Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Ebtisam Elghblawi, Dermatologist, Tripoli, Libya. DermNet Editor in Chief: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. October 2017.
Neurofibromatosis (NF) is a neurocutaneous genetic disorder that affects the bone, soft tissue, skin, and nervous system.
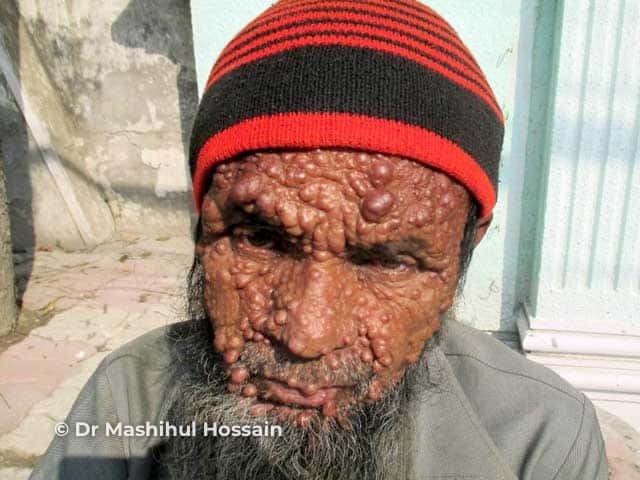
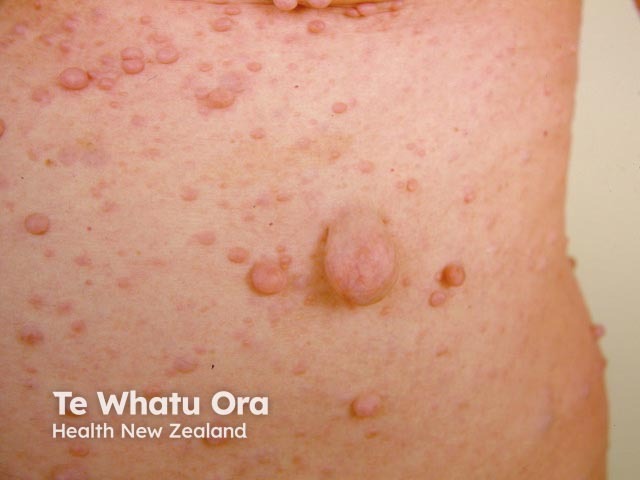
Neurofibromatosis

Neurofibromas
At least 8 different clinical phenotypes of NF have been identified. It is classified into 2 distinct types:
NF1 occurs in about 1 in 3000 births. It also known as von Recklinghausen disease. It is characterised by the presence of:
NF2 occurs in about 1 in 50,000 births. It also known as bilateral acoustic neurofibromatosis or central neurofibromatosis. It is characterised by multiple tumours and lesions on the brain and spinal cord.
Solitary neurofibroma is not associated with NF1 or NF2.
NF1 and NF2 occur as a result of defects in different genes.
The mutated gene can be inherited from a parent who has NF by autosomal dominant transmission, or it can be a founder gene due to spontaneous mutation. A parent with NF has a 50% chance of passing the gene on to each of their children.
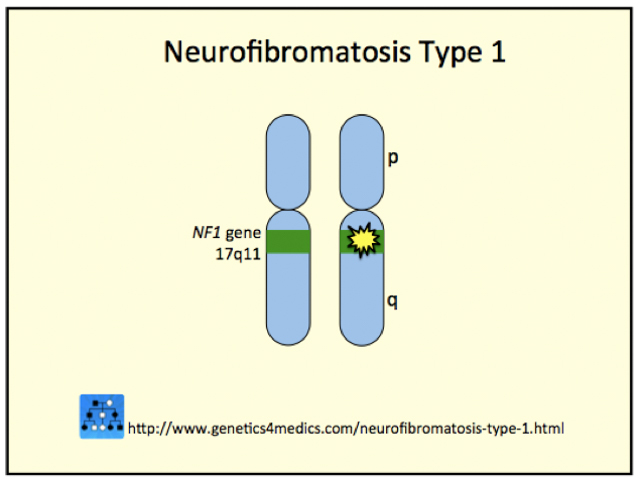
Neurofibromatosis Type 1
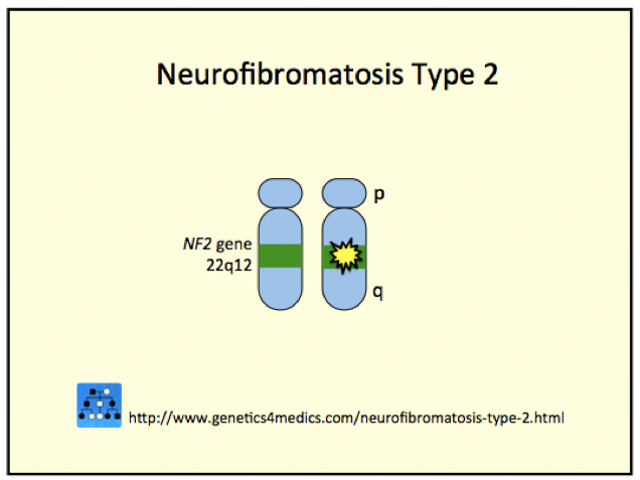
Neurofibromatosis Type 2
*Image courtesy Genetics 4 Medics
The extent and severity of manifestations of NF vary greatly from person to person and varies within the same family.
