What is spitzoid melanoma?
Spitzoid melanoma is a malignant melanoma that is histologically similar to a benign skin lesion, Spitz naevus.
What are the clinical features of spitzoid melanoma?
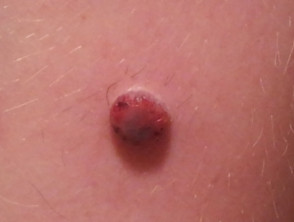
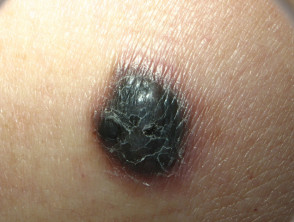
Spitzoid melanoma presents as a changing and enlarging papule or nodule. It can be amelanotic (nonpigmented, red) or pigmented (brown, black or blue). Advanced Spitzoid melanoma may be crusted and ulcerated. It is most often located on the head or extremities.
Spitzoid melanoma is often round in shape and uniform in colour. Therefore, it does not follow the commonly used ABCDE criteria of melanoma (Asymmetry, Border irregularity, Colour variation, Diameter over 6 mm in greatest dimension) [1]. It can arise de novo (a new lesion), or within an existing Spitz naevus [2].
When the histological diagnosis is uncertain, the diagnosis of Spitzoid Melanoma of Uncertain Malignant Potential (STUMP) may be made.
Differential diagnosis of spitzoid melanoma
Spitzoid melanoma may resemble a number of other skin lesions, including:
- Melanocytic naevus (mole)
- Spitz naevus
- Haemangioma
- Basal cell carcinoma
- Pyogenic granuloma
Spitzoid melanoma
Who gets spitzoid melanoma?
Spitzoid melanomas are more common in adults than in children, but due to a very low rate of other cutaneous melanoma subtypes in children, the incidence of spitzoid melanomas is relatively high in children [2].
Spitzoid melanomas can occur in any ethnic group and on any body location [3].
How is Spitzoid melanoma diagnosed?
Spitzoid melanoma is diagnosed on skin biopsy of an enlarging nodule.
Histologically and cytologically, Spitzoid melanomas share common features with Spitz naevi. Compared to Spitz naevus, spitzoid melanoma:
- Lacks symmetry and uniformity
- Is poorly circumscribed
- May involve epidermis and dermis as a confluent mass
- Cells do not mature in deeper areas
- Has mitotic figures deep in the dermis, which may be atypical
- May be necrotic.
Cytology shows high nuclear to cytoplasmic ratios with dusty cytoplasmic melanisation along with large eosinophilic nucleoli [3].
What is the treatment for spitzoid melanoma?
Spitzoid melanoma should be completely excised with a margin of normal tissue. The recommended clinical margins depend on the measured thickness of the tumour, as with other melanomas. The specimen should be carefully examined under the microscope.
In thicker tumours, a sentinel lymph node biopsy may be recommended to determine whether the melanoma has spread. The role of SLN biopsy is controversial in the management of atypical spitzoid melanocytic lesions and the reliability of any associated prognostic information unclear. Patients with spitzoid melanoma and positive sentinel lymph node biopsy have been shown to have a more indolent disease course than those with positive sentinel lymph node biopsy and non-spitzoid melanomas.
What is the outlook for patients with spitzoid melanoma?
The prognosis of spitzoid melanoma in adults is similar to other melanomas of comparable thickness [3].
In a study comparing ages of patients with spitzoid melanoma, it was found that there was an 88% 5-year survival rate in children (ages 0–10) with metastatic spitzoid melanoma, compared to a lower, 49% 5-year survival in children aged 11–17 years.[4] The prognosis of children with spitzoid melanomas is better than that observed in adults[5].