What is Martorell ulcer?
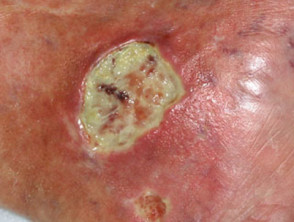
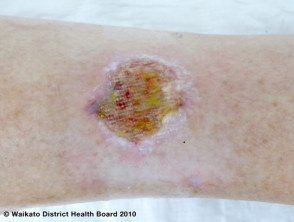
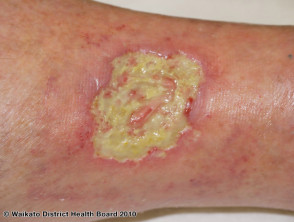
A Martorell ulcer is a very painful ulcer of the lower leg that develops in association with poorly controlled high blood pressure. It is also called Martorell’s hypertensive leg ulcer, arteriosclerotic ulcer of Martorell and Martorell hypertensive ischaemic leg ulcer (Martorell HYTILU).
Martorell ulcer
Who gets Martorell ulcer and why?
Martorell ulcers occur in patients with high blood pressure that is longstanding and often poorly controlled. There is a further association with diabetes mellitus. Martorell ulcers affect women more commonly than men. Most sufferers are in their 50s and 60s, with a reported age range of 41-86 years.
It is believed the ulcer results from narrowing of small blood vessels located in the skin, leading to increased resistance to blood flow, and a lack of blood supply to the skin resulting in skin death. In addition the blood vessels are unable to open up to allow an increase in blood supply. This is the most peripheral form of arterial vascular disease.
Clinical features of Martorell ulcer
Martorell ulcers most commonly occur on the outer aspect of back of the lower leg often just above the ankle. Over the Achilles tendon is another common site.
A significant proportion of patients report the ulcer began after skin trauma, but more commonly it starts as a painful red blister or patch which turns blue then ulcerates.
Ulcer characteristics may include:
- Extreme pain out of proportion to the size and appearance of the ulcer – it is typically described as ‘strong to excruciating’
- Solitary or symmetrical, affecting the same site on both lower legs
- Red-purple inflamed ulcer edge
- Episodes of sudden enlargement due to another area of skin death
- Irregular shape
- Satellite ulcers
- Deep, exposing underlying tendons
- Failure to respond to usual treatments for leg ulcers.
These ulcers typically occur in the absence of significant arterial or venous disease.
Extensive ulceration is associated with a poor outcome.
How is Martorell ulcer diagnosed?
Martorell ulcer should be considered clinically when a patient with longstanding high blood pressure presents with very painful leg ulcer(s) on the outer aspect of the lower leg or over the Achilles tendon. There is no significant disease affecting arteries or veins. Patients with Martorell ulcer do not suffer from rest pain or intermittent claudication (pain in the calf muscles with walking). In addition they do not suffer from kidney disease, so calciphylaxis is excluded.
A deep narrow elliptical incisional skin biopsy across the edge of the ulcer to include both normal skin and the ulcer, and extending down into the subcutaneous fat shows thickening of the arteriolar walls, often with calcium deposits which may resemble calciphylaxis. There is no inflammation of the blood vessels. A punch biopsy from the ulcer does not extend deep enough to find these characteristic changes and the diagnosis may be missed.
Blood tests such as C-reactive protein and white cell count, may be elevated.
Treatment of Martorell ulcer
Treatment is in two parts:
- Better control of blood pressure using medications that open up blood vessels and do not cause constriction of blood vessels. Therefore non-specific beta-blockers should be stopped and calcium channel blockers, specific beta 1-blockers and ACE inhibitors used if possible. A large case series has shown that even a small reduction in blood pressure can have a major impact on ulcer pain and healing.
- Ulcer care usually includes surgical debridement together with compression therapy, subatmospheric pressure technique (vaccuum-assisted closure) and, for large ulcers, skin grafting. Skin grafting leads to a rapid improvement in pain.
Pain relief is required then reduced as appropriate ulcer treatment improves pain. Paracetamol and other nonsteroidal anti-inflammatory drugs are often sufficient but, for severe pain, narcotic analgesics (opiates) may be needed initially.
Antibiotics may be required for secondary bacterial wound infection.
The role for anti-coagulant treatment (blood thinners) and sympathectomy (procedure in which sympathetic nerve fibres are cut) remain unclear at this time.
Preventative measures to reduce the risk of developing Martorell ulcer may include:
- stopping smoking
- compression stockings
- protection from trauma.
This is an important diagnosis to think of if pyoderma gangrenosum is being considered as the treatments are quite different. Immunosuppression is associated with a poor prognosis in Martorell ulcer.