What are face masks and respirators?
Face masks and respirators are examples of personal protective equipment (PPE) worn over the mouth and nose to protect the wearer from inhaling particles and dust, and to reduce the risk of spread of airborne infectious pathogens. Face masks are used by the general public during viral epidemics, and routinely in occupational settings such as healthcare facilities and dusty work environments.
Face masks
Mask etiquette image from World Health Organization, 2020
What are the common types of face masks and respirators?
- Cloth masks:
- Filter large particles such as pollen and dust
- 2–3 layers of fine weave cloth is required to filter respiratory droplets
- Not recommended in medical/healthcare settings.
- Surgical/medical masks:
- Loosely worn
- Filter sprays and large-particle respiratory and salivary droplets
- Reduce transmission to and from the wearer.
- N95 respirator masks, and other filtering face pieces (FFP):
- Individually fitted to create a facial seal
- Provide at least 95% protection against airborne particles 0.3 micron or greater in diameter
- Exhalation valves make breathing easy but exhaled air is not filtered so infectious particles can be transmitted from the wearer to others.
Types of masks
Why do face masks cause skin problems?
The skin barrier can be compromised due to increased humidity and temperature, created from breathing in a closed environment under a face mask. This causes follicular occlusion, increases sebum secretion, and changes skin microflora. Mechanical effects are due to friction and pressure.
Further contributory factors include:
- Type of mask
- N95 respirator masks > surgical mask > cloth mask
- Duration of mask wearing
- Prolonged wearing and re-use of disposable masks
- Pre-existing skin problems
What are the clinical features of mask-related skin problems?
Common skin symptoms associated with face mask usage
Facial itch, redness, rash, dryness and peeling, swelling and numbness, pain and tingling, and oily skin are commonly reported symptoms related to face mask usage, particularly when a mask is worn for more than 4 hours daily.
Mechanical skin damage
Mechanical skin damage can initially present as pressure indentations around the nose from the metal nose clip, or itching, redness, and scaling behind the ears due to the earloops.
Friction may also cause koebnerisation of a pre-existing skin condition such as psoriasis and vitiligo.
Mechanical skin damage may progress to erosions, ulceration, postinflammatory hyperpigmentation, and scarring.
Acneform eruptions
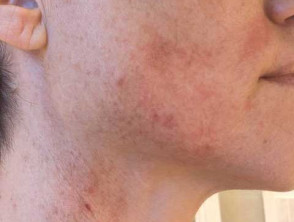
Mask wearing can induce or exacerbate acne, an effect that has been colloquially termed ‘maskne’, a form of acne mechanica. It is the commonest skin rash related to face masks and particularly affects the cheeks. Rosacea flares can also be triggered by face mask usage. Acne and rosacea flares due to face masks can impact quality of life.
Contact dermatitis
Underlying skin conditions such as atopic dermatitis increase the risk of developing irritant contact dermatitis (ICD) due to a pre-existing defective skin barrier [see Barrier function in atopic dermatitis].
Allergic contact dermatitis (ACD) is a less common cause of mask reactions. Identifying the allergen can be difficult due to the variety of constituents used by manufacturers and the lack of publicly available information. Reported causes of ACD related to masks include:
- Rubber accelerators in the elastic bands of the mask
- Metal eg, nickel, from the nose piece/strip
- Antimicrobials in surgical masks eg, formaldehyde, bromo-2-nitropropane-1,3-diol (a formaldehyde-releaser)
- Methyldibromoglutaronitrile (dibromodicyanobutane) is a preservative found in some adhesives used in the construction of N95 respirators and surgical face masks
- Polyurethane sponge strip in N95 respirators.
Urticaria
Cheilitis
- Tightness and chapping of the lips (cheilitis)
- Angular cheilitis
Exacerbation of pre-existing skin conditions
Worsening of seborrhoeic dermatitis may present with increased itch, redness, and peeling, particularly with prolonged mask-wearing. This is thought to be due to the overgrowth of malassezia yeasts under the mask.
Reactions to face masks
How can face mask reactions be prevented?
Before wearing a face mask
- Use a mild cleanser and non-comedogenic moisturiser to protect the skin barrier and reduce friction
- Apply a lip balm
- Avoid toners, fragranced products, and greasy creams that may irritate the skin or increase the risk of allergic contact dermatitis
- Treat a pre-existing skin condition
- Do not spray mask with disinfectant
- Wash cloth face masks daily
While wearing a face mask
- Trial different masks and choose one of a material that does not irritate
- Ensure the mask is properly fitted
- Consider a lining between your skin and the mask to reduce irritation and friction
- Tricks to avoid earloop pressure include using a paperclip or standard hospital wristband to link the loops behind the head
- Minimise duration of mask-wearing where possible, aiming for a five-minute break every few hours
After wearing a face mask
- Inspect the skin for signs of reactions and start appropriate treatment early
- Moisturise to protect the skin barrier
- Minimise re-use of a face mask
What is the treatment for face mask reactions?
General measures
- Reduce mask usage if safe to do so
- Select a comfortable mask that is not too tight
- Consider a lining between the mask and skin
Pressure injuries
- Protect skin at pressure site
- Compresses for 20 minutes every 2–3 hours eg, using cold water, normal saline, or diluted povidone-iodine
Acneform eruptions
- Standard acne and rosacea treatments as appropriate
Contact dermatitis
- Identify and avoid the irritant and/or allergen eg, patch testing
- Moisturise
- Mild potency topical steroid, or topical calcineurin inhibitor
Urticaria
- Oral antihistamines may give symptomatic relief
Cheilitis
- Barrier lip emollient
- Mild potency topical steroid
What is the outcome for face mask reactions?
Skin reactions to face masks will usually improve or resolve with reduced or cessation of mask use.