Café-au-lait macules are defined, oval or irregularly-shaped, light brown patches greater than 0.5 cm in diameter. They may be present at birth and increase in number during the first few years of life.
Although isolated café-au-lait macules can be found in many people without NF, individuals with more than 5 of these have a good chance of also having NF1, particularly if they appear on the skin within the first 5 years of life.
More than 5 café-au-lait macules are found in 1.8% of newborns, 25–40% of children, and 14% of adults with NF1.
Freckling in the armpits, known as Crowe sign, is characteristic of neurofibromatosis type 1. The freckles appear during puberty, after the development of café-au-lait macules and before neurofibromas. They may also appear in other skin folds such as the groin.
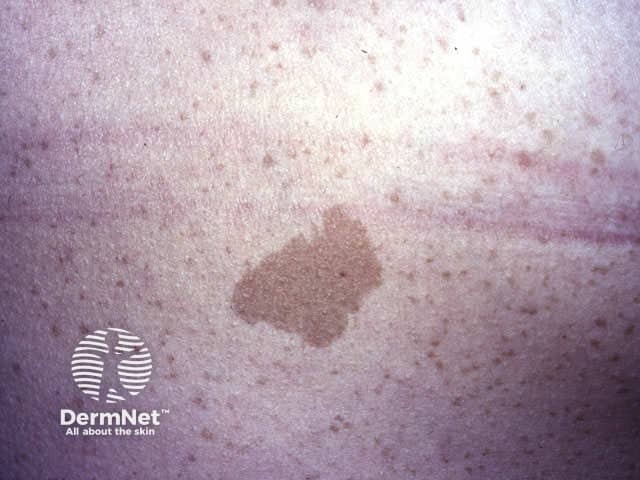
Café-au-lait macule
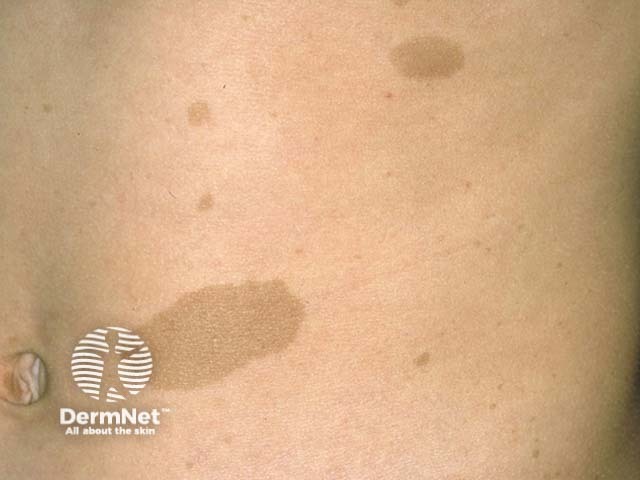
Café-au-lait macule
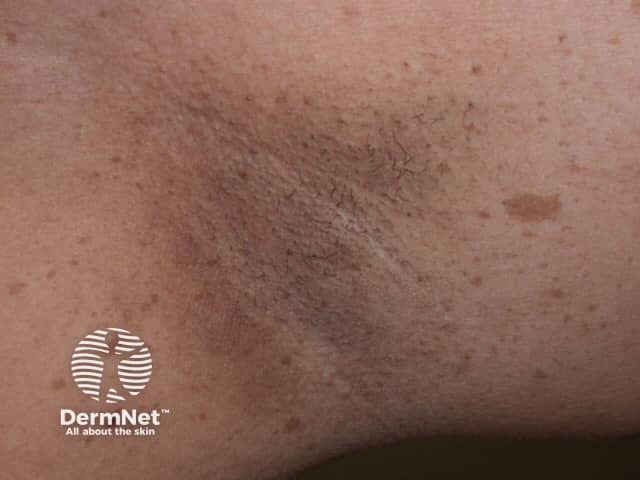
Freckling in the armpit
Lisch nodules are tiny tumours on the iris of the eye. After puberty, Lisch nodules are present in 97–100% of patients with NF1. Clinically, they do not cause any problems but help to confirm diagnosis.
Neurofibromas are composed of Schwann cells, fibroblasts, mast cells, and vascular components, and can develop at any point along a nerve. There are three types: cutaneous, subcutaneous, and plexiform. Cutaneous and subcutaneous neurofibromas are not specific for neurofibromatosis, but plexiform neurofibromas are only seen in NF1.
