What is Morgellons disease?
The term Morgellons was coined in 1674 by Sir Thomas Browne in his monograph entitled “De vermiculis capillaribus infantium". The affected child had critical breakouts of hair-like extrusions from the back which upon occurring; relieved the child from “coughs and convulsions”. Since the first description, the term Morgellons disease has faded into obscurity. It was not until 2002 when the mother of a child with a similar skin condition resurrected this term and began the Morgellons Research Foundation.
Morgellons disease is characterised by individuals describing filaments of various colours growing from the skin as well as biting or crawling sensations under the skin. It is also known as Morgellons syndrome.
For many decades, Morgellons disease has been thought to be related to delusional parasitosis, a psychiatric disorder where patients mistakenly believe they are infested with a skin parasite. However, investigators at the Morgellons Research Foundation have attempted to distinguish it from delusional parasitosis. They conclude that more information is needed to formally define this disease.
What are the signs and symptoms of Morgellons disease?
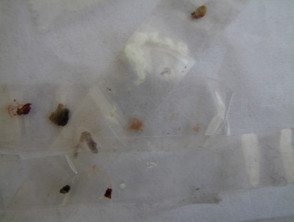
The most characteristic symptom of individuals with Morgellons disease is a sensation of filaments, fibres or spheres extruding from the skin generating uncomfortable lesions. Affected individuals may present to the doctor with a collection of these fibres for examination or may actively pick at these lesions with tweezers.
So-called fibres picked out of the skin
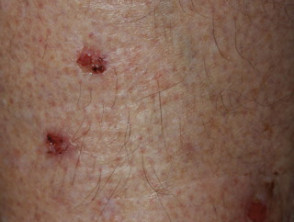
Skin findings
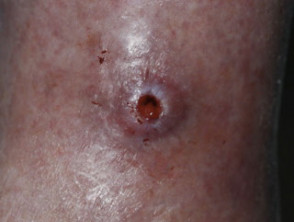
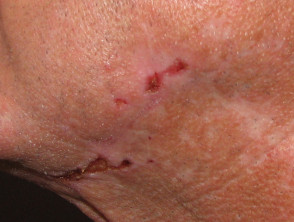
Most patients have painful skin ulcers, which they presume are the result of the fibres but are in fact the result of picking.
Morgellon disease
Other systems
There is a high degree of association with psychiatric illnesses such as bipolar affective disorder, schizophrenia, obsessive-compulsive disorder and depression.
In addition to symptoms from the skin, individuals often have symptoms from other organ systems:
- Nervous system: Headaches, fatigue, visual disturbances, tinnitus (ringing in the ear), short term memory deficits and emotional lability (instability).
- Cardiovascular: Intolerance of changes in blood pressure, irregular heart rates and high pulse rates.
- Respiratory: Variable degrees of coughing and mild shortness of breath of which there are no medically determined explanation.
- Musculoskeletal: Diffuse musculoskeletal pain, fibromyalgia and chronic fatigue syndrome.
What causes Morgellons disease?
There has been much debate over the nature of Morgellons whether it is infectious, environmental or psychiatric. There is a proposed association with Lyme disease and more recently, the Morgellons Research Foundation has identified an association with 3 more bacterial pathogens: Chlamydophila pneumonia, Babesia species and Borrelia species. The number of cases related to infection is small and there is no evidence that these bacteria directly cause Morgellons disease. A study arranged by the Centers for Disease Control (CDC) and Prevention in the US, concluded that collected fibres were mainly derived from fabric, such as cotton, and that the illness was associated with significantly reduced health-related quality of life.
Most dermatologists believe that Morgellons disease is a psychiatric illness which is analogous to delusional parasitosis and is a reflection of compulsive skin picking. In support of this theory is the absence of positive confirmatory tests.
The ulcers are distinguished from dermatitis artefacta because the patient usually accepts that they have caused the skin lesions while attempting to remove the fibres.
How is the diagnosis made?
The diagnosis is made by ruling out other skin conditions such as prurigo (which is itchy), or true infections/ infestations (eg, scabies).
- Skin scraping for mycology
- Skin biopsy for histology and culture
- Blood tests to rule out other causes of itch and erosions and ulcers
A history of drug abuse with cocaine, methylphenidate, or amphetamines must also be ascertained as these substances can induce compulsive skin picking.
What is the treatment for Morgellons disease?
The treatment of Morgellons disease is difficult. The affected individual has often seen numerous physicians and feels misunderstood. Although there are anecdotal reports of improvement with antibiotics, in most cases treatment require appropriate counselling. Patients may benefit from antipsychotic drugs.
It is important to reassure the individual that there is no true infection or infestation and to listen and understand the individual's distress. As there is a high association with psychiatric illnesses, it is important to screen for these and refer to a psychiatrist if deemed appropriate.