What is reflectance confocal microscopy?
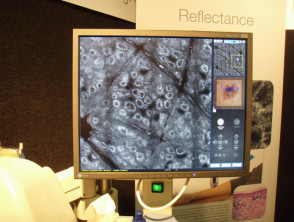
In dermatology, reflectance confocal microscopy (RCM) is a non-invasive imaging technique that enables in vivo visualisation of the epidermis down to the papillary dermis in real-time. Resolution is almost comparable to conventional histology. It has the advantage of allowing the clinician to do a “virtual biopsy” of the skin and obtain diagnostic clues while minimising unnecessary skin biopsies.
The confocal microscope was invented by Prof Marvin Minsky in the mid-1950s. RCM in skin imaging was later described by Dr Rajadhyaksha and his colleagues in 1995. Since then, there has been a lot of interest in using this technique in the diagnosis of skin malignancies such as melanoma and in inflammatory skin conditions.
How does reflectance confocal microscopy work?
RCM uses the diode laser as a source of monochromatic and coherent light.
- The light passes through a beam splitter, a scanning and focussing optical lens and a skin contact device.
- It penetrates the skin and illuminates a small tissue spot.
- Light reflected from the focal point reflects back through the lens, which focusses it into a small pinhole and forms an image on a photodetector.
- The pinhole only allows light from a focal point to pass through (i.e. it is confocal), and prevents light from another tissue point or out-of-focus plane from getting through.
RCM relies on reflectance (back-scattering) of light from structures with endogenous contrast, such as melanin, haemoglobin and some organelles. Reflectance occurs at the boundaries of two structures with different refractive indices, such as membranes, keratohyaline granules and melanosomes.
The commercially available Vivascope® 1500 uses a laser of 830 nm, as this wavelength does not cause tissue injury for the patient or injury to the eyes of the operator. The depth of penetration is 200–300 µm, which generally corresponds to the papillary dermis or upper reticular dermis.
Confocal microscope
How is reflectance confocal microscopy used?
RCM is a painless procedure.
- A small amount of immersion oil is applied to the skin (refractive index of oil is close to that of the stratum corneum).
- A glass window is attached to a metal ring and placed over the oil.
- The glass window is fixed to the skin using medical adhesive tape to prevent skin movement.
- A water-based immersion medium, e.g water or water-based gel, is placed inside the ring, which is magnetically attached to the optical lens housing of the microscope.
RCM allows horizontal scanning of the imaged tissue at a pre-selected depth.
- Each basic image generated is 5 mm x 5 mm. Entire lesions up to 8 mm x 8 mm can be imaged.
- The basic images are stitched together by a computer forming a block or mosaic.
- A vertical series of images can be obtained at the same horizontal position and is called a stack.
- A cube is a stack of blocks/mosaics.
The RCM device has an attachment for a dermatoscope. This allows dermatoscopic-confocal microscopy correlation. Video of capillary blood flow can also be filmed.
What are the potential clinical applications of reflectance confocal microscopy?
RCM can be used to diagnose benign and malignant skin lesions, such as:
- Melanoma, especially lentigo maligna
- Basal cell carcinoma
- Squamous cell carcinoma
RCM can be used to monitor treatment, such as:
- Effectiveness of imiquimod in actinic keratosis
- Assess appropriate surgical margins ex vivo in Mohs surgery
A consensus group determined that the best indications for the use of RCM are (Jan 2017):
- Lesions located on the head and neck, damaged by chronic sun exposure
- Lesions dermoscopically typified by regression
- Amelanotic tumours.
RCM can also be used to diagnose inflammatory conditions, such as:
- Psoriasis
- Dermatitis/eczema
- Infestations, e.g scabies.
What features can be seen in normal skin using RCM?
Stratum corneum
- The horny layer is a highly refractive (bright) surface surrounded by visible skin folds (these are dark).
- Corneocytes are large (10–30 µm), polygonal and without a visible nucleus.
Stratum granulosum
- Keratinocytes in the granular cell layer have well-demarcated outlines that form a honey-combed pattern.
- The cytoplasm appears white and grainy due to organelles and keratohyaline granules.
Stratum spinosum
- Keratinocytes in the squamous cell layer are smaller (15–25 µm), polygonal, have thin white cytoplasm and oval dark nuclei.
- They also form a honey-combed pattern.
Stratum basale
- Basal cells are small (7–12 µm), uniform in shape and size, and appear brighter due to the presence of melanin caps above their nuclei.
