What is zika virus?
Zika virus causes an infection that is mainly spread by the bite of tropical zika virus-carrying mosquitoes. It presents as a flu-like illness rather similar to dengue fever, but not as severe. An itchy rash is a prominent feature. It also causes neurological symptoms due to small fibre neuropathy.
Birth defects have been reported after zika infection of pregnant women. Pregnant women should take special precautions if travelling to affected areas. See Question and Answers: Zika virus infection (Zika) and pregnancy (CDC).
Who gets zika virus infection?
Zika virus affects people that have travelled to affected tropical areas and have been bitten by a mosquito that carries the infection. It is estimated that only about one in five people carrying the virus actually develop symptoms from zika virus infection.
For current affected areas worldwide, see Zika-affected areas information on the US Center for Disease Control (CDC) website. New Zealand does not have the zika-virus-carrying mosquitoes, and to date, zika virus infection has only been reported in people that have recently travelled to an affected area. During 2014–2016, these have included the Pacific Islands, South East Asia, Central and South American countries.
What causes zika virus infection?
Zika virus infection is an arboviral illness (viruses transmitted by arthropods such as mosquitoes and ticks).
Where does zika virus come from and how is it spread?
Zika virus is a small, spherical, single-stranded enveloped RNA virus belonging to family Flaviviridae, genus Flavivirus.
Zika virus was first described in humans in the 1960s in Nigeria. It was first reported outside Africa in 2007 when a case was reported on the island of Yap in Micronesia. Possible factors for zika virus spread include:
- Overpopulation of areas leading to inadequate housing and public health systems (water, sewerage and waste management).
- Poor vector control, e.g., stagnant pools of water for mosquito breeding.
- Climate change (increased virus transmission has been linked to El Nino conditions).
- Increased international travel (recreational, business or military) to endemic areas.
The mosquito Aedes aegypti is the main Aedes species involved in transmitting the zika virus from infected individuals to healthy contacts. These mosquitoes breed in and around ponds of stagnant water where humans live and usually bite during daylight hours. When a human is infected the virus circulates the blood for 10 days before symptoms occur. It is during this time that the Aedes mosquito may acquire the virus, then bite and infect another unsuspecting victim.
Zika virus can be transmitted from an infected mother to a baby at the time of birth, or transmitted by sexual intercourse if the partner is infected.
What are the clinical features of zika virus infection?
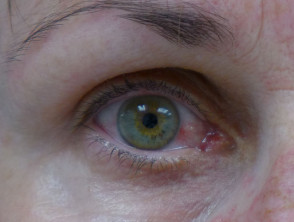
Zika virus infection arises about 10 days after a bite from an infected mosquito. It results in headache, mild fever, chills, conjunctivitis (red eyes), joint and muscle aches and an itchy rash. Other non-specific symptoms may include headache, fatigue, malaise, abdominal pain and vomiting.
Dysaesthesia (numbness, tingling) may occur, as well as autonomic symptoms such as dry mouth, dry skin, dry eyes and bladder incontinence.
Zika virus infection usually recovers within a week.
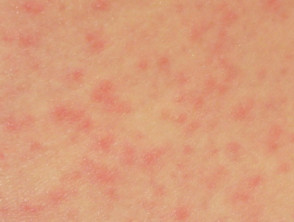
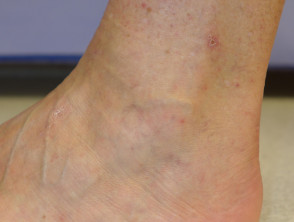
What does the zika virus rash look like?
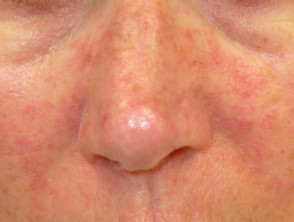
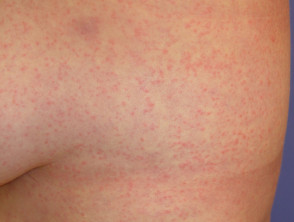
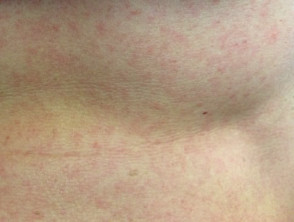
The rash associated with zika virus is either morbilliform (papules) or scarlatiniform (micropapules). It starts on the face on the first day of illness and spreads to trunk and limbs. The rash may affect palms and soles, which may be swollen. It begins to fade within 2–3 days and is gone completely within a week.
