Introduction
Scientists and technicians engage in important research and analysis in laboratories all over the world. However, this sector is at high risk of skin conditions due to the nature of laboratory work itself.
In one study of 5641 workers from 137 different laboratories, 23% of workers had developed skin conditions due to the handling and care of laboratory animals.
Why are scientists and technicians at risk for skin disorders?
Risks to scientists and technicians who work in laboratories include:
- The fast-paced nature of laboratory work
- Tasks like pipetting, mixing, compounding, or loading autosampler devices can bring workers into contact with a variety of chemicals
- The presence of chemicals such as dyes, solutions, solvents, disinfectants and other cleaning agents
- The potential for exposure to contact allergens and irritants.
Understanding occupational skin disorders
Occupational skin disorders are caused or made worse by the nature of a person’s job. They account for about 80% of occupational disease worldwide, but in the United States and other developed countries, rates have been falling due to an increase in both safety measures and automation. The layered, flexible nature of skin provides reasonable protection against chemicals, extremes of heat and cold, solar radiation, allergens and irritants. However, different types of work can lead to breaches in the skin’s defences and to the development of dermatoses.
Skin disorders associated with scientists and technicians
There are several types of skin disorder associated with laboratory work.
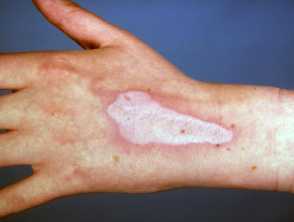
Chemical burns
Chemical burns are a common complaint among laboratory workers. This is due to tasks that involve close contact with a variety of chemicals.
- Personal protective equipment — gloves, goggles and protective aprons — may reduce chance of exposure.
- Washing facilities should be present on site to reduce worker risk.
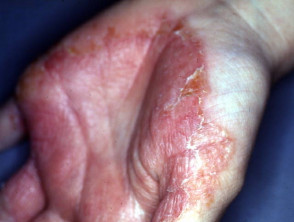
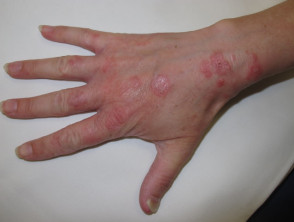
Contact dermatitis
Irritant and allergic contact dermatitis
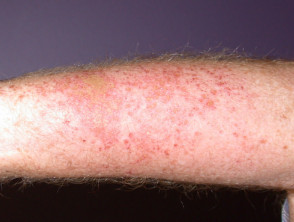
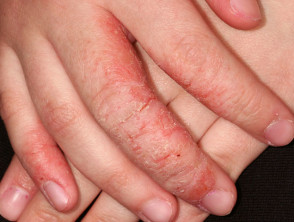
Irritant contact dermatitis and allergic contact dermatitis are common in laboratory workers. This is mainly due to frequent exposure to allergens and irritants. Contact dermatitis can also be caused by contact with laboratory animals.
- Common signs and symptoms of dermatitis include redness, swelling, blisters, oozing and weeping or dryness.
- The most common sites of contact dermatitis are the backs of the hands, wrists and forearms.
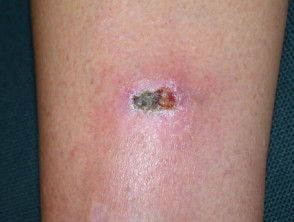
Mechanical injury
Mechanical injuries are another risk for laboratory workers. They are often due to handling sharps like lancets, glass tubes, etc.
- The fast-paced nature of laboratory work and/or ignoring of proper protocols is a contributing factor in many of these injuries.
- Mechanical injuries put laboratory workers at risk for secondary bacterial wound infections.
Skin infections
Workers in microbiology laboratories are exposed to many microorganisms that can infect the skin, particularly if the integrity of the skin barrier is compromised. Such infections include:
- Bacterial skin infections
- Fungal skin infections
- Viral skin infections
- Infections related to arthropods, helminths and other bugs.
Skin infections
Workplace risk assessment
A risk assessment of the laboratory workplace should include an assessment of the:
- Physical working conditions (proper lighting, etc.)
- Regular maintenance of laboratory equipment
- Safe storage, handling and disposal of laboratory chemicals and sharps
- Knowledge of the individual chemicals worked with, their properties and their risks
- Education of employees about laboratory safety
- On-site provision of showering and rinsing facilities
- Protocols for various laboratory procedures.
A collaboration between laboratory managers and workers is needed to ensure that laboratories stay truly safe and that accidents are prevented.
Personal protective equipment
Depending on the precise nature of the work, personal protective equipment for workers in the laboratory can include:
● Gloves
● Goggles
● Protective aprons
● Protective clothing and shoe covering
● Masks.
Such personal protective equipment can protect the skin — not only on the hands but also the rest of the body — when dealing with hazardous materials.
Hand care advice for scientists and technicians
Proper hand care can reduce the risk of occupational skin diseases. It can include:
- Proper use of personal protective equipment (see above) to protect the skin from exposure
- Washing hands after disposal of personal protective equipment and following a general hand-washing protocol, using alcohol-based gels/sanitisers as needed
- Opting for use of non-latex gloves to avoid latex allergy
- Using emollients and moisturisers
- Seeking medical help at the first signs and symptoms of skin irritation or breakdown.
How is occupational skin disease diagnosed?
Diagnosis of occupational skin disease should be based on:
-
- A detailed personal and medical history, including a personal history of atopy (especially atopic eczema)
- An occupational history, including the nature of job and the potential for work-related exposure to allergens or irritants
- The appearance and distribution of skin signs
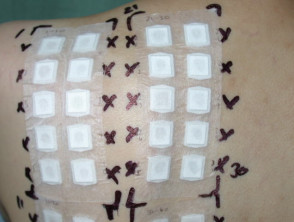
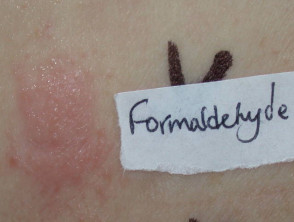
- Patch tests if an allergic reaction is suspected
- Laboratory tests for bacteria, fungi, viruses, arthropods, helminths and other bugs.
Patch tests
What is the treatment for occupational skin disease?
Treatment for occupational dermatoses may involve:
- Topical corticosteroids, with oral prednisone if indicated
- Emollients
- Referral to a dermatologist for phototherapy or immunomodulation therapy if the dermatitis is persistent or resistant to first-line therapy.