What is obesity?
Obesity is a chronic disease, defined as having a body mass index (BMI) over 30 kg/m2. It is an increasing concern in healthcare across the world.
The calculation of BMI considers both height and weight. Morbid obesity is a BMI over 40 kg/m2 or a BMI over 35 kg/m2 with an obesity-related health condition such as diabetes, hypertension, or sleep apnea. A patient can also be considered morbidly obese if they weigh more than 100 pounds (45 kilograms) over their ideal body weight. BMI is not always an accurate measure of obesity, especially if unusually tall or short. And muscle weighs more than fat.
What causes obesity?
The cause of obesity is complex. It is a heritable trait influenced by the environment, genetics, and metabolism.
- Obesity occurs due to an accumulation of surplus energy over time from dietary consumption. If the intake of energy is more than is burned off, the body will convert this excess into fat.
- Obesity can reflect an unhealthy lifestyle, which is a combination of unhealthy eating and a sedentary lifestyle.
- Other factors, such as low socioeconomic status and ‘westernised’ behaviour, can contribute to obesity.
- Other causes of obesity include a genetic predisposition (although there is no universal ‘fat gene’) and hormonal causes, such as hypercortisolism (Cushing syndrome), hypothyroidism, and insulinoma.
What are the complications of obesity?
Obesity impacts physical and mental health. Obesity is a risk factor for conditions such as:
- Type II diabetes mellitus
- Hypertension
- Non-alcoholic fatty liver disease
- Certain cancers including endometrial, breast, colon, oesophageal, and renal cancer
- Various skin conditions.
How does obesity cause skin problems?
Changes in the physiology of the skin in obesity include:
- Altered epidermal barrier leading to increased transepidermal water loss
- Increased production of sebum by the sebaceous glands
- A thickened layer of subcutaneous fat leading to larger skin folds and increased sweating (hyperhidrosis)
- Impaired lymphatic flow in the subcutaneous tissue leading to lymphoedema
- Impaired collagen production leading to poor wound healing.
Mechanical factors affecting the skin relating to obesity include:
- Increased pressure on the feet due to the weight
- Stretching of the skin during weight gain
- Increased moisture and friction between the skin folds
- Decreased sensitivity to pain due to poor vascularisation to nerve endings; this can lead to ulcers.
Other skin conditions are related to hyperinsulinaemia in the metabolic syndrome.
What are the skin manifestations of obesity?
Skin conditions that can appear as a result of obesity can include the following.
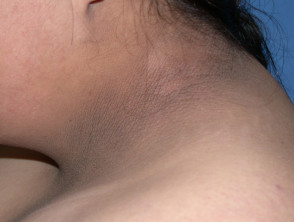
Acanthosis nigricans
Acanthosis nigricans is characterised by symmetrical, hyperpigmented, and hyperkeratotic velvety plaques in the axillae, groin, and posterior neck.
Acanthosis nigricans is associated with insulin resistance. Insulin binds to insulin growth factor (IGF) receptors on the keratinocytes and fibroblasts leading to an increase in skin thickness.
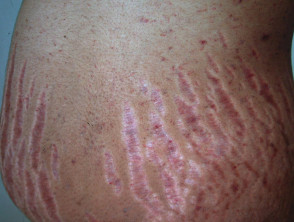
Striae distensae
Striae distensae (stretch marks) are linear atrophic plaques. They follow physical mechanical stretching of the skin when weight is gained.
- Striae are common on the breasts, abdomen, thighs, and buttocks of obese patients.
- They start as flat red or purple flattened lines, which run in the opposite direction of the lines of tension on the skin.
- Over time they become white and depressed with a wrinkled surface.
Skin manifestations of obesity
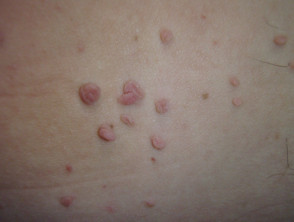
Skin tags
Skin tags (acrocordons) are associated with hyperinsulinaemia, and chaffing or rubbing of the skin.
- Skin tags are common in the axillae, neck, groin, and other skin folds.
- They are skin-coloured or soft brown papules.
- They tend to hang off the skin.
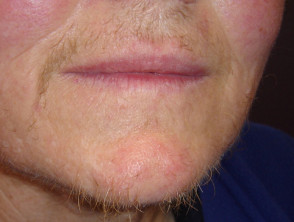
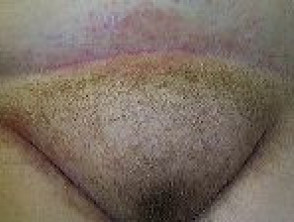
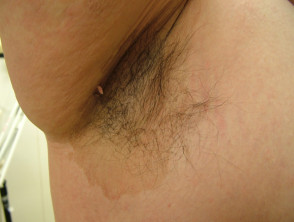
Hirsutism
Hirsutism is a male distribution pattern of hair, such as a beard, in a female.
The tendency to hirsutism is inherited and it is exacerbated by the hyperandrogenism produced by fatty tissues. The amount of abnormal facial hair positively correlates with increasing BMI.
Dercum disease
Dercum disease most often occurs in obese, postmenopausal women. It is characterised by multiple painful lipomas and bruising without obvious trauma.
