are characterised dermoscopically by pseudonetwork – this is pigmentation arising around prominent facial hair follicles, and several types of skin lesion may appear rather similar to lentigo maligna. However, lentigo maligna shows greater variation in the thickness of the lines making up the network, often forming an atypical rhomboid pattern associated with greyish dots, the structure tends to be irregular, and there is variation in colour.
If a skin lesion is clinically suspicious of lentigo maligna, it is best cut out (excision biopsy) with a 2–3 mm margin. Partial biopsy is less accurate than complete excision biopsy, as a single small biopsy could miss a malignant focus. However sometimes the lesion is very large, and before performing significant surgery, a partial biopsy is arranged to confirm the diagnosis. The doctor should remove a long ellipse of skin, take biopsies from multiple sites or carefully shave a representative area for histology.
The pathological diagnosis of melanoma and its precursors can be very difficult. Some lesions clinically typical of lentigo maligna are reported to show junctional melanocytic proliferation alone (with or without atypia), others have the criteria to diagnose in situ melanoma, and a few show invasive cancer.
The histological features of lentigo maligna include a predominantly junctional confluent proliferation of melanocytes and extension along adnexal structures. Solar elastosis (degeneration of elastic tissue within dermis) is typically prominent. Immunostains eg SAC R21 may improve accuracy of diagnosis in borderline cases.
The pathologist's report should include a macroscopic description of the specimen and melanoma (the naked eye view), and a microscopic description. The following features should be reported if there is invasive melanoma.
The report may also include comments about the cell type and its growth pattern, invasion of blood vessels or nerves, inflammatory response, regression and whether there is associated in-situ disease.
The Breslow thickness is reported for invasive melanomas. It is measured vertically in millimetres from the top of the granular layer (or base of superficial ulceration) to the deepest point of tumour involvement. It is a strong predictor of outcome; the thicker the melanoma, the more likely it is to metastasise (spread).
The Clark level indicates the anatomic plane of invasion.
Level |
Characteristics |
|
Level 1 |
In situ melanoma |
|
Level 2 |
Melanoma has invaded papillary dermis |
|
Level 3 |
Melanoma has filled papillary dermis |
|
Level 4 |
Melanoma has invaded reticular dermis |
|
Level 5 |
Melanoma has invaded subcutaneous tissue |
|
The deeper the Clark level, the greater the risk of metastasis (secondary spread). It is useful in predicting outcome in thin tumours, and less useful for thicker ones in comparison to the value of the Breslow thickness.
In most cases, lentigo maligna should undergo surgical excision. This means cutting it out and repairing the defect by simply closing the wound and stitching it up, creating a flap or by skin grafting.
Lentigo maligna has an unusually high risk of recurrence (up to 20%). For this reason, it is usually removed with a margin of healthy tissue, which can be difficult to achieve on facial skin. The ideal margin for all forms of melanoma in situ is 5-10mm, depending on how well defined are the edges of the lesion. Recommended margins for invasive melanoma are based on its thickness: it is 1 cm if less than 1 mm and 1-2 cm if the melanoma is over 1 mm in depth. If the margin and extent of the lentigo maligna is unclear, mapped serial excision may be recommended (margin-controlled, Mohs micrographic surgery or 'slow Mohs'), in an attempt to remove all the malignant cells and to spare healthy skin.
Studies have shown improved disease-specific survival with Mohs surgery compared to wide local excision.
Other treatments for lentigo maligna may be considered if it is difficult to remove the lesion surgically, or surgery will be very deforming, or there is a major contraindication to surgery:
However, these treatments do not offer as high cure rates as complete surgical excision.
Because the risk of invasive melanoma is small, one option in very elderly patients with large lentigo maligna is to simply photograph and watch the lesion carefully, biopsying any areas suspicious of invasive disease because of clinical or dermoscopic change.
Lentigo maligna melanoma should be completely removed surgically. If possible, there should be a 1 cm margin of normal skin around the tumour, but the margin may depend on the site of the lesion and how close it is to important structures like the mouth, eye or nose. If the local lymph nodes are enlarged due to melanoma, they should also be completely removed, which entails a major surgical procedure under general anaesthetic.
Melanoma staging means finding out if the melanoma has spread from its original site in the skin. Most melanoma specialists refer to the American Joint Committee on Cancer (AJCC) cutaneous melanoma staging guidelines (2009). In essence, the stages are:
Stage |
Characteristics |
|
|---|---|---|
Stage 0 |
In situ melanoma including lentigo maligna |
|
Stage 1 |
Thin melanoma 2 mm in thickness |
|
Stage 2 |
Thick melanoma > 2 mm in thickness |
|
Stage 3 |
Melanoma spread to involve local lymph nodes |
|
Stage 4 |
Distant metastases have been detected |
|
Lentigo maligna is not dangerous; it only becomes potentially life threatening if an invasive melanoma develops within it.
Long term follow-up involves reviewing the treated area and full skin examination to identify new lesions of concern. If the lesion was invasive, regional lymph nodes should also be examined. It may be prudent to biopsy any lesion arising within or close to the excision site.
The risk of spread (metastatic melanoma) from invasive melanoma depends on several factors, but the main one is the thickness of the melanoma at the time it was surgically removed.
The Australian and New Zealand Melanoma Guidelines report that metastases are rare for melanomas < 0.75mm and the risk for tumours 0.75–1 mm thick is about 5%. The risk steadily increases with thickness so that melanomas > 4 mm result in a 10-year survival of around 50%, according to the American Joint Committee on Cancer (AJCC) statistics.