Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated by Dr Jannet Gomez, August 2017.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outlook
Paronychia is inflammation of the skin around a finger or toenail. It can be acute (< 6 weeks) or chronic (persisting > 6 weeks).
Paronychia is also called whitlow. It may be associated with felon.
Acute paronychia can affect anyone. However, it is more likely to follow a break in the skin, especially between the proximal nail fold/cuticle and the nail plate. For example:
Chronic paronychia mainly occurs in people with hand dermatitis, or who have constantly cold and wet hands, such as:
Acute and chronic skin infections tend to be more frequent and aggressive in patients with diabetes or chronic debility, or that are immune suppressed by drugs or disease.
Acute paronychia is usually due to bacterial infection with Staphylococcus aureus (which may be multiresistant), Streptococcus pyogenes, Pseudomonas, or other bacterial pathogens. It can also be due to the cold sore virus, Herpes simplex (herpetic whitlow), and the yeast, Candida albicans.
The cause or causes of chronic paronychia are not fully understood. In many cases, it is due to dermatitis of the nail fold. Often several different micro-organisms can be cultured, particularly Candida albicans and the Gram-negative bacilli, pseudomonas.
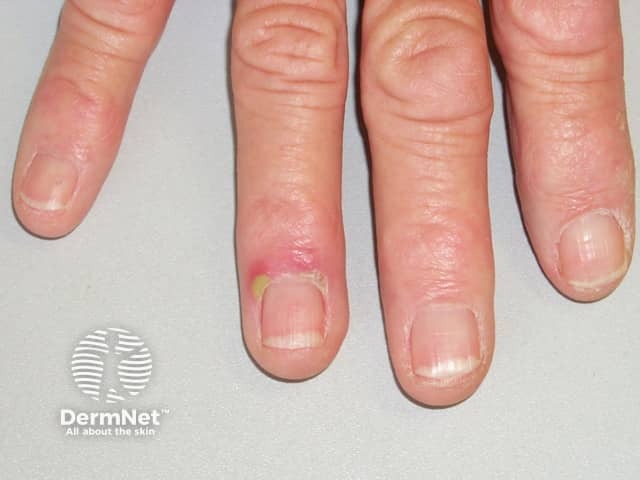
Acute paronychia develops rapidly over a few hours, and usually affects a single nail fold. Symptoms are pain, redness and swelling.
If herpes simplex is the cause (herpetic whitlow), multiple tender vesicles may be observed. Sometimes yellow pus appears under the cuticle and can evolve to abscess. The nail plate may lift up (onycholysis). Acute paronychia due to S. pyogenes may be accompanied by fever, lymphangitis and tender lymphadenopathy.
Acute candida more commonly infects the proximal nail fold.
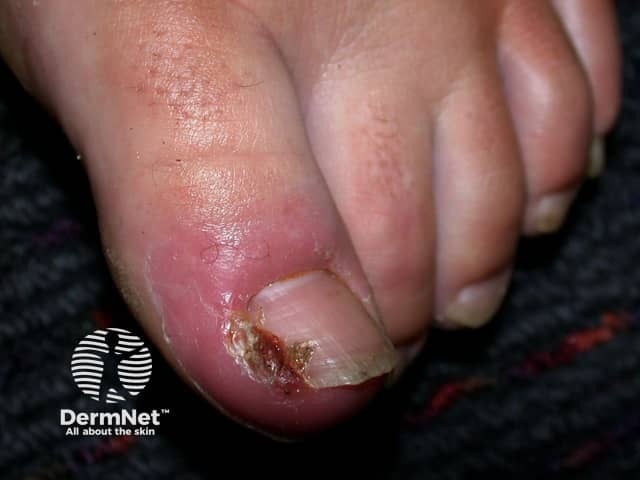
Paronychia and ingrown toenail in an athlete
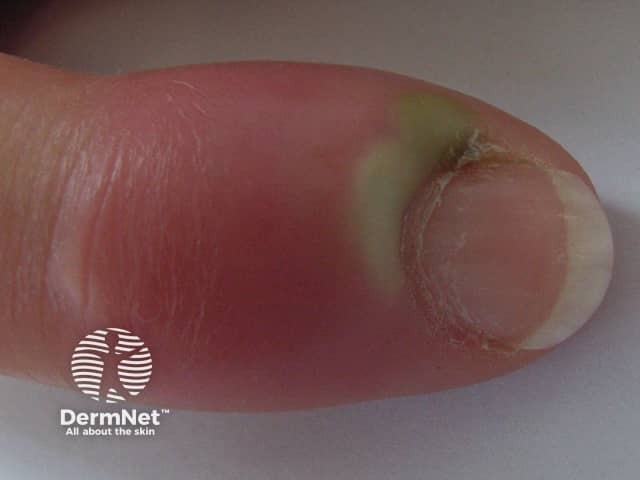
Acute staphylococcal paronychia
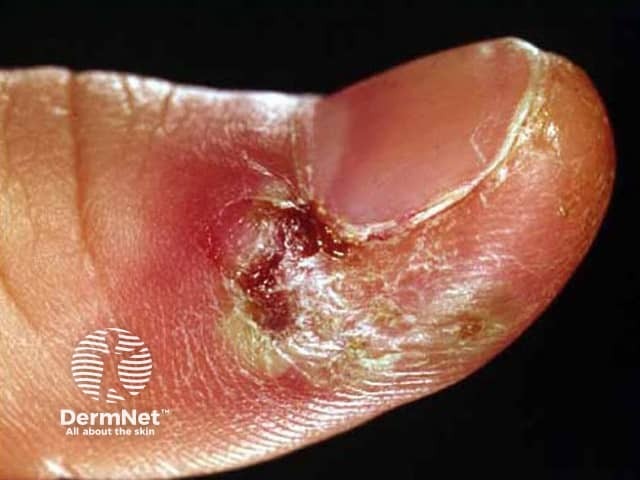
Acute herpetic paronychia
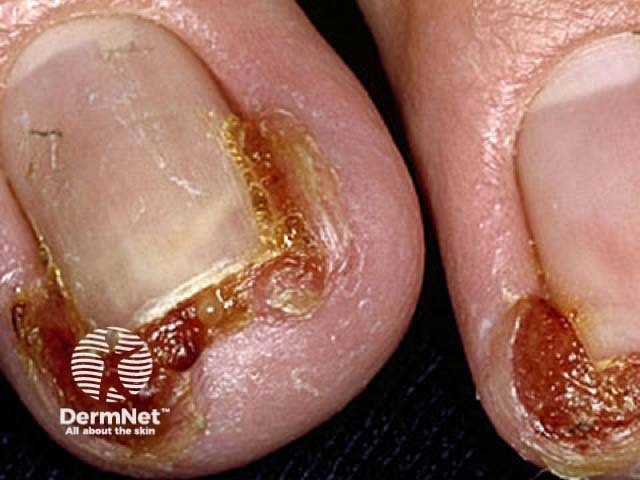
Chronic paronychia is a gradual process. It may start in one nail fold, particularly the proximal nail fold, but often spreads laterally and to several other fingers. Each affected nail fold is swollen and lifted off the nail plate. This allows the entry of organisms and irritants. The affected skin may be red and tender from time to time, and sometimes a little pus (white, yellow or green) can be expressed from under the cuticle.