Patients with Dercum disease are 50% or more above their ideal weight and pain increases with BMI.
Skin manifestations of obesity
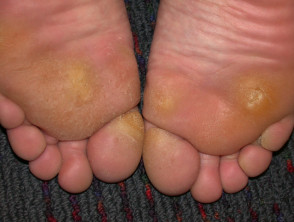
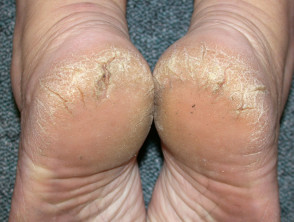
Plantar hyperkeratosis
Plantar hyperkeratosis is a form of acquired keratoderma with thickened skin over the heels and metatarsal heads.
- It affects nearly 50% of obese patients due to increased pressure on the feet when walking and standing.
- Excess weight may alter the stresses over bony prominences.
- Hyperkeratosis may cause cracked heels, pain, impair balance, and make it uncomfortable to wear shoes.
Skin conditions worsened by obesity
What skin conditions are worsened by obesity?
Skin conditions may be exacerbated by obesity and can include the following.
Psoriasis
Psoriasis is a common chronic inflammatory skin condition. Compared to people of normal weight:
- Obese patients with a BMI greater than 35 kg/m2 are twice as likely to have psoriasis
- They are more likely to have flexural psoriasis
- Their psoriasis tends to be more severe and more resistant to treatment.
Obesity may cause psoriasis through adipocyte pro-inflammatory cytokines and growth factors associated with insulin resistance-inducing growth factors.
Hidradenitis suppurativa
Hidradenitis suppurativa is a chronic inflammatory condition aggravated by obesity and characterised by scarring, abscesses, and fistulas in the axillae and groin.
The relationship to obesity probably relates to androgens, IGF, and chaffing.
Cellulite
Cellulite describes a normal age-related skin dimpling over the thighs, buttocks, and abdomen of women due to weak connective tissue around fat lobules. Cellulite is present in non-obese patients but is more obvious in obesity.
Lymphoedema
Lymphoedema presents as a soft pitting swelling of the lower legs or arms. Bacterial infection leads to scarring and further lymphoedema. It can progress to elephantiasis nostras verrucosa.
- Lymphoedema is common in obese patients due to obstruction of lymphatic return.
- Patients with a BMI greater than 30 kg/m2 have a 90% chance of developing lymphoedema at some point in their lifetime.
Intertrigo
Intertrigo presents as macerated erythema in skin folds.
- Intertrigo is caused by friction, moisture, and occlusion.
- It may be associated with a superimposed bacterial and candida infection.
- In non-obese patients, it can occur in the groin, axillae, or under the breasts.
- In obese patients, it can also occur in skin folds created by the obesity.
Obesity results in a larger skin surface in the skin folds, which can lead to increased sweating. Relatively more alkaline skin than is present in non-obese patients increases the risk of infections.
Skin conditions worsened by obesity
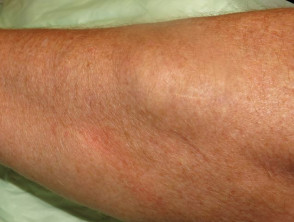
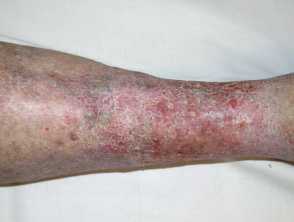
Chronic venous insufficiency
Chronic venous insufficiency leads to the pooling of blood in the veins of the lower legs with gravity.
- Obesity increases intra-abdominal pressure, which reduces the venous return from the legs, leading to failure of the venous valves and dilation of the veins (varicose veins).
- Intravascular fluid can leak into the surrounding tissue causing venous eczema, fibrosis (lipodermatosclerosis), and stasis ulcer.
What are the challenges in managing skin conditions in obesity?
Skin problems in an obese patient can be difficult to manage for a variety of reasons.
- Topical treatments can be difficult to apply.
- Increased moistness and friction lead to reduced efficacy of topical treatments.
- Poor vascularisation contributes to slow healing.
- Obese patients have an increased risk of infection.
Specific treatments can also be challenging due to patient size. For example, during phototherapy, the patient’s skin is closer to the ultraviolet bulbs than is the case for non-obese patients resulting in an increased risk of burning.
How can obesity be managed?
Managing obesity requires a lot of strength and self-motivation. The most important strategy is a change in lifestyle with both dietary changes and physical activity.
- Dietary considerations include a low-calorie diet, small portion sizes, regular mealtimes, avoidance of snacking, and avoiding foods high in fat and sugar.
- At least 150 minutes of moderate-intensity physical activity each week is important for general health even if weight loss is not required. Exercise lowers blood pressure, reduces cholesterol, improves insulin sensitivity, and improves mental health.
Surgery
Bariatric surgery may be offered to well-motivated patients with a BMI greater than 40 kg/m2 to assist in weight loss.
- There are several options, including laparascopic banding of the stomach.
- Results can include marked weight loss and improvement of diabetes, hypertension, and sleep apnoea.
- Morbidly obese patients are at high risk of surgical complications.