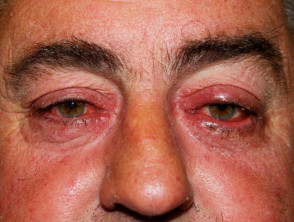
What is ocular rosacea?
Rosacea is a common skin problem in which there is mid-facial flushing, redness, prominent vasculature, swelling, papules and/or pustules. Ocular rosacea is a form of rosacea that involves the eyelids and the front of the eye. Ocular rosacea includes:
- Blepharitis
- Conjunctival hyperaemia
- Rosacea-associated keratitis
Who gets ocular rosacea?
Ocular rosacea affects adult males and females equally, with one study reporting an average age at presentation of 56 years. It is uncommon in children and generally starts after the age of 30 years.
It usually occurs in patients with existing rosacea but it can be the first sign of the disease. Ocular rosacea tends to occur in patients with facial flushing (1).
What is the cause of ocular rosacea?
The exact cause of ocular rosacea is unknown. However, immunological factors, micro-organisms on the skin surface, and reactive blood vessels are involved (1).
- Demodex mites, normal inhabitants of eyelash follicles, may stimulate inflammation in ocular rosacea and anterior blepharitis.
- Bacteria may play a role, as ocular rosacea improves with antibiotics. One theory is that bacterial lipases release toxic free fatty acids and glycerides from lipids secreted by meibominan glands.
- The pro-inflammatory cytokine interleukin 1-alpha (IL-1α) increases metallomatrix protein-9 (MMP-9) in the tear fluid. Upregulation of MMP-9 damages ocular tissues.
Obstruction of meibomian glands changes tear film composition leading to:
- Reduced tear film lipid layer
- Tear film instability
- Tear hyperosmolarity
What are the symptoms of ocular rosacea?
Ocular rosacea mostly affect the eyelids, conjunctiva and cornea. Rarely, it can involve the iris and sclera. Symptoms can include:
- Itching
- Burning and soreness
- Increased tears
- Photophobia (light sensitivity)
- Foreign body sensation.
- Dry eye
- Inflamed papules
- Corneal ulcers
- Red eye
What are the clinical signs of ocular rosacea?
Eyelid and conjunctiva
Anterior blepharitis involves the lid margin and lash line. Signs include:
- Swelling and thickening of lid margin
- Redness and dilated blood vessels
- Scaly debris at the base of the eyelashes
- Loss of eyelashes (madarosis) or misdirected eyelashes.
Posterior blepharitis involves obstruction of the ducts and loss of the Meibomian glands (2). This leads to:
- Conjunctival hyperaemia (dilated conjunctival vessels)
- Cloudy secretions
- Papillary and follicular reactions in the tarsal plate
- Conjunctival scarring
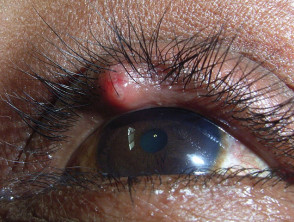
- Chalazions (granulomatous inflammatory lesions around meibomian glands)
- Hordeolum externum (stye, ie eyelash infection with Staphyloccocus aureus)
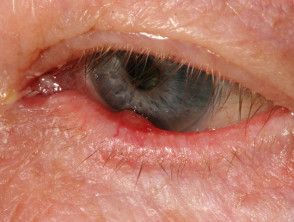
Cornea
An inflamed cornea (keratitis) is a rare but serious ocular complication of rosacea and can threaten vision (1).
- Keratitis may affect one or both eyes.
- The thinned cornea becomes inflamed with superficial punctate erosions, increased blood vessels and opacities.
- Keratitis due to ocular rosacea tends to begin at one edge or the bottom of the eye and then spread to affect lower half to two-thirds of the cornea.
- Recurrent attacks lead to corneal thinning, increased corneal opacity and vessel invasion.
- Severe ocular disease rarely can result in descemetocoele (deep ulcer) and corneal perforation.
- Corneal disease can include pannus formation (a layer of vascular fibrous tissue) and phlyctenules (allergic corneal nodules).
Iris and sclera
- Iritis: inflamed iris
- Episcleritis: inflammation of the layer between conjunctiva and cornea
- Scleritis: inflammation of the white of the eye
Iritis, episcleritis and scleritis are rare in ocular rosacea. They cause a painful, watery red eye and may affect vision.
Ocular rosacea
How is ocular rosacea diagnosed?
Ocular rosacea may be suspected in a patient with cutaneous rosacea that has eyelid or eye disease. The symptoms and signs are nonspecific, so the diagnosis is more difficult in the absence of cutaneous rosacea.
Blepharitis can also be due to seborrhoeic dermatitis, a scaly skin condition, and inflammatory papules on and around the eyelids may be due to periorificial dermatitis.
What are the treatment options for ocular rosacea?
Conservative management
- Lid hygiene: dilute baby shampoo, dilute bicarbonate solution or proprietary preparation can be applied with a cotton bud to clean eyelid margins and remove scale along the lash line.
- Warm compresses to closed eyelids for five to ten minutes daily can improve flow of meibomian gland secretions, chalazion and hordeolum.
- Artificial tears (ocular lubricants) reduce symptoms due to dry eye.
- Avoid wearing contact lenses if they irritate the inflamed eye.
Topical antimicrobials
Anterior blepharitis can be successfully treated with various topical antiseptics and antibiotics including:
- Erythromycin
- Metronidazole
- Azithromycin
- Bacitracin
- Polymyxin B
- Fusidic acid
Topical anti-inflammatory agents
- Topical nonsteroidal anti-inflammatory agents such as ibuprofen may be helpful.
- Topical steroids are used short-term to treat marked lid inflammation or rosacea keratitis. Long-term use of topical steroids should be avoided, as they can lead to glaucoma and cataracts.
- Topical ciclosporin is typically used in ocular rosacea that has not responded to topical steroids.
Systemic antibiotics
The following oral antibiotics are used for ocular rosacea:
- Tetracyclines such as doxycycline
- Macrolides such as erythromycin
They reduce bacteria, improve tear film stability and normalise meibonian gland secretions.
Oral antibiotics are generally continued for 6–12 weeks, and then slowly tapered over the course of one to two months. Further courses of oral antibiotics can be used for disease flare-ups.
Styes failing to clear with topical antibiotic are treated with oral anti-staphylococcal antibiotics such as flucloxacillin.
Oral retinoids
Oral isoretinoin can be used in low dose to treat ocular rosacea but with caution because its adverse effects include increased infections, dry eye, and other ocular effects.
Omega-3 fatty acid supplementation
Oral omega-3 fatty acid supplementation has been reported to be beneficial for some patients with dry eyes.
Surgical intervention
Surgery may be required to repair corneal opacification or perforation due to rosacea keratitis. The procedure is called keratoplasty.
Hordeola that fail to improve with warm compresses and antibiotic therapy may be excised.