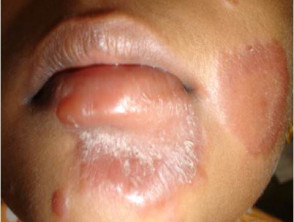
What is a lepra reaction?
Lepra reactions are inflammatory reactions occurring in leprosy, due to circulating immune complexes, vasculitis, or T-cell reaction which may be induced by treatment.
Type 1 lepra reaction
What is a type 1 lepra reaction?
The type 1 lepra reaction is a delayed type of hypersensitivity to M. leprae antigens. It is also called a lepra 1 reaction.
- Type 1 lepra reaction most often occurs after treatment for leprosy has been started, but it may also occur before treatment and after the end of the treatment.
- It reflects a strengthening of specific cellular immunity against M. leprae towards the tuberculoid type.
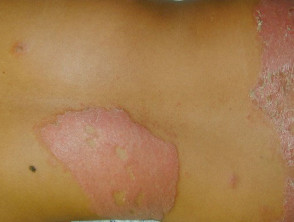
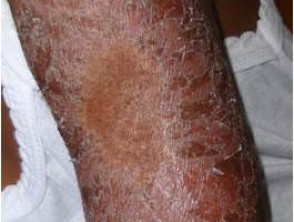
Type 1 lepra reactions in borderline tuberculoid leprosy
Who gets type 1 lepra reaction?
The lepra 1 reaction is unpredictable. It occurs in patients with borderline disease; that is, the transition between tuberculoid leprosy and lepromatous leprosy.
The classification of borderline leprosy includes:
- Borderline tuberculoid leprosy
- Borderline borderline leprosy
- Borderline lepromatous leprosy.
What are the clinical features of type 1 lepra reaction?
Type 1 lepra reactions typically affect the skin and nerves, and there are no systemic symptoms. The reaction is classified as mild or severe.
Skin signs of type 1 lepra reaction include:
- Erythema and induration of existing lesions
- Ulceration during very intense reactions.
Nerve involvement in type 1 lepra reaction, and:
- Mainly affects the cubital, sciatic, external popliteal, facial, and cervical nerves
- Often results in pain or tenderness
- May result in loss of function for more than a few days can cause muscle weakness, loss of sensation, paralysis, or deformity.
A mild type 1 lepra reaction is characterised by a few inflamed plaques and no nerve impairment. A severe type 1 lepra reaction is characterised by many inflamed plaques and nerve impairment.
How is a type 1 lepra reaction diagnosed?
A type 1 lepra reaction is clinically suspected in a patient with borderline leprosy that develops symptoms within a few months of starting treatment.
There are no routine laboratory tests. A skin biopsy may reveal:
- Granulomas
- Multinucleated giant cells
- Oedema.
There is no increase of polymorphonuclear neutrophils in the patient's blood count or a change in C-reactive protein (CRP) levels. Type 1 lepra reactions have been associated with elevated levels of serum chemokine 10.
What is the treatment for a type 1 lepra reaction?
A mild lepra 1 reaction requires supportive care. This involves:
- Topical steroids
- Painkillers
- Monitoring.
A severe type 1 lepra reaction with nerve impairment requires prompt treatment.
- First-line treatment is prednisone or prednisolone 0.5–1 mg/kg/day until inflammation has reduced, followed by a slow taper of the dose.
- Ciclosporin is a second-line treatment for severe type 1 reactions not controlled by prednisone.
- Neurolysis or nerve surgery to relieve pressure may be necessary if nerve impairment persists.
- Treatment with rifampicin, dapsone, and/or clofazimine should continue.
What is the outcome of a type 1 lepra reaction?
The natural course of an untreated type 1 lepra reaction is for it to persist for several months.
- The skin lesions continue to swell and may become confluent.
- Nerve impairment can be very severe, leading to loss of function and disability.
Type 2 lepra reaction
What is a type 2 lepra reaction?
A type 2 lepra reaction is characterised by an acute immune complex vasculitis affecting the skin and other organs. It is poorly understood. It is also called lepra 2 reaction or erythema nodosum leprosum.
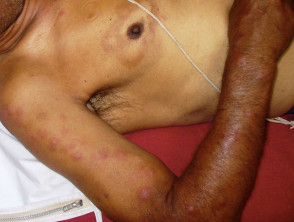
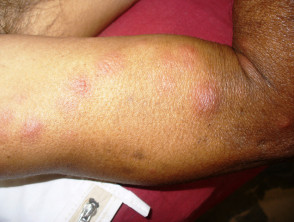
Type 2 lepra reactions
Who gets type 2 lepra reaction?
The type 2 lepra reaction occurs in patients with:
- Lepromatous leprosy
- Borderline lepromatous leprosy.
Type 2 lepra reaction is commonly associated with:
- Puberty
- Pregnancy
- Lactation.
What are the clinical features of type 2 lepra reaction?
The clinical features of lepra 2 reactions depend on its severity and which organs are affected.
In type 2 lepra reaction, the skin may show:
- Lesions scattered on any part of the body (mainly on the extensor aspect of the limbs and on the face).
- Multiple small red painful nodules
- Sterile pustules and ulcers
- Lesions may be superficial or deep in the dermis.
Other clinical features of type 2 lepra reaction may include:
- Iridocyclitis (inflammation of the eye)
- Orchitis (inflammation of a testis)
- Renal impairment or renal failure
- Proteinuria (excess protein in the urine)
- Cytolytic cholestasis (inability to produce bile)
- Fever
- Fatigue
- Enlarged lymph nodes
- Swollen painful red joints.
How is a type 2 lepra reaction diagnosed?
A type 2 lepra reaction is clinically suspected if a patient with lepromatous leprosy or borderline lepromatous leprosy complains of fever and fatigue and has multiple painful red skin nodules, whether or not they have received treatment.
Blood tests show high inflammatory markers. These include:
- A high white cell count
- A high protein C level
- Renal and liver impairment (occasionally).
Pathology is essential to confirm type 2 lepra reaction. A biopsy of a new red nodule less than 24 hours old shows:
- An infiltrate of polymorphs superimposed on chronic inflammation
- A heavy bacterial load of M. leprae (special stains may be necessary).
What is the treatment for a type 2 lepra reaction?
Treatment depends on the severity of the type 2 lepra reaction as assessed clinically and supported by laboratory tests. A mild cutaneous reaction without other organ impairment can be managed by supportive care. This includes:
- Painkillers
- Control of fever
- Regular monitoring.
Treatment for severe type 2 lepra reactions may include:
- Prednisone at a dose of about 1 mg/kg/day, quickly tapered
- Clofazimine (note that the multibacillary regimen with clofazimine prevents type 2 lepra reactions)
- Thalidomide 400 mg/day for 5–10 days, tapered over 1–2 months.
Ciclosporin, azathioprine, methotrexate, mycophenolate mofetil, and pentoxifylline have been used successfully in small trials.
What is the outcome of a type 2 lepra reaction?
Without treatment, type 2 lepra reactions continue for about 2 weeks then settle down. Recurrences are frequent.
Untreated type 2 lepra reactions can result in renal failure requiring dialysis, liver failure requiring transplantation, blindness, and/or long-term inflammation of the testicles.
Lucio phenomenon
Lucio phenomenon is a very rare, acute, and severe complication of longstanding and untreated lepromatous leprosy. It may be life-threatening.
- It mainly occurs in patients with Mexican ancestry.
- It presents with multiple punched-out and necrotic ulcers.
Lucio phenomenon is treated intensively with systemic steroids.
Leg ulceration due to Lucio phenomenon in leprosy