What is lichen spinulosus?
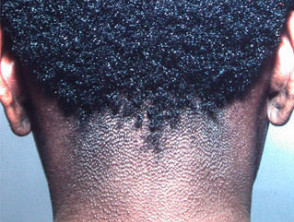
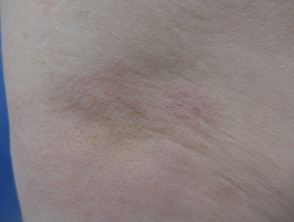
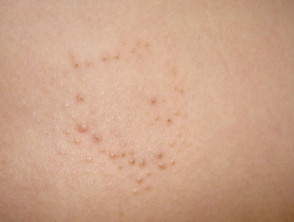
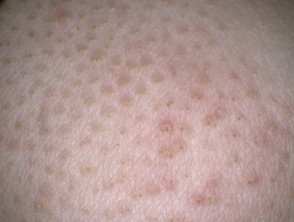
Lichen spinulosus is a clinically distinctive variant of keratosis pilaris. It is characterised by solitary or multiple patches of minute follicular papules, each centred by a horny spine, which may occur on any part of the body. It is also called "keratosis spinulosa".
What are the signs and symptoms of lichen spinulosus?
Lichen spinulosus occurs during childhood to young adulthood, with most cases occurring during adolescence. It tends to have a sudden onset and is not accompanied by other signs and symptoms. The follicular papules are small rough bumps that appear in round or oval patches, which extend and spread rapidly over a few days to affect large areas of skin.
- Patches and plaques of follicular papules grow to between 2–5cm in diameter
- Patches develop symmetrically at intervals on the neck, buttocks, thighs, abdomen, knees and extensor surfaces of the arms
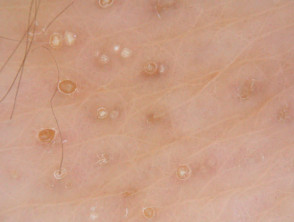
- Individual follicular papules are 1–3mm in diameter with a pointed or hair-like horny spine extending approximately 1mm around the tip of the follicle
When a patch is rubbed gently with the fingers, it has been likened to the feel of brushing your fingers over a nutmeg grater. The lesions do not cause any pain but some patients may complain of pruritus (itching).
Lichen spinulosa
What causes lichen spinulosus?
The cause of lichen spinulosus is unknown. Several possible causes have been postulated but none have been confirmed. These include:
- Reaction to an unidentified infection
- Association with atopy (inherited, familial tendency towards some form of allergy such as eczema, asthma or hay fever)
- Genetic predisposition
How is the diagnosis made?
Diagnosis is made by clinical assessment alone. At present, no specific laboratory or diagnostic tests have been identified to make or confirm a diagnosis of lichen spinulosus. Histological findings of lichen spinulosus are similar to those found in keratosis pilaris.
What is the treatment for lichen spinulosus?
There is no specific treatment for lichen spinulosus and in most cases it resolves spontaneously within 1–2 years, although it can persist for decades in some patients. Some patients may find the following useful:
- Non-soap cleansers (soap may exacerbate the dryness)
- Moisturising cream applied twice daily; try those containing urea, salicylic acid or alphahydroxy acids
- Rubbing with a pumice stone or an exfoliating sponge in the shower or bath
- Topical retinoids, which are gels or creams available on prescription. For the first few weeks of treatment, redness and peeling of the treated areas can be expected. Topical retinoids should not be used in pregnancy
- Laser assisted hair removal may also be of benefit in some cases