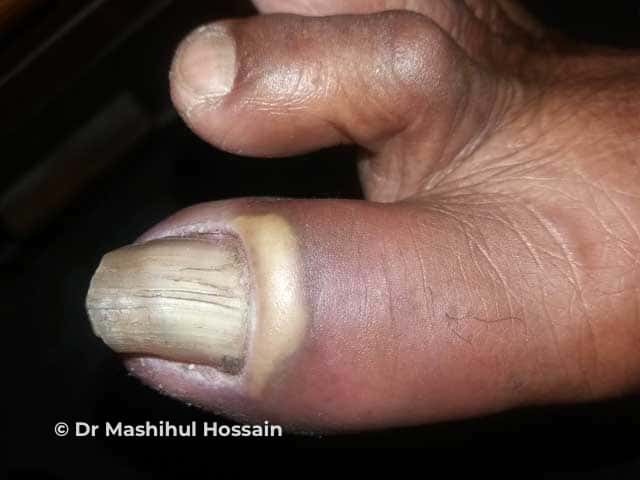
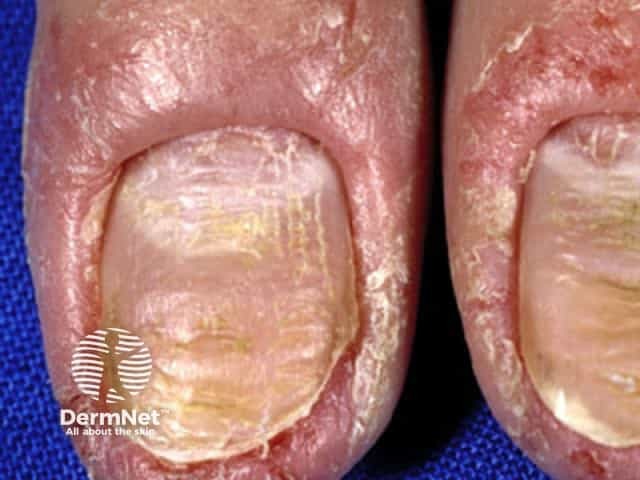
The nail plate thickens and is distorted, often with transverse ridges.
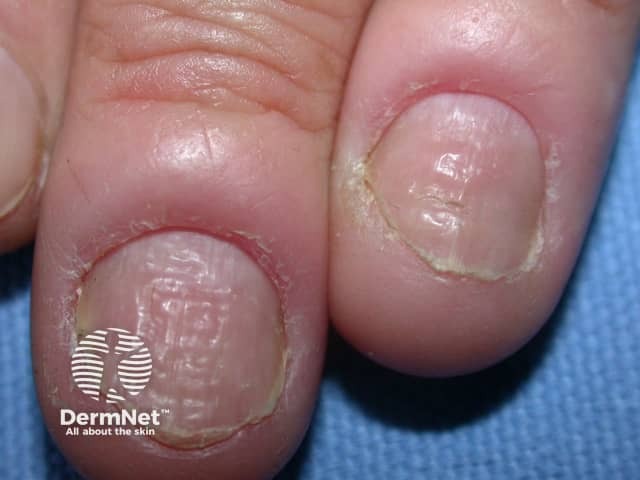
Nailfold swelling
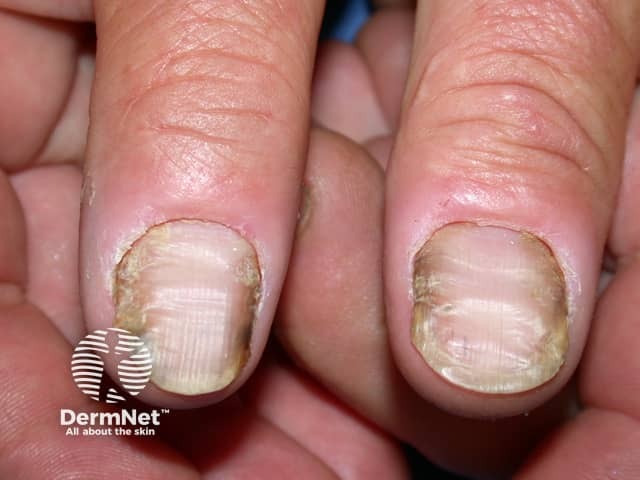
Nail dystrophy
Eczema
See more images of paronychia ...
Acute paronychia can spread to cause a serious hand infection (cellulitis) and may involve underlying tendons (infectious tendonitis).
The main complication of chronic paronychia is nail dystrophy. It is often associated with distorted, ridged nail plates. They may become yellow or green/black and brittle. After recovery, it takes up to a year for the nails to grow back to normal.
Paronychia is a clinical diagnosis, often supported by laboratory evidence of infection.
Attend to predisposing factors.
Treatment should focus on dermatitis and any microbes grown on culture [1].
Other management
Acute paronychia usually clears completely in a few days, and rarely recurs in healthy individuals.
Chronic paronychia may persist for months or longer and can recur in predisposed individuals.