Introduction
Atopic dermatitis, also known as atopic eczema, is a chronic or relapsing skin condition characterised by intense pruritus (itch) and disfiguring rashes. It is the most common skin disorder of childhood. Around 50% of people affected by atopic dermatitis during childhood continue to have it as adults.
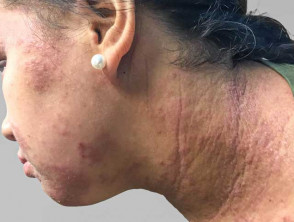
- Dermatitis often affects visible areas like the face and neck.
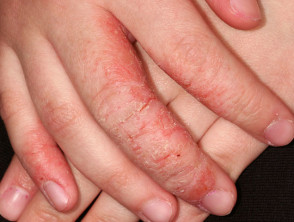
- Chronic dermatitis itches constantly.
- Rubbing and scratching leads to lichenification (thickened skin).
- Hypopigmentation, hyperpigmentation and post-inflammatory pigmentation are common.
Atopic dermatitis can lead to negative psychological effects such as social isolation and low self-esteem.
Atopic dermatitis
What are the psychological effects of atopic dermatitis?
The psychosocial effects of atopic dermatitis can be profound.
- Preschool children with atopic dermatitis are at a greater risk for hyperactivity and have a greater dependence on their parents compared to unaffected children.
- Children with atopic dermatitis are prone to teasing and bullying at school, which can lead to social isolation, poor school performance, and feelings of social stigmatisation.
- Lifestyle restrictions with atopic dermatitis include restrictions on what kind of clothing can comfortably be worn, owning pets, and physical/leisure activities like swimming or outdoor sports/activities.
- Children and adults with dermatitis may have poor self-image, low self-esteem and decreased social skills.
Assessing the impact of atopic dermatitis
The Dermatitis Family Impact (DFI) questionnaire can be used to assess the impact of atopic dermatitis on the patient and their family. It evaluates:
- The financial burden of dermatitis
- The impact on the family and social aspects of the disease
- Personal strain
- How well the family/patient is managing their disease.
At least one study has found that the impact of having children with dermatitis is similar to the family impact of having children with diabetes or asthma in regard to the cost of care, the changes that the family must make to cope with the disease, and the strain on family relationships.
Atopic dermatitis and depression
Patients with severe atopic dermatitis have high levels of depression.
- Depression is often linked to decreased quality of life due to insomnia/sleep deprivation because of the intense pruritus; this sleep deprivation can lead to emotional problems and impaired thinking.
- Stress is also a trigger for dermatitis exacerbations (flare-ups), leading to increased pruritus, changes in the permeability and homeostasis of the skin, and acceleration of the immune system response.
Where can individuals go for help?
Treatment for atopic dermatitis may require collaboration between a dermatologist and a psychologist or psychiatrist to deal with both the physical and psychological effects of the disease.
Treatment for the psychological components of the disorder can include:
- Psychological counselling, including cognitive behavioural therapy, relaxation therapy and habit reversal training
- Psychotropic medications, such as antidepressants
- Involvement in patient support groups.