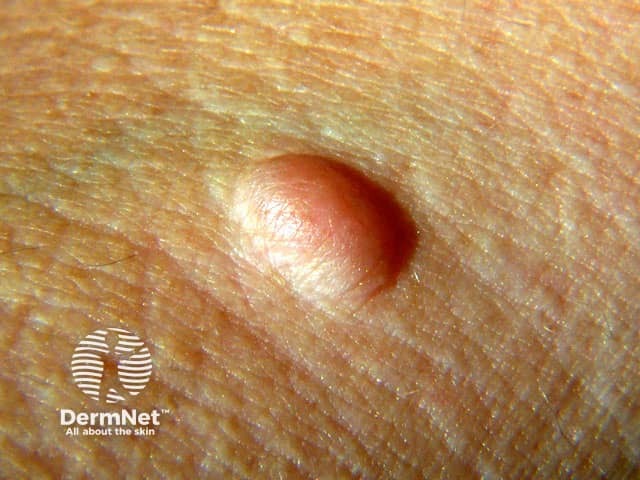
Neurofibroma
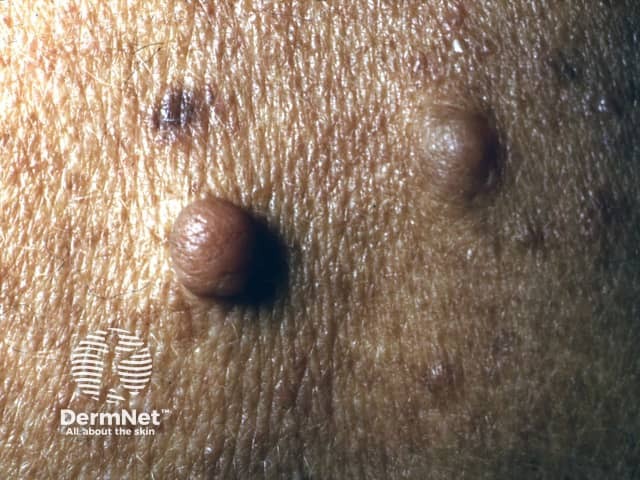
Neurofibroma
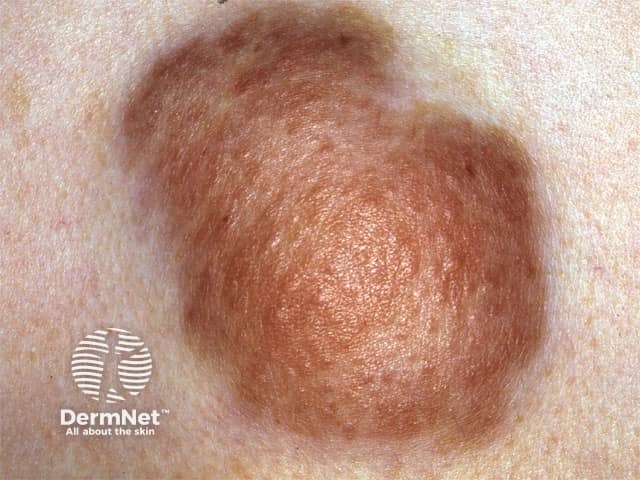
Plexiform neurofibroma
See more images of neurofibromatosis ...
The severity of cutaneous involvement in NF1 is not an indicator of the extent of the disease as internal manifestations are common and are often more serious. Problems in other parts of the body include:
Although most tumours are benign (non-cancerous), it is estimated that a person with NF1 has a 3–15% increased risk for developing cancerous tumours.
NF2 does not have as many outward signs as NF1. It is characterised by multiple tumours and lesions on the brain and spinal cord. The first symptom is usually hearing loss due to a tumour growing on one or both auditory nerves. Often this is not apparent until the late teens or early 20's.
Tumours in NF2 are usually benign. But benign tumour enlargement in the brain and spinal cord can interfere with vital functions.
The main role for follow-up is to monitor the development of tumours and intervene when necessary.
Imaging with ultrasound scans, CT scans and MRI may be arranged to determine the site of any suspected tumour.
There is no cure for NF.
Neurofibromas that become large and painful can be cut out to reduce the risk of malignancy and other complications. Facial deformity can be mitigated by aesthetic (plastic) surgery.
Genetic counselling and education about NF is important. One concern that should not be overlooked is the risk of isolation or loneliness in people with NF. People with NF are often anxious about future complications and sometimes disfiguring lesions can lead to withdrawal from society.
Targeted molecular therapies show promise for the future treatment of neurofibromatosis. MEK inhibitors such as selumetinib may offer hope in reducing the size of plexiform neurofibromas, lighten cafe-au-lait macules, and reduce pain.