What is mixed connective tissue disease?
Mixed connective tissue disease is a rare autoimmune connective tissue disorder with anti-U1RNP auto-antibodies and clinical features of three commoner connective tissue diseases:
- Systemic lupus erythematosus
- Systemic sclerosis
- Polymyositis (dermatomyositis without skin signs).
Mixed connective tissue disease is also known as Sharp syndrome.
What causes mixed connective tissue disease?
The cause of mixed connective tissue disease is not fully known. Due to the presence of autoantibodies, it is classified is an autoimmune disease.
It is most common in patients with HLA-DR4, suggesting it has a genetic background.
Who gets mixed connective tissue disease?
- Mixed connective tissue disease is approximately 4 times more common in women than in men
- It often affects women under 30 years of age
- Children may be affected.
What are the clinical features of mixed connective tissue disease?
The course of mixed connective tissue disease may be similar to systemic lupus erythematosus, or systemic sclerosis. However the clinical features tend to evolve in sequence over a number of years, making diagnosis difficult sometimes.
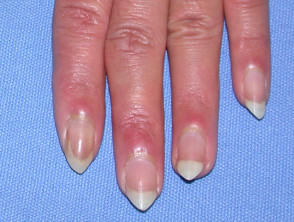
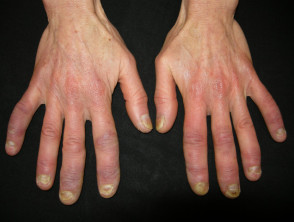
- Early symptoms often involve the hands, with Raynaud phenomenon and sausage-shaped swelling of the digits.
- Malaise, myositis, and arthritis may also develop.
Mixed connective tissue disease can be particularly severe in children, due to:
- Cardiac disease
- Renal impairment
- Thrombocytopenia.
Dermatological manifestations of mixed connective tissue disease include:
- Prominent nailfold capillaries or periungual telangiectasia
- Small vessel vasculitis and palpable purpura
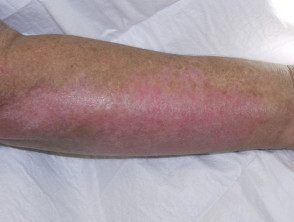
- Erythematous plaques resembling discoid lupus erythematosus
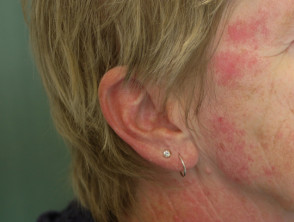
- Facial erythema
- Hair loss (localised scarring and diffuse non-scarring alopecia)
- Painful dermal nodules on hands and elbows, often calcified.
Cutaneous signs of mixed connective tissue disease
Complications of mixed connective tissue disease
Late stage complications of mixed connective tissue disease include nephritis, pericarditis and myocarditis, and interstitial lung disease.
Babies of mothers with mixed connective tissue disease and anti-U1RNP autoantibodies can develop neonatal lupus erythematosus and a rare non-lethal form of chondrodysplasia punctata.
What investigations should be undertaken in patients with suspected mixed connective tissue disease?
The presence of high titres of autoantibodies against the U1-ribonucleoprotein (RNP) complex is a defining feature of mixed connective tissue disease. This was previously termed an antibody to ‘extractable nuclear antigens’ (anti-ENA). The U1 small nuclear ribonucleoprotein particle is a target of autoreactive B cells and T cells.
Other tests
- Blood count may reveal anaemia, thrombocythaemia, and leukopenia.
- Renal function may be impaired.
- Muscle enzymes may be elevated.
- C-reactive protein and erythrocyte sedimentation rate (ESR) may be elevated.
- Patients may also have hypergammaglobulinaemia.
- Urinalysis may show proteinuria and haematuria.
- Chest X-ray may show pleural thickening and fibrosis, and signs of pulmonary hypertension.
- Echocardiogram may reveal pericarditis and pulmonary hypertension.
- Abnormal oesophageal motility may also be detected on imaging.
What treatment options are available for mixed connective tissue disease?
General
- Sun protection is essential.
Prescribed treatment
Treatment may depend on the relative severity of lupus-like, systemic sclerosis-like and polymyositis-like aspects of mixed connective tissue disease. These can include:
- Topical corticosteroids for cutaneous symptoms
- Oral corticosteroids
- Anti-inflammatories
- Anti-malarials (hydroxychloroquine), if features of systemic lupus erythematosus
- Calcium-channel blockers for Raynaud phenomenon
- Vasodilators such as sildenafil or bosentan for pulmonary hypertension.
What is the outlook for mixed connective tissue disease?
- Around one-third of patients with mixed connective tissue have mild disease, requiring only anti-inflammatories, and may go into remission where no U1-RNP antibodies are detected.
- Another one-third of patients have a progressive course developing progressive systemic sclerosis, which has a poor outcome.
- Pulmonary hypertension is the main cause of death.