Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
A thermal burn is a burn to the skin caused by any external heat source. This may be in the form of a naked flame from an open fireplace or house fire, a scald from steam, hot or molten liquid, or via direct contact with a hot object such as a hot oven rack or hot cooking pan.
Other types of burns include radiation burns, sunburn from the sun's ultraviolet rays, chemical burns and electrical burns.
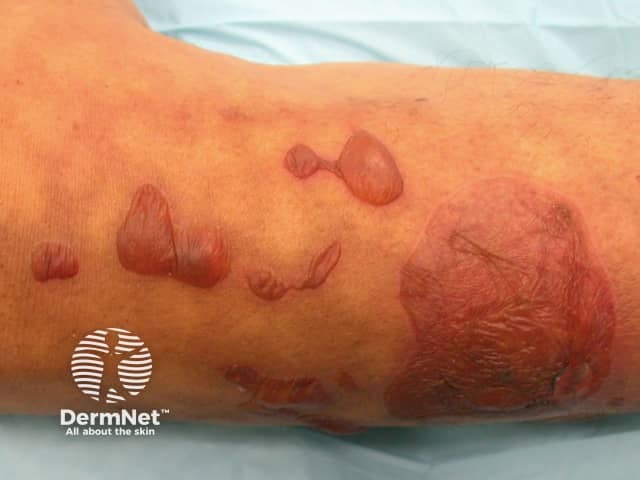
Burns from hot water bottle
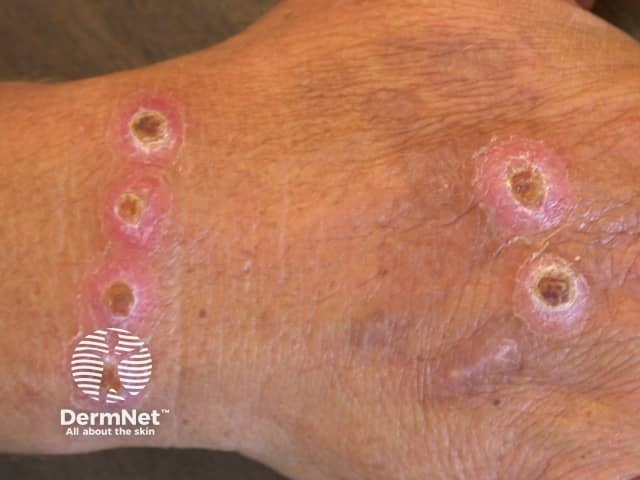
Cigarette burns
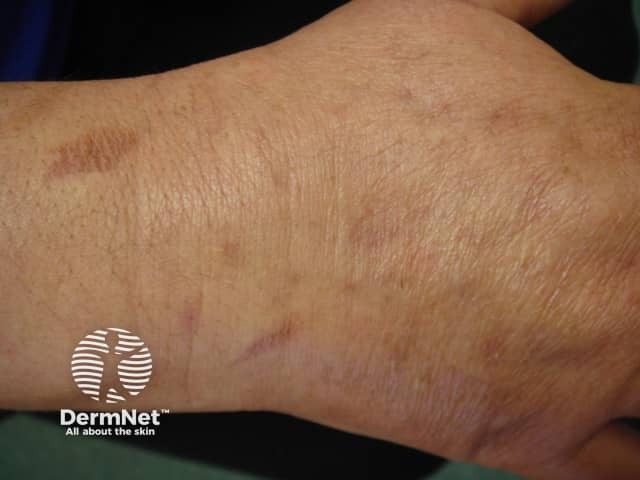
Oven burns
To understand the nature and classification of thermal burns it is necessary to have a brief understanding of how skin is made up. Basically, skin consists of an outer layer called the epidermis and an inner layer called the dermis. The epidermis consists of epithelial cells among which are the pigment-containing cells called melanocytes, which absorb some of the potentially dangerous UV rays in sunlight. The epidermis does not contain any blood vessels but is nourished via the blood vessels located in the dermis. Hence, the dermis is richly supplied with blood vessels, lymphatic vessels and nerves. It also contains hair follicles, sebaceous glands and sweat glands. Lying below the dermis is the hypodermis or subcutaneous fat tissue. This is not part of the skin but attaches the skin to underlying bone and muscle as well as supplying it with blood vessels and nerves.
Traditionally thermal injuries were classified as first, second or third degree burns. Nowadays many doctors describe burns according to their thickness (superficial, partial and full). The signs and symptoms experienced by a burn victim depend largely on the severity of the burn and the number of layers of skin that are affected.
The management of thermal burn involves several key steps.
Evaluating the total wellbeing of the burn patient is of paramount importance, particularly in patients with large burns. The primary aim is to ensure airway support, gas exchange and circulatory stability is achieved and maintained. Secondarily, a detailed history should be obtained from the patient to determine how the burn injury occurred. This may give clues for further examination, e.g. suspected carbon monoxide poisoning in individuals injured in structural fires.
Evaluation of the burn wound itself should only occur once the patient has been stabilised. The extent and depth of the burn will help guide decisions regarding wound care, inpatient or outpatient care, and monitoring.
Extent of burn
Depth of burn
Prompt diagnosis of infection of the burn wound is important to prevent further complication. Two burn wound infections are:
Any serious burns should be referred to a specialised burns unit, particularly those involving face, hands and genitalia. For less serious burns, management may be in the outpatient or inpatient setting.
Outpatient wound care strategies
Inpatient wound care strategies
The main treatment aims of burn wound management are:
Commonly used topical antibacterials include1% silver sulfadiazine cream, 0.5% silver nitrate solution and mafenide acetate 10% cream.