What is a stasis ulcer?
A stasis ulcer is the most common cause of chronic full-thickness skin loss on the lower leg. As the name implies venous blood doesn’t flow properly from the leg back towards the heart. A stasis ulcer is also called venous leg ulcer, gravitational ulcer and varicose ulcer (although the latter is an inappropriate name when varicose veins are not present).
Who gets stasis ulcers?
Stasis ulcers affect 1% of the population, so they are not uncommon. A variety of medical problems and lifestyle factors have been linked to their development. These include:
- Increasing age
- Previous deep venous thrombosis (DVT) (a blood clot in the deep veins)
- Obesity
- Lower limb fracture, surgery or injury
- Immobility
- High blood pressure
- Standing upright for long periods
- Multiple previous pregnancies
- Varicose veins.
Stasis ulcers account for at least 40–50% of chronic lower limb ulcers and contribute to a further 20% of mixed arterial and venous ulcers.
What causes stasis ulcers?
Stasis ulcers are caused by:
- Venous insufficiency (poor return of venous blood from the peripheries to the central circulation)
- Venous hypertension (high pressures within the veins)
- Oedema (accumulation of fluid in the lower limbs).
Factors leading to venous insufficiency include:
- Venous obstruction from DVT or obesity
- Incompetence of the valves within the blood vessels
- Impaired calf pump.
When blood is unable to be efficiently returned to the heart:
- Fluid leaks from the engorged blood vessels into surrounding tissues.
- The vessel walls become fibrotic (thickened).
- There is reduced delivery of oxygen and nutrients to the tissues.
- There is impaired removal of metabolic waste products.
- The tissues become inflamed.
- Wound healing is impaired.
The result is an eventual skin breakdown, especially after an acute injury (which might be quite minor).
What are the clinical features of stasis ulcers?
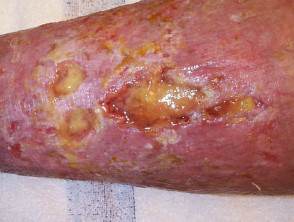
Characteristics of stasis ulcers include:
-
- Being located on the lower legs, commonly the inner ankle or ‘gaiter’ region
- Causing minimal pain
- A tendency to be shallow, with lots of exudate.
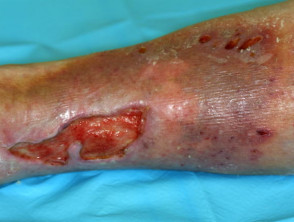
Stasis leg ulcers
Accompanying features confirming venous disease include:
-
- Ankle swelling
- Varicose veins
- Red-brown skin discolouration due to haemosiderin deposition resulting from the breakdown of red blood cells
- Dermatitis, either blistered and oozy, or dry and scaly, itchy skin
- Lipodermatosclerosis (thickened, woody tissues)
- Slow-growing, thick toenails.
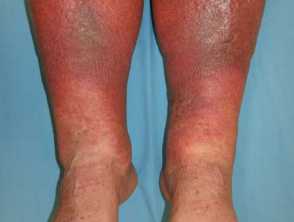
Complications of venous insufficiency
What are the complications of stasis ulcers?
The main complication of stasis ulcers is an infection. Wound infection can further impair the healing process. Bacteria colonise nearly all leg ulcers, but systemic antibiotics are not required unless clinical signs of infection are present. Signs that a stasis ulcer may require treatment with antibiotics include:
- Redness and swelling of the skin surrounding the wound
- Increasing warmth
- Increasing pain
- Increasing wound size
- Increasing purulent discharge from the wound
- Fever.
Topical antibiotics are not recommended because they slow the rate of wound healing, despite their bactericidal properties.
Cellulitis and venous insufficiency
How are stasis ulcers diagnosed?
Stasis ulceration is usually a clinical diagnosis, made on the basis of the patient's history and examination findings, and includes the presence of risk factors for venous stasis, that is, congestion and slowing of venous circulation, and the characteristic features of the wound and surrounding tissues.
- Duplex ultrasonography is used to confirm venous obstruction or valvular incompetence prior to saphenous vein ablation surgery
- Concomitant arterial disease is identified using the ankle-brachial index (ABI)
Other investigations to evaluate venous insufficiency and provide haemodynamic information may include:
- Intravenous ultrasonography
- Ascending or descending venography/phlebography (direct contrast, magnetic resonance)
- Venous air plethysmography
- Photoplethysmography
- Lymphoscintigraphy
- Liquid crystal thermography
- Ambulatory venous pressure measurements
- Arm-foot pressure differential tests
- Venous function tests
- Haematological studies of the coagulation system.
What is the treatment for stasis ulcers?
The treatment for stasis ulcers aims to address the underlying cause, provide symptomatic relief, and promote wound healing.
General measures
- Aim for weight reduction if the individual is overweight.
- Advise the individual to increase exercise to aid circulation.
- Reduce leg swelling by getting the individual to elevate the leg above the level of the heart as frequently as possible, a minimum of 30 minutes, three times daily.
Compression
Compression is a mainstay of treatment for stasis ulcers.
- Compression (eg, four-layer elastic bandaging) helps heal stasis ulcers, limits leg swelling and provides symptomatic relief.
- Compression stockings are less effective in the treatment of established ulcers but are useful for wound prevention.
Local wound care
Adequate wound care involves keeping the wound clean and moist with regular dressing changes.
- Debridement is used to remove dead tissue along the borders of the wound and excessive slough from the wound bed.
- Treat venous eczema with topical steroids and regular emollients.
Medical and surgical treatment
Oral medications that affect blood flow, particularly aspirin, provide some benefit in promoting the healing of stasis ulcers.
Surgical interventions may help stasis leg ulcers heal and prevent their recurrence.
- Superficial vein ablation reduces the backflow of blood from deep penetrating veins to superficial leg vessels; see leg vein therapies.
- Skin grafting may be required for stable, uninfected, large stasis ulcers who have not shown improvement with other measures.
In the case of a resistant stasis ulcer, other therapies may be tried, including:
- Hyperbaric oxygen therapy
- Medications that cause venous constriction, including flavonoids
- Medications that affect blood flow, such as pentoxifylline
- Therapeutic ultrasound and electromagnetic therapy.
What is the outcome for stasis ulcers?
Stasis leg ulcers are chronic and may persist for a few months to many years. Once they have healed, there is a high likelihood that stasis ulceration will recur, unless the underlying venous insufficiency is effectively treated.