At the same time, the eyes become sore and red and may be sensitive to the light. Small red dots, petechiae, may be observed inside the mouth on the palate.
Zika virus infection
What are the complications of zika virus?
Guillain-Barré syndrome
Guillain-Barré syndrome is a rare, rapid-onset form of paralysis. It is an autoimmune syndrome and is often triggered by an infection a few days to weeks earlier. The first case of zika virus infection complicated by Guillain-Barré syndrome was reported from French Polynesia in March 2014, and others have occurred in Brazil. Death is rare.
For further information about Guillain-Barré syndrome, see Guillain-Barré Syndrome Fact Sheet, NIH National Institute of Neurological Disorders and Stroke.
Birth defects
The zika virus replicates and persists for several months in the placenta and in the brain tissue of a fetus. This results in an increase in fetal loss, growth retardation, and in birth defects in babies born to mothers infected with zika virus during pregnancy. Birth defects include:
- Fetal microcephaly (small head)
- Intracranial calcifications (calcium deposits in the brain)
- Brain damage
Pregnant mothers with suspected zika infection, or that have recently travelled to an infected zone, should see their doctor or midwife. They should undergo testing for the zika virus (see below). If the infection is confirmed, the CDC recommends serial ultrasound examination to monitor fetal growth and anatomy and referral to a maternal-fetal medicine or infectious disease specialist with expertise in pregnancy management. Amniocentesis may be considered after 15 weeks of gestation.
How is zika virus diagnosed?
Zika virus infection is diagnosed by typical clinical symptoms after a mosquito bite in an endemic area. The infection is confirmed by specific serological tests for zika virus immunoglobulins (IgG and IgM), which may need to be repeated 2–3 weeks later. New Zealand samples are tested at an Australian Arbovirus Reference laboratory. There is some cross-reactivity with tests for dengue viruses.
In New Zealand, zika virus infection is notifiable.
What is the treatment of zika virus infection?
There is no specific treatment available against zika virus infection.
Zika virus infection is usually self-limiting and resolves with supportive therapy. Paracetamol (acetaminophen) may be used to treat patients with fever. Aspirin and nonsteroidal anti-inflammatory drugs (NSAIDs) are not recommended. Drink plenty of fluids, and take rest.
People with a zika virus infection or who have recently had zika virus infection should not donate blood, as the virus could be transmitted to a recipient. They must also be careful to avoid mosquito bites to reduce spreading the disease to others.
How to prevent zika virus infection
The best way to prevent zika virus infections is by preventing the spread of the virus by vector control. This means eliminating or controlling mosquito breeding sites. The zika virus-carrying mosquito likes to breed in artificial containers and receptacles containing water in and near buildings. The following measures can be taken to reduce the breeding of mosquitoes.
- Cover tightly with a lid all water tanks, cisterns, barrels, rubbish containers, etc.
- Remove or empty water in old tyres, tin cans, bottles, trays, etc.
- Check and clean out clogged gutters and flat roofs where water may have settled.
- Change the water regularly in pet water dishes, birdbaths and plant trays.
- Introduce larvivorous fish (e.g., guppy) to ornamental water features as these eat the mosquito larvae.
- Trim weeds and tall grasses as adult mosquitoes seek these for shade on hot days.
People can do the following to prevent themselves from being bitten by mosquitoes.
- Wear long sleeves and pants.
- Install secure screens to windows and doors to keep mosquitoes out.
- Use an insect repellent such as DEET.
- Sleep under mosquito curtains or nets, this is particularly important when children are sleeping or resting during daylight hours.
- In high-risk areas, insecticide sprays may be used to kill mosquitoes.
- Children must be protected too.
Vaccines to prevent zika virus infection are in development.