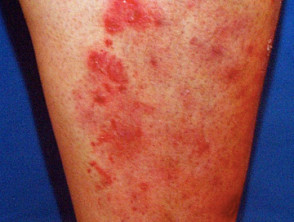
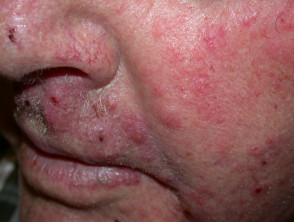
What is tinea incognito?
Tinea incognito is the name given to a fungal skin infection when the clinical appearance has been altered by inappropriate treatment, usually a topical steroid cream. It is also known as steroid-modified tinea. The result is that the original infection slowly extends and may mimic other skin disorders.
Often the patient and/or their doctor believe they have a dermatitis, hence the use of a topical steroid cream. The steroid cream dampens down inflammation so the condition feels less irritable. But when the cream is stopped for a few days the itch gets worse, so the steroid cream is promptly used again. The more steroid applied, the more extensive the fungal infection becomes and the less recognisable.
Tinea incognito was described by two UK dermatologists (Dr Adrian Ive and Dr Ronnie Marks), who later admitted that they should have correctly declined it as “tinea incognita”, as tinea is feminine. The majority of subsequent publications have followed this grammatical error.
Tinea incognita
What causes tinea incognito?
Tinea incognito is due to dermatophyte fungal infection (tinea), most often when it affecting the trunk and/or limbs (tinea corporis). Trichophyton rubrum is the most common organism to cause tinea corporis and tinea incognito in New Zealand.
Anti-inflammatory creams that can induce tinea incognito include:
- Topical steroids
- Tacrolimus ointment
- Pimecrolimus cream.
Tinea incognito can also be caused by systemic steroids.
Underlying diseases may predispose individuals to infection, especially:
Factors such as sweating, abrasion, and maceration also contribute to the development of infection.
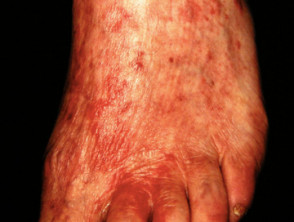
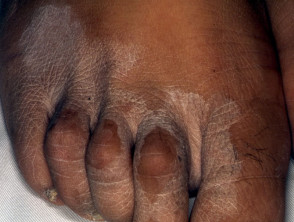
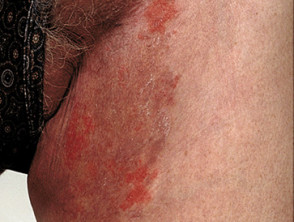
What are the clinical features of tinea incognito?
DermNet's page on tinea corporis describes its usual clinical features. Compared with an untreated tinea corporis, tinea incognito:
- Has a less raised margin,
- Is less scaly,
- More pustular,
- More extensive,
- And more irritable.
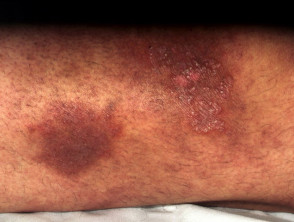
There may also be secondary changes caused by long term use of a topical steroid such as:
- Atrophy (thin skin, stretch marks (striae) in the skin folds).
- Purpura (bruising) and telangiectasia (broken blood vessels).
How is tinea incognito diagnosed?
The diagnosis of tinea is most easily made by taking skin scrapings for microscopy and culture a few days after stopping all creams.
- If there is little surface scale, the laboratory may report the specimen to be inadequate or negative.
- After stopping a steroid cream, tinea incognito becomes very inflamed and more fungal elements may be seen on microscopy than usual.
- The responsible organism generally grows promptly in culture.
If a skin biopsy is performed, the pathology of tinea incognito reveals the organisms.
What is the treatment of tinea incognito?
- Any topical steroid or calcineurin inhibitor should be discontinued.
- Bland antipruritic lotions can be applied.
- Standard antifungal treatment should be used.
Tinea is usually treated with topical antifungals (such as miconazole, ketoconazole, econazole), but is likely to require oral antifungal medicines such as terbinafine and itraconazole.
How can tinea incognito be avoided?
Tinea incognito can be avoided if:
- Patients do not use topical steroids to treat undiagnosed skin conditions
- Medical practitioners consider the diagnosis of dermatophyte infection in any scaly or pustular rash that has a prominent and irregular border, and is unilateral or asymmetrical in distribution
- Mycology is performed when in doubt about the diagnosis of a scaly or pustular rash.