- Melanocytes and pigmented keratinocytes appear as solitary round/oval structures and are indistinguishable.
- In skin phototypes II to IV, the basal keratinocytes form clusters of round cells with highly refractive keratinocytes and display a cobblestone appearance on upper confocal sections.
Dermo-epidermal junction (DEJ)
- At the DEFJ, small basal cells and melanocytes form bright rings surrounding dark dermal papillae
- Within these, small blood capillary loops with blood vessels are seen.
- This arrangement is termed an “edged papilla”.
Dermis
- Blood vessels in the dermis appear as dark tubular structures containing weakly and brightly refractile cells.
- Collagen fibres appear as bright, elongated fibrillary structures.
RCM features of skin lesions
Melanoma
Early melanoma is characterised by:
- Alteration of the DEJ, which is flattened and disarranged
- Ill-defined papillary contours (“non-edged” papilla)
- Papillae that alternate with single-cell proliferations and nests of atypical cells to form an “aspecific” pattern.
- Dermal papillae that are replaced by atypical cells.
Features of more advanced melanoma are:
- Malignant cells occupying the entire junction
- Loose, large, bright cells within the epidermis
- Large bright cells with dark eccentric nuclei in the superficial epidermis (pagetoid spread)
- Cerebriform nests in nodular melanoma
Melanocytic naevi
- A meshwork pattern is present in a majority, corresponding to the junctional component.
- Junctional nests appear as well outlined, rounded structures, sometimes connected to the epidermis.
- In compound naevi, a clod pattern is seen and corresponds to superficial dermal nests of melanocytes.
Benign keratosis
- A benign keratosis is used to describe a solar lentigo, a seborrhoeic keratosis, a lichen planus-like keratosis or a combination of these.
- At the dermo-epidermal junction, there is an increase in the density of dermal papillae surrounded by a bright monomorphic layer of cells.
Histology and dermoscopy of a benign keratosis
Reflectance confocal microscopy of the same keratosis
Credit. Dr Manu Jain.
Figure 1. RCM image of a benign keratosis at the dermo-epidermal junction shows round to polymorphous edged papillae surrounded by a rim of bright monomorphous cells (arrowhead) and a corneal pseudocyst (arrow).
Figure 2. RCM image of a benign keratosis at the suprabasal part of the epidermis shows a cobblestone pattern: closely set, bright round cells even in size and brightness with uniform spacing separated by a less refractive polygonal outline.
Basal cell carcinoma
Features of basal cell carcinoma (BCC) are:
- Tightly packed cells with peripheral palisading.
- The grouped cells are outlined by a dark space
- They are often surrounded by prominent blood vessels.
Squamous cell carcinoma
The features of squamous cell carcinoma (SCC) are:
- Variable keratinocyte atypia.
- Atypical honeycombed pattern and architectural disarray of variable degree within stratum granulosum and spinosum
- Round blood vessels going through the dermal papillae perpendicular to the skin surface Bright scale-crust on the skin surface
RCM features of inflammatory diseases
Inflammatory diseases can be grouped into 4 main categories.
- Spongiotic dermatitis
- Psoriasiform diseases
- Diseases with interface changes
- Pigmentary disorders other than tumours
Psoriasis
Features of chronic plaque psoriasis are:
- Non-rimmed papilla at the dermo-epidermal junction. The papillae are surrounded by faint rings of basal keratinocytes rather than bright rings.
- Epidermal thickening
- Several vessels within the non-rimmed papillae
Spongiotic dermatitis
Spongiotic dermatitis is characterised by:
- Intercellular and intracellular fluid accumulation lead to a regular honeycombed appearance.
- Spongiotic vesicle appear as hollow dark spaces between the granular and spinous layer
- Exocytosis is seen as round, bright cells interspersed between the keratinocytes, around blood vessels and adnexal structures and in the dermis.
Limitations of RCM
In the commercially-available confocal microscope, the depth of imaging is 200–300 µµm, which corresponds to the papillary dermis. Therefore lesions or inflammatory processes that are deeper than that cannot be assessed.
Other limitations include:
- Cannot differentiate benign spitzoid lesion from melanoma in most cases.
- Lesions with abundant scale can impair visualisation of the dermoepidermal junction.
- Requires extensive training to interpret images.
- The instrument can be bulky and difficult to place in small concave sites, such as ear, inner canthus.