Pilonidal sinus is a common condition typically affecting the region of the base of the spine or the intergluteal cleft. Other anatomic sites have been rarely reported. It is regarded by many authors within the “follicular occlusion tetrad” as the primary process appears to be follicular occlusion.
Histology of pilonidal sinus
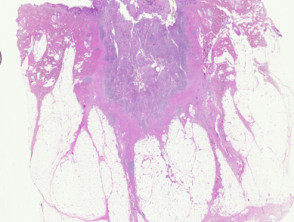
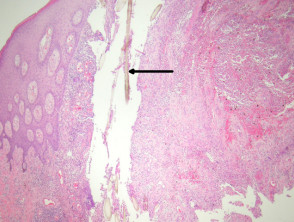
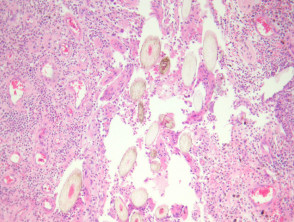
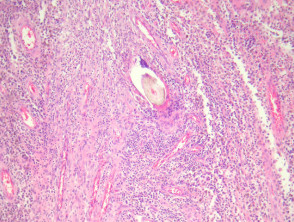
Sections show a dense inflammatory reaction usually occupying the entire dermis with erosion and ulceration of the overlying epidermis (figure 1). Free hair shafts are often seen coursing through the inflammatory focus (figure 2, arrow). Often, the free hair shafts are seen in clusters (figure 3). Dye used to outline the sinus tract for the surgeon may sometimes be seen. Surrounding the free hair shafts is a polymorphous infiltrate which may be rich in plasma cells and lymphocytes (figure 4). Foreign body-type giant cells and neutrophilic abscesses are also commonly observed.
Pilonidal sinus pathology
Special studies for Pilonidal sinus
None are generally needed.
Differential diagnosis of pilonidal sinus pathology
Follicular occlusion tetrad – Hidradenitis suppurativa (acne inversa), acne conglobata (severe nodulocystic acne), dissecting cellulitis (perifolliculitis capitis abscedens et suffodiens) will show a similar histopathology. Correlation with the clinical findings is helpful.
Squamous cell carcinoma – Squamous cell carcinoma has been reported to occur within pilonidal sinuses. Though rare, careful examination of the squamous epithelium, particularly in cases with a marked epithelial reaction pattern